December 23rd, 2011 by Jessie Gruman, Ph.D. in Book Reviews, Health Policy
No Comments »

 My friend and former Chair of the CFAH Board of Trustees, Doug Kamerow, has written a book that I think you will like.
My friend and former Chair of the CFAH Board of Trustees, Doug Kamerow, has written a book that I think you will like.
Besides being a mensch and witty as heck, Doug is a family doctor and a preventive medicine specialist. In his new book, Dissecting American Health Care: Commentaries on Health Policy and Politics, these four characteristics constitute the lens through which he comments on scores of events, controversies and changes in public health and health policy that have taken place over the past four years. For example, Doug writes about last year’s debate over the H1N1 vaccine, the papal position on condoms and HIV, how prevention fared in the health care reform act (ACA) and his attempt to Read more »
*This blog post was originally published at Prepared Patient Forum: What It Takes Blog*
October 11th, 2011 by DavedeBronkart in Health Policy, Opinion
No Comments »

Last week the New York Times reported that some health insurers have applied to regulatory agencies to push premiums sharply higher – usually double-digit increases, while citizens are suffering. This falls on top of the 11 year history reported last year by the Kaiser Family Foundation: wages and inflation are up ~40%, while health costs and worker contributions were up 138% and 159%:
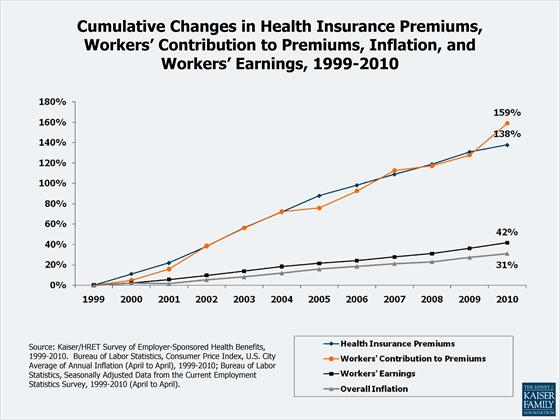
No wonder we feel squeezed. (Last week’s announcement comes on top of this history.)
This has enormous human impact. Read more »
*This blog post was originally published at e-Patients.net*
July 23rd, 2011 by Dr. Val Jones in Health Tips, Opinion
No Comments »
 Alright, I admit that the title of this post is a little dramatic. But it really does seem that most people I know socially have had a bad experience with the healthcare system lately. Take for example my friend whose 3- year-old went to the hospital for a common pediatric procedure – the little girl was overdosed on a medicine, aspirated, got pneumonia, went into respiratory distress (noticed first by her mom) and remained in the pediatric ICU for several days. The hospital staff swept the overdose under the rug, and outright denied it happened when faced with direct questioning. As outrageous as that all is, my friend chose not to pursue action against the hospital and staff for their error and behavior. She just “let it go” because no permanent harm had occurred.
Alright, I admit that the title of this post is a little dramatic. But it really does seem that most people I know socially have had a bad experience with the healthcare system lately. Take for example my friend whose 3- year-old went to the hospital for a common pediatric procedure – the little girl was overdosed on a medicine, aspirated, got pneumonia, went into respiratory distress (noticed first by her mom) and remained in the pediatric ICU for several days. The hospital staff swept the overdose under the rug, and outright denied it happened when faced with direct questioning. As outrageous as that all is, my friend chose not to pursue action against the hospital and staff for their error and behavior. She just “let it go” because no permanent harm had occurred.
Another dear friend was recently misdiagnosed with having a pulmonary condition when he was in heart failure from an arrhythmia… and almost had a stroke during a contraindicated pulmonary stress test. His simple conclusion: “doctors suck.” Was anyone held accountable for this? No. Again because no permanent harm had occurred.
Just the other night I was having dinner with some visitors from out of town. They both told me Read more »
March 20th, 2011 by Jessie Gruman, Ph.D. in Health Tips, True Stories
1 Comment »

 I am a poster child for why everyone who has had cancer needs to work with their doctor(s) to develop and implement a survivorship plan.
I am a poster child for why everyone who has had cancer needs to work with their doctor(s) to develop and implement a survivorship plan.
Two of my four cancer-related diagnoses were found during routine screenings. Two of my cancer-related diagnoses and one serious heart condition were almost certainly due to late effects of cancer treatment when I was young.
Each was a complete surprise to me, and while there is evidence that predicts most of these occurrences, not one of my doctors used this literature to shape a plan for my post-treatment care.
I was on my own. My fear of yet another recurrence led me over time to cobble together a motley collection of oncologists (one for each body part) and other specialists (cardiologist, dermatologist, endocrinologist, and so forth) to watch over me. I thought I was lucky that this has worked so far. Read more »
*This blog post was originally published at CFAH PPF Blog*
January 6th, 2011 by admin in Research, True Stories
No Comments »

This is a guest post from Dr. Jessie Gruman.
**********
More Can Also Be Less: We Need A More Complete Public Discussion About Comparative Effectiveness Research
When the public turns its attention to medical effectiveness research, a discussion often follows about how this research might restrict access to new medical innovations. But this focus obscures the vital role that effectiveness research will play in evaluating current medical and surgical care.
I am now slogging through chemotherapy for stomach cancer, probably the result of high doses of radiation for Hodgkin lymphoma in the early 1970s, which was the standard treatment until long-term side effects (heart problems, additional cancers) emerged in the late 80s. So I am especially attuned to the need for research that tracks the short and long-term effectiveness — and dangers — of treatments.
Choosing a surgeon this September to remove my tumor shone a bright light for me on the need for research that evaluates current practices. Two of the three surgeons I consulted wanted to follow “standard treatment procedures” and leave a six-centimeter, cancer-free margin around my tumor. This would mean taking my whole stomach out, because of its anatomy and arterial supply.
The third surgeon began our consultation by stating that her aim would be to preserve as much of my stomach as possible because of the difference in quality of life between having even part of one’s stomach versus none. If at all possible, she wanted to spare me life without a stomach.
But what about the six-centimeter margin? “There isn’t really much evidence to support that standard,” she said. “This issue came up and was discussed at a national guidelines meeting earlier in the week. No one seemed to know where it came from. We have a gastric cancer registry at this hospital going back to the mid 1990s and we haven’t seen support for it there, either. A smaller margin is not associated with an increased risk of recurrence.” Read more »
 My friend and former Chair of the CFAH Board of Trustees, Doug Kamerow, has written a book that I think you will like.
My friend and former Chair of the CFAH Board of Trustees, Doug Kamerow, has written a book that I think you will like.




 Alright, I admit that the title of this post is a little dramatic. But it really does seem that most people I know socially have had a bad experience with the healthcare system lately. Take for example my friend whose 3- year-old went to the hospital for a common pediatric procedure – the little girl was overdosed on a medicine, aspirated, got pneumonia, went into respiratory distress (noticed first by her mom) and remained in the pediatric ICU for several days. The hospital staff swept the overdose under the rug, and outright denied it happened when faced with direct questioning. As outrageous as that all is, my friend chose not to pursue action against the hospital and staff for their error and behavior. She just “let it go” because no permanent harm had occurred.
Alright, I admit that the title of this post is a little dramatic. But it really does seem that most people I know socially have had a bad experience with the healthcare system lately. Take for example my friend whose 3- year-old went to the hospital for a common pediatric procedure – the little girl was overdosed on a medicine, aspirated, got pneumonia, went into respiratory distress (noticed first by her mom) and remained in the pediatric ICU for several days. The hospital staff swept the overdose under the rug, and outright denied it happened when faced with direct questioning. As outrageous as that all is, my friend chose not to pursue action against the hospital and staff for their error and behavior. She just “let it go” because no permanent harm had occurred. I am a poster child for why everyone who has had cancer needs to work with their doctor(s) to develop and implement a survivorship plan.
I am a poster child for why everyone who has had cancer needs to work with their doctor(s) to develop and implement a survivorship plan.










