October 8th, 2011 by John Mandrola, M.D. in Health Tips, Opinion
No Comments »

I recently wrote about the incredible sensations that come with vigorous exercise. Perhaps it was the post ride cannabinoid flurry, but it’s possible that I went too far in suggesting that ‘we’ (doctors, patients, the whole of Western Society) default first to pills before healthy living.
Two commentors called me out on this snark. They wrote about valid points.
One comment focused on the fact that her AF medicines were causing side effects that made vigorous exercise difficult. The second objected to my inference that exercise alone could substitute for the many benefits of modern medicine.
To the idea that medicine Read more »
*This blog post was originally published at Dr John M*
July 28th, 2011 by AndrewSchorr in Health Tips, True Stories
No Comments »

You know I am a cancer survivor – 15 years down the road from a leukemia diagnosis and enjoying a 10 year remission. So whenever something seems weird about my health it’s cancer coming back, right? Wrong! Just how wrong was proven last night. I am writing this from my hospital bed in Seattle.
 The first symptom of a possible problem came three days ago when I had soreness in my right calf. A pulled muscle? Maybe. But I had not noticed straining it. Back at the gym the next day I had soreness again but thought it was no big deal. Last night it was worse. It hurt some to walk. I got home and, after my wife and son were asleep, got ready for bed. I had a slight fever and then noticed the right calf was not only sore, but swollen and warm. Very strange. I’d never seen that before.
The first symptom of a possible problem came three days ago when I had soreness in my right calf. A pulled muscle? Maybe. But I had not noticed straining it. Back at the gym the next day I had soreness again but thought it was no big deal. Last night it was worse. It hurt some to walk. I got home and, after my wife and son were asleep, got ready for bed. I had a slight fever and then noticed the right calf was not only sore, but swollen and warm. Very strange. I’d never seen that before.
Trying not to be stupid I called the 24-hour consulting nurse. She immediately began to focus on deep vein thrombosis (DVT), a worrisome condition that affects about two million Americans a year and can lead to a life threatening situation. She had a doctor call me. Normally those doctors would rather make a house call then send you to the more costly emergency room. But not this time. “Dr. Steve” urged me to go to the ER rather than let a DVT progress and endanger my life. An ultrasound exam would determine if it was really a DVT. Read more »
*This blog post was originally published at Andrew's Blog*
July 24th, 2011 by John Mandrola, M.D. in Opinion, Research
No Comments »

I recently came across a very important blog post on the use of the novel new blood-thinner, dabigatran (Pradaxa).
Fellow Kentucky cardiologist, and frequent TheHeart.org contributor, Dr. Melissa Walton-Shirley wrote this very detailed case presentation involving a cantankerous non-compliant rural patient with AF (atrial fibrillation) that sustained a stroke while “taking” dabigatran.
Dr. Walton-Shirley details the very commonly done procedure of cardioversion (shock) for AF. As she clearly points out, the most important safety feature of shocking AF back to regular rhythm entails adequate blood thinning before and after the procedure. Thin blood prevents the possibility of clots dislodging after restoring normal contraction to the top chambers of the heart (atria).
Herein lies the rub with dabigatran, and the two soon-to-be-approved non-warfarin blood-thinning agents, apixaban and rivaroxaban. In the past, Read more »
*This blog post was originally published at Dr John M*
December 28th, 2010 by RyanDuBosar in Opinion, Research
No Comments »

This is a guest post by Dr. Juliet Mavromatis:
**********
The emergence of a new generation of anticoagulants, including the direct thrombin inhibitor, dabigatran and the factor Xa inhibitor, rivaroxaban, has the potential to significantly change the business of thinning blood in the United States. For years warfarin has been the main therapeutic option for patients with health conditions such as atrial fibrillation, venous thrombosis, artificial heart valves and pulmonary embolus, which are associated with excess clotting risk that may cause adverse outcomes, including stroke and death. However, warfarin therapy is fraught with risk and liability. The drug interacts with food and many drugs and requires careful monitoring of the prothrombin time (PT) and international normalized ratio (INR).
Recently, when I applied for credentialing as solo practioner, I was asked by my medical malpractice insurer to detail my protocol for monitoring patients on anticoagulation therapy with warfarin. When I worked in group practice at the Emory Clinic in Atlanta I referred my patients to Emory’s Anticoagulation Management Service (AMS), which I found to be a wonderful resource. In fact, “disease management” clinics for anticoagulation are common amongst group practices because of the significant liability issues. Protocol based therapy and dedicated management teams improve outcomes for patients on anticoagulation with warfarin. Read more »
*This blog post was originally published at ACP Hospitalist*
January 4th, 2010 by Toni Brayer, M.D. in Better Health Network, Health Policy, True Stories
1 Comment »

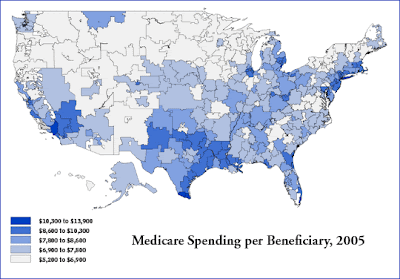 It has been proven than there is tremendous variation in the practice of medicine across the United States. The Dartmouth data (Wennberg et al) has documented the differences in how medical resources are used and how different physicians practice medicine, depending upon where they live. The Dartmouth studies are mainly focused on cost and outcomes and make the case that improved quality is often inversely related to the cost of care. More (expensive) care is not necessarily better care.
It has been proven than there is tremendous variation in the practice of medicine across the United States. The Dartmouth data (Wennberg et al) has documented the differences in how medical resources are used and how different physicians practice medicine, depending upon where they live. The Dartmouth studies are mainly focused on cost and outcomes and make the case that improved quality is often inversely related to the cost of care. More (expensive) care is not necessarily better care.
Now that I am recovering from a total joint replacement, I am amazed to see the differences in how physicians, doing the same surgery, treat the patient. Total knee replacement (TKA) is one of the most common orthopedic procedures done today. Despite this, the patient cannot expect the same post op care. Read more »
*This blog post was originally published at EverythingHealth*


















