
January 5th, 2015 by Dr. Val Jones in Health Tips, Research
Tags: Acetaminophen, Annals Of Internal Medicine, Celecoxib, Comparative Effectiveness, Corticosteroids, Diclofenac, hyaluronic acid, Ibuprofen, Knee OA, Osteoarthritis, What Works For Knee Pain?
No Comments »
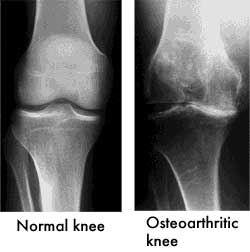 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
#1. Knee injection with gel (Rx hyaluronic acid)
#2. Knee injection with steroid (Rx corticosteroid)
#3. Diclofenac (Voltaren – Rx oral NSAID)
#4. Ibuprofen (Motrin – OTC oral NSAID)
#5. Naproxen (Alleve – OTC oral NSAID)
#6. Celecoxib (Celebrex – Rx NSAID)
#7. Knee injection with saline solution (placebo injection)
#8. Acetaminophen (Tylenol – OTC Synthetic nonopiate derivative of p-aminophenol)
#9. Oral placebo (Sugar Pill)
I found this rank order list interesting for a few reasons. First of all, acetaminophen and celecoxib appear to be less effective than I had believed. Second, placebos may be demonstrably more effective the more invasive they are (injecting saline into the knee works better than acetaminophen, and significantly better than sugar pills). Third, injection of a cushion gel fluid is surprisingly effective, especially since its mechanism of action has little to do with direct reduction of inflammation (the cornerstone of most arthritis therapies). Perhaps mechanical treatments for pain have been underutilized? And finally, first line therapy with acetaminophen is not clinically superior to placebo.
There are several caveats to this information, of course. First of all, arthritis pain treatments must be customized to the individual and their unique tolerances and risk profiles. Mild pain need not be treated with medicines that carry higher risks (such as joint infection or gastrointestinal bleeding), and advanced arthritis sufferers may benefit from “jumping the line” and starting with stronger medicines. The study is limited in that treatments were only compared over a 3 month trial period, and we cannot be certain that the patient populations were substantially similar as the comparative effectiveness was calculated.
That being said, this study will influence my practice. I will likely lean towards recommending more effective therapies with my future patients, including careful consideration of injections and diclofenac for moderate to severe OA, and ibuprofen/naproxen for mild to moderate OA, while shying away from celecoxib and acetaminophen altogether. And as we already know, glucosamine and chondroitin have been convincingly shown to be no better than placebo, so save your money on those pills. The racket is expected to blossom into a $20 billion dollar industry by 2020 if we don’t curb our appetite for expensive placebos.
In conclusion, the elephant in the room is that weight loss and exercise are still the very best treatments for knee osteoarthritis. Check out the American Academy of Orthopedic Surgery’s recent list of evidence-based recommendations for the treatment of knee arthritis for more information about the full spectrum of treatment options.
December 12th, 2014 by Dr. Val Jones in Expert Interviews, Health Tips
Tags: Apps, Empowered Patients, EMR, Health Outcomes, Mobile Health, Poverty, Texting, The American Resident Project
1 Comment »
 I am proud to be a part of the American Resident Project, an initiative that promotes the writing of medical students, residents, and new physicians as they explore ideas for transforming American health care delivery. I recently had the opportunity to interview three of the writing fellows about how to help patients take control of their health. Dr. Marissa Camilon (MC) is an emergency medicine resident at LA County USC Medical Center, Dr. Craig Chen (CC) is an anesthesiology resident at Stanford Hospitals and Clinics, and Dr. Elaine Khoong (EK) is a resident in internal medicine at San Francisco General Hospital. Here’s what they had to say:
I am proud to be a part of the American Resident Project, an initiative that promotes the writing of medical students, residents, and new physicians as they explore ideas for transforming American health care delivery. I recently had the opportunity to interview three of the writing fellows about how to help patients take control of their health. Dr. Marissa Camilon (MC) is an emergency medicine resident at LA County USC Medical Center, Dr. Craig Chen (CC) is an anesthesiology resident at Stanford Hospitals and Clinics, and Dr. Elaine Khoong (EK) is a resident in internal medicine at San Francisco General Hospital. Here’s what they had to say:
1. How would you characterize the patients who are most successful at “taking charge of their health?”
MC: They are usually the the patients who aren’t afraid to ask questions about everything- possible treatments, pathology, risk factors.
EK: I think there are several traits that make patients successful at modifying their health: 1) Understanding of their disease: patients need to understand how their actions impact their health and be able to clearly identify the steps they need to take to achieve their desired health. 2) Possessing an internal locus of control: patients need to feel that their health is actually in their control. Oftentimes, patients who come from families that have a history of chronic diseases simply assume certain diseases may be their fate. But in reality, there are things that can be done to manage their disease. 3) Living in a supportive, nurturing environment: behavior changes are difficult. It is often not easy to the right thing for your health. Patients that take control of their health have a support system that helps ensure they take the steps they need. 4) Having realistic expectations: improving your health takes time and thus it requires patience. Individuals must be able to identify the baby steps that they’ve taken towards improving their health.
CC: Patients must collaborate with their physician – the best patients come in motivated, knowledgeable, and educated so they can have a meaningful dialogue with their doctor. Medical decision making is a conversation; patients who are invested in their health but also open to their doctor’s suggestions often have the best experiences.
2. What do you see as the main causes of non-adherence to medical advice/plans?
MC: Not fully understanding his or her own disease process, denial/shock, inability to pay for appointments/rides/medications.
EK: I think there are several reasons that patients may be non-adherent. These reasons can largely be grouped into three main categories — knowledge, attitude, and environmental factors. Some patients simply don’t understand the instructions provided to them. Providers haven’t made it clear the steps that need to be taken for patients to adhere. In other cases, patients may simply not believe that the advice provided will make an impact on their health. Probably most frequently, there are environmental factors that prevent patients from adhering to plans. Following medical advice often requires daily vigilance and strong will power. The challenges of daily life can make adherence difficulty.
CC: In my mind, non-adherence is not a problem with a patient, but instead a problem with the system. Modern medicine is a complex endeavor, and patients can be on a dozen different medications for as many medical problems. It’s unreasonable to expect someone to keep up with that kind of regimen. Socioeconomic factors also play a big role with adherence. Patients who are poor struggle to maintain housing, feed their children, hold a job; how can we expect them to be perfectly medically compliant? Tackling the issue of non-adherence requires engagement into the medical and social factors that pose challenges for patients.
3. Could mobile health apps help your patients? Do you think “there’s an app for that” could revolutionize patient engagement or your interaction with your patients now or in the future?
MC: Apps, not necessarily. Most of patient population has limited knowledge of their mobile phones (if they even have mobile phones). If they do have a phone, its usually an older model that doesn’t allow apps.
EK: I absolutely think that mobile health apps could help my patients. I work at a clinic for an urban underserved population. For patients that work multiple part-time jobs to make ends meet, it is difficult to ask them to come into see a healthcare provider (particularly if the commute to see us requires 2+ bus rides). Unfortunately the patients who are working multiple jobs are often patients in their 40’s and 50’s when they start manifesting the early signs and symptoms of our most common chronic diseases (hypertension, diabetes, and cardiovascular disease). Mobile applications have great potential to simplify the way through which patients can receive medical guidance especially helping the patients who don’t have the luxury to seek medical advice during normal work hours.
CC: I think there is a role for technology in the delivery of modern medical care. However, we have to keep in mind that not everyone has access to smartphones, and often the most medically disadvantaged populations are those who need support the most. Although initially, technology seemed to put a barrier between the clinician and the patient, I think as devices become more prevalent and we become better at using them, we’ll be able to use these collaboratively. The main advantage of an “app” or device is giving the patient more control over their health; they can track their sleep, diet, exercise, medication adherence, and other aspects of their health and work with their doctor to optimize it.
4. Do you know of any programs to improve health literacy that have been particularly successful or innovative? If so, describe. If not, what kind of initiative do you think could make a difference for your patients?
MC: I know that some of the primary care clinics in the county have started using texting for appointments reminders. Texting seems to be more accessible to our county population.
EK: Unfortunately, off the top of my head, I cannot think of any great programs that have increased health literacy. Part of the reason for this is that we really don’t have a great sense of what levers increase literacy. Any initiative that will work best honestly depends on the individual patient — each patient has different barriers that limit their health literacy. For some patients, their limited English proficiency is the greatest barrier. For other patients, there are cultural beliefs that must be considered in delivering health content. And for some patients, numeracy or general literacy is an issue. Unfortunately, I think there is no one size fits all solution for addressing health literacy.
CC: I don’t think there’s any magic bullet for health literacy. Different communities, patient populations, and clinical settings merit different interventions. For example, tackling child obesity in a neighborhood with lots of fast food requires a different program than ensuring prenatal health in an immigrant community.
5. Are there generational differences in how your patients interact with the healthcare system? Describe.
MC: I tend to see older patients since they usually have more medical problems. They are more likely to have a primary care doctor; whereas younger patients don’t come in as often, but don’t usually have access to primary care.
EK: I think more than a generational difference there is actually a cultural and socioeconomic difference. Traditionally, we are taught or somehow led to believe that older patients are more likely to simply adhere to medical advice whereas younger patients question. But in my limited experience, I have seen affluent patients more engaged with providers (bringing in their own resources, asking about health advice they’ve heard or read about). Some of my less wealthy patients seem more passive about their health and during visits. Furthermore, patients from certain cultural backgrounds are more or less likely to view healthcare providers as an authoritative figure rather than a partner in shared decision making.
6. Do you use digital systems (EMR/Social Media/Mobile) to interact with your patients in any way? Do you think you should do more of that, or that there is a desire for more on the part of your patients?
MC: We do have an EMR but don’t really use it to interact with patients. As I mentioned before, mobile texting may encourage patient interaction.
EK: The main way that I currently use digital systems to interact with patients is via email. Our clinic has a somewhat difficult-to-navigate telephone prompt system, so some patients email me directly re: changing their appointments, medical advice, or medication refills. Unfortunately our EMR doesn’t currently have a patient portal (although it will be rolling this out soon). I think a patient portal is a great tool for helping patients stay more engaged in their healthcare.
I think there is a role for SMS messaging to remind patients about appointments, important medications, or other healthcare related notices. For the right patient population, I think this could make a big difference.
In general, I am a big proponent of technology. I don’t think it’s going to be a panacea for our many problems in the healthcare system, but I think there are very specific shortcomings that technology can help us address.
7. What would your patients say they needed in order to be better educated about their health and have more successful healthcare experiences?
MC: More time with their physicians, mainly.
EK: Almost certainly simply more time with healthcare providers to better explain their health issues as well as more time to explore shared decision making.
CC: There is a lot of information out there about common illnesses and diseases, but not all of it is accurate or up-to-date. One challenge for patients is identifying appropriate resources written in a manner that can be easily read and understood with content that has been reviewed by a physician or other health care expert.
8. If you could pick only 1 intervention that could improve the compliance of your patients with their care/meds, what would it be?
MC: Increase the amount of time physicians have to answer questions with patients and discuss medical treatment options with them.
EK: Wow, that’s a hard one. I struggle to answer questions like this because I strongly believe that each patient is so different. Any non-adherent patient has his or her own barrier to adherence. But I suppose if I had to pick something, it might be some form of weekly check-in with a health coach / community health worker / health group class that intimately knew what the most important steps would be to helping that one patient ensure better health.
CC: I think that social interventions make the most difference in the health of underserved populations. For example, stable housing, healthy meals, job security, and reduction in violent crime will improve health including medical compliance far more than any medicine- or technology-based intervention.
December 1st, 2014 by Dr. Val Jones in Health Tips, Opinion
Tags: Change Of Shift, Medical Errors, Medical Rounds With Nurses, Nurses, Physician Communication, Rounds, Signout, Team Rounds
1 Comment »
 Whenever possible I make a point of rounding on patients with their nurses present. I rely on nurses to be my eyes and ears when I’m not at the bedside. I need their input to confirm patient self-reports of everything from bowel and bladder habits to pain control, not to mention catching early warning signs of infection, mental status changes, or lapses in safety awareness. Oftentimes patients struggle to recall bathroom details, and they can inadvertently downplay pain control needs if they don’t happen to be in pain when I visit them. A quick check with their nurse can clarify (for example) that they are asking for pain medicine every 2 hours, that they have missed therapy due to somnolence, that their wound incision looks more red, and/or that they haven’t had a bowel movement in a dangerously long time. All critical details that I wouldn’t necessarily know from talking to the patient alone. Some of this information is not accurately captured in the electronic medical record either.
Whenever possible I make a point of rounding on patients with their nurses present. I rely on nurses to be my eyes and ears when I’m not at the bedside. I need their input to confirm patient self-reports of everything from bowel and bladder habits to pain control, not to mention catching early warning signs of infection, mental status changes, or lapses in safety awareness. Oftentimes patients struggle to recall bathroom details, and they can inadvertently downplay pain control needs if they don’t happen to be in pain when I visit them. A quick check with their nurse can clarify (for example) that they are asking for pain medicine every 2 hours, that they have missed therapy due to somnolence, that their wound incision looks more red, and/or that they haven’t had a bowel movement in a dangerously long time. All critical details that I wouldn’t necessarily know from talking to the patient alone. Some of this information is not accurately captured in the electronic medical record either.
On a recent trip to a new facility, I asked the head nurse when change of shift occurred. She was visibly perplexed and asked why I wanted to know. I explained that I planned to attend nursing sign out so that I’d be up to date on how my patients were doing. She raised her eyebrows to their vertical limit and responded, “I haven’t seen a doctor do nursing rounds in 30 years.”
That was one of the saddest things I’d heard in a long time. How is it that one of the fundamental features of medical care (doctors and nurses visiting patients together) has gone the way of the dinosaur? Most of my colleagues say they don’t round with nurses because they “don’t have time for that stuff” or that they can “flag down a nurse when there’s an issue” without needing scheduled communication. While I can sympathize with the fear of yet another “time suck” during a busy hospital day, I believe that rounding with nurses can actually save time, reduce medical errors, and head off developing problems at earlier stages (e.g. wound infections, intestinal obstructions, delirium, over/under medication and unwanted medication side effects).
You may think that coordinating nursing rounds with medical rounds is an insurmountable logistical nightmare, and if you have patients scattered throughout various floors of a hospital, that will certainly make things more difficult. But I have found ways to overcome these barriers, and highly recommend them to my peers:
1. Attend nursing sign out at change of shift if possible. Do not disrupt their hand-off process, but ask for clarification (or offer clarification) at key points during patient presentation.
2. Listen to the change of shift recording. Some nurses have their night shift team record their observations and findings in lieu of a 1:1 hand-off process during busy morning hours. This has its advantages and disadvantages. The good thing is that relaying information becomes asynchronous (i.e., like email vs a phone call – you don’t have to be present to get the info), the bad thing is that you can’t ask for clarification from the person delivering the information. If the nurses know in advance that the patient’s doctor is also listening in, they will leave targeted medical questions and concerns for you on the recording.
3. Do your rounds at times when medications are most commonly delivered. You will be more likely to run into a nurse in the patient’s room and can coordinate conversations as well as perform skin checks together.
4. Communicate with nurses (between rounds) when you are about to order a series of tests or dramatically change medication regimens. Explain why you’re doing it so they will be able to plan to execute your orders more efficiently (i.e. before the patient leaves for a radiologic study, etc.) This open communication will be appreciated and will be reciprocated (and may help to spark interest in joining you for regular rounds).
5. Invite nurses to round with YOU. If you can’t join their change of shift, consider having them join your medical rounds. You’ll need to negotiate this carefully as the goal is to streamline rounding processes, not double them.
A recent study published in the New England Journal of Medicine described a sign out process that reduced medical errors by 30%. This communication strategy involved 1:1 transfer of information about patients in a structured team environment (including nurses in some physician meetings). I anticipate that further investigation will reveal that interdisciplinary rounding (with nurses and doctors together) is a critical piece of the error reduction process. For all our advances in technology and digital information tracking, “old school” doctor-nurse rounds may prove to be more important in reducing errors and keeping our patients safe than other far more costly (and exasperating) interventions.
November 13th, 2014 by Dr. Val Jones in Health Tips, Opinion
Tags: Conversation Interruption, History And Physical Exam, Interruptions, Physicians, Rudeness
3 Comments »
 Much has been made about physicians’ tendencies to interrupt patients. Studies have shown that patients are permitted 12-18 seconds of talk time before they are redirected (or interrupted) by their doctor. This leads to patients feeling that the physician didn’t listen or didn’t care. I believe that there is a way to solve the problem without wasting time or being rude. I have used this technique with great success over the years and it works especially well in the inpatient setting, when beginning a formal “history and physical exam.” In three simple words:
Much has been made about physicians’ tendencies to interrupt patients. Studies have shown that patients are permitted 12-18 seconds of talk time before they are redirected (or interrupted) by their doctor. This leads to patients feeling that the physician didn’t listen or didn’t care. I believe that there is a way to solve the problem without wasting time or being rude. I have used this technique with great success over the years and it works especially well in the inpatient setting, when beginning a formal “history and physical exam.” In three simple words:
Physician goes first.
Before I enter the patient’s room, I perform a careful review of their medical records and imagine what it must have been like for them to experience the events leading up to our meeting. I reconstruct the emotional time line in my head and figure out which pieces of information I need to complete my assessment and plan. Then when I meet the patient (often for the first time) I begin by greeting them warmly and then telling them what I have gleaned from their medical records, and how I think they may have felt during the process leading up to their hospitalization. This establishes that I have taken the time to get to know their background, that I genuinely care about how they’ve been dealing with things emotionally, and that I am determined to correct the record if there are any gaps or errors. I then rely on the patient to fill in the details or clarify results that are unclear.
This strategy saves the patient from having to review historical information that the physician already knows about (which usually leads to the classic interruption at second 12-18 of the interaction), and provides structure for patient participation and input. It establishes trust with the new physician, and conveys empathy. It corrects the medical record when necessary, and maximizes the efficiency of the information exchange. To drive home the concept, let me provide you with two hypothetical conversations with “Mrs. Smith” – in the first case the physician will approach her in the traditional manner, and in the second, with the “physician goes first” method.
Establishing the “chief complaint” with Mrs. Smith – Traditional method
Dr. Jones: (entering hospital room where Mrs. Smith is sitting alone in her bed in no acute distress): “Good morning, Mrs. Smith. I’m Dr. Jones, the attending physician for this unit. What brings you here today?”
Mrs. Smith: (eyeing Dr. Jones with some degree of confusion). “Well, I just had surgery, and I guess I’m still a bit weak so they said I needed to come to rehab but I still don’t really understand why I had to change rooms. Did you know I had surgery? Yes, I was walking my dog on the sidewalk and he pulled a little too hard to lurch at a squirrel and the next thing I knew I was on the ground and my hip was hurting and I was all scraped up and I saw this man in the distance who started running towards me and then I think I passed out and when I got to the hospital, I don’t know, they were worried I had a seizure and then they did a CAT scan and then when I….”
Dr. Jones: “I see. But what I need to know from you now is what is your chief complaint. In other words, why are you here in the rehab unit?”
Mrs. Smith: “Well aren’t you the doctor? You’re supposed to tell me what to do when I’m here aren’t you?”
Dr. Jones: “Yes, of course. But I was hoping you could tell me in your own words.”
Mrs. Smith: Sighs heavily. “Well, I’m here because I fell down and broke my hip and then they found out that I hit my head too and then I guess they were trying to figure out if they needed to put a drain in or just give me seizure pills and I’m not sure how they decided but I don’t remember a drain so I guess… Isn’t all this in my records somewhere? Can’t you figure out what happened?”
Dr. Jones: “Yes, it’s all in your chart but…”
Mrs. Smith: “Well then why don’t you just read it instead of asking a poor old lady with a bad headache to tell you what happened all over again. Everyone keeps asking me for the same old story and I’m just so tired…”
Dr. Jones: “So you’re here in rehab because you’re tired?”
Mrs. Smith: “Well, I guess that’s it.”
Establishing the chief complaint with Mrs. Smith – “Physician goes first” method:
Dr. Jones: “Hello Mrs. Smith, I’m Dr. Jones, the rehab physician who will be taking care of you on this floor. I read through your chart very carefully and learned that you fell down on the sidewalk when walking your dog about a week ago. It looks as if you broke your hip as well as hit your head during the fall. I see that you had your hip repaired surgically, and that fortunately you didn’t need any treatment for your head injury because it didn’t bleed very much internally, but as a precaution you were given some anti-seizure medicine. I imagine that this sudden hospitalization was an unwelcome surprise for you – there you were just walking your dog on a normal day, minding your own business and whammo – now you’re here in the hospital with me!? Well, my goal is to get you back home as soon as you’re ready and steady enough. What is your main goal for rehab?”
Mrs. Smith: “Yes, well it certainly was a shock to get the wind knocked out of me. You hear about little old ladies falling down and breaking a hip but I never thought it could happen to me. Now all I need to do is be able to walk safely so I can go home.”
Dr. Jones: “Well, the good news is that you were very active prior to your fall so I bet you’ll do very well here because you have a good baseline fitness level. My goal is to help control your pain so you can make the fastest gains possible. I bet your hip bothers you and you may have headaches too.”
Mrs. Smith: “Yes, well that’s just it. I’m in quite a bit of pain when I stand up but I’m afraid of becoming a drug addict so I try not to take the pills…”
As you can see, the second conversation was much more successful in establishing a relationship with the patient and getting to the meat of what the doctor needs to know (the patient’s primary goal, her pain level, and what the barrier to treatment might be) without the frustration caused by traditional “open ended questions” and lack of structure – leading to interruptions and perceived lack of caring on the part of the physician.
In my experience, doing a little up front chart review and taking the lead in the first patient encounter results in a dramatic decrease in wasted time and need for redirection. So in the case of avoiding rude patient interruptions – taking the conversation lead may be the best bet.
This is an unusual case where putting the patient first involves letting them talk second.
November 3rd, 2014 by Dr. Val Jones in Health Tips, Opinion
Tags: Dangers, Electronic Medical Records, EMR, EPIC, Excessive Complexity, fail, Hospital Pharmacists, Medical Errors, Medication Errors, Medication Reconciliation, Pharmacists
214 Comments »
 Most hospitalized patients and families don’t realize that life-threatening medication errors are regularly thwarted by pharmacists. They are truly the unsung heroes of patient care. I just finished a locum tenens assignment at a hospital that uses EPIC as their electronic medical records system, and I was stunned by the impossibly complex medication reconciliation process. Each time a patient is admitted to the hospital, or transferred to another part of the hospital, a physician must review, approve, and re-order their medications. While this may seem like a good way to insure that medication errors are avoided, it actually has the exact opposite effect.
Most hospitalized patients and families don’t realize that life-threatening medication errors are regularly thwarted by pharmacists. They are truly the unsung heroes of patient care. I just finished a locum tenens assignment at a hospital that uses EPIC as their electronic medical records system, and I was stunned by the impossibly complex medication reconciliation process. Each time a patient is admitted to the hospital, or transferred to another part of the hospital, a physician must review, approve, and re-order their medications. While this may seem like a good way to insure that medication errors are avoided, it actually has the exact opposite effect.
Because EPIC keeps lists of home meds, discontinued meds, and current meds available for review and reactivation, it takes little more than one misplaced check box to order the wrong dose or type of medication. Physicians who transfer a patient to another service can indicate their intended medication list and keep it “on hold” for the receiving physician to review and approve. Unfortunately, the software’s tab system is so complex that it’s extremely difficult to find that list and activate it. Lost in a sea of admissions tasks and order boxes in different fonts, colors, and drop down menus, one often accidentally reviews and approves discontinued types and doses of medicines. The only protection against such errors is the hospital pharmacist.
With each new admission to the inpatient rehabilitation unit, I had to resort to calling a pharmacist for help. I was terrified that I would accidentally insert medication errors into the patient’s order set by carrying forward discontinued meds. The long-suffering pharmacists explained to me that “most physicians make medication order errors in EPIC with each admission.” They said that they regularly had to talk physicians out of throwing their computer out the window in a state of extreme frustration. They also said that their EPIC user environment looked very different (and less confusing) than what the physicians used, so that they couldn’t even provide real-time phone guidance regarding order entry process.
The scary thing is that EPIC has the largest market share of any EMR in the United States. It is also (in my experience) the most prone to medical errors due to its overly complex medication reconciliation process. I have used other EMRs that have far simpler and more intelligent medication order entry processes. Soarian (Sieman’s EMR, just sold to Cerner) has, for example, an outstanding order entry system. So my complaint is not that “all EMRs are bad” – it’s that some have particularly flawed designs that are causing real harm to untold millions of patients. We just haven’t documented the harm yet. I tremble at the thought of what we’d find.
Until electronic medication reconciliation is made safer, pharmacists will be working overtime to correct records and protect patients from carry over errors. I thank my lucky stars that I have had vigilant, determined pharmacists by my side as I cared for very complex, sick patients who were exceptionally vulnerable to dosing errors. There has never been a more important time to exercise caution when entering hospital medication orders, or to express your appreciation for pharmacists. Without their help we might all be experiencing medication errors of EPIC proportions.
 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:


 I am proud to be a part of the
I am proud to be a part of the 
 Whenever possible I make a point of rounding on patients with their nurses present. I rely on nurses to be my eyes and ears when I’m not at the bedside. I need their input to confirm patient self-reports of everything from bowel and bladder habits to pain control, not to mention catching early warning signs of infection, mental status changes, or lapses in safety awareness. Oftentimes patients struggle to recall bathroom details, and they can inadvertently downplay pain control needs if they don’t happen to be in pain when I visit them. A quick check with their nurse can clarify (for example) that they are asking for pain medicine every 2 hours, that they have missed therapy due to somnolence, that their wound incision looks more red, and/or that they haven’t had a bowel movement in a dangerously long time. All critical details that I wouldn’t necessarily know from talking to the patient alone. Some of this information is not accurately captured in the electronic medical record either.
Whenever possible I make a point of rounding on patients with their nurses present. I rely on nurses to be my eyes and ears when I’m not at the bedside. I need their input to confirm patient self-reports of everything from bowel and bladder habits to pain control, not to mention catching early warning signs of infection, mental status changes, or lapses in safety awareness. Oftentimes patients struggle to recall bathroom details, and they can inadvertently downplay pain control needs if they don’t happen to be in pain when I visit them. A quick check with their nurse can clarify (for example) that they are asking for pain medicine every 2 hours, that they have missed therapy due to somnolence, that their wound incision looks more red, and/or that they haven’t had a bowel movement in a dangerously long time. All critical details that I wouldn’t necessarily know from talking to the patient alone. Some of this information is not accurately captured in the electronic medical record either. Much has been made about physicians’ tendencies to interrupt patients.
Much has been made about physicians’ tendencies to interrupt patients.  Most hospitalized patients and families don’t realize that life-threatening medication errors are regularly thwarted by pharmacists. They are truly the unsung heroes of patient care. I just finished a
Most hospitalized patients and families don’t realize that life-threatening medication errors are regularly thwarted by pharmacists. They are truly the unsung heroes of patient care. I just finished a 









