December 28th, 2015 by Dr. Val Jones in True Stories
1 Comment »
 Most physicians will be thrust into the role of patient or caregiver at some point during their careers. Unfortunately, it’s not until this occurs that many become fully aware of the finer points of excellent care and communication. Take for example, the simple act of reporting test results to a patient. We do this every day, but may not realize that how we frame the information is as important as the data themselves.
Most physicians will be thrust into the role of patient or caregiver at some point during their careers. Unfortunately, it’s not until this occurs that many become fully aware of the finer points of excellent care and communication. Take for example, the simple act of reporting test results to a patient. We do this every day, but may not realize that how we frame the information is as important as the data themselves.
I came to realize this on a recent hospital visit when I was in the role of healthcare proxy for a loved one with heart disease. Not only did various physicians present information with different degrees of optimism, but individual doctors presented things differently on different days… depending on (I guess) how tired/hurried they were. Consider these different messages with the same ejection fraction (EF – a measure of heart pump strength) and angiogram (heart vessel imaging) test results:
Doctor 1: “I wish I had better news. The EF is lower than we thought. It is low because of your previous massive heart attack.”
Doctor 2: “Although your EF is impaired, there’s a lot that can be done to improve pump function with medications.”
Doctor 1 (different day): “On the other hand, the EF might be temporarily low because of your recent flu infection. It’s possible it will bounce back in a couple of months and you’ll be back to your usual self.”
Doctor 2: “I’m not worried about your chest pain because we know it’s caused by small vessel disease. Your angiogram showed that all your main heart arteries are wide open. The pain is not dangerous, though I’m sure it’s annoying.”
Doctor 1: “Chest pain is always serious. You never know when it could be the big one.”
Doctor 3: “It’s hard to interpret EF because some people live long and productive lives with low EFs, and others are quite impaired with only a small dip in pump function.”
Doctor 2: “Sure there are medications we can try to improve your EF, but I doubt you’ll tolerate them because your blood pressure is kind of low.”
Doctor 3: “Don’t worry about the EF, it will correct on its own once we get your rhythm controlled. This is an electrical problem, not plumbing.”
All of this emotional whiplash caused by the same test results… due to different physicians’ interpretations of prognosis and treatment options. What can be done? First of all, we physicians need to take a deep breath and realize how our words affect our patients. They are scared and vulnerable, and they are looking to us for hope… and when there is real hope, why not emphasize it? There is no need to focus on the worst-case scenarios until we are well and truly in their midst.
I believe that being a good clinician is not just about giving patients factual information, but also about presenting data with kindness. Sometimes, as I’ve discovered with my own loved one, it’s not as important what you say, as how you say it.
May 7th, 2011 by DavedeBronkart in Health Tips, Opinion
No Comments »

A vital aspect of participatory medicine is helping patients learn how to participate. This week I saw a great example of someone who’s doing it right. Here’s the story, including the patient aid for download.
 We hear a lot about “patient-centered”: patient-centered care, patient-centered thinking, everything. Frankly, a lot of it strikes me as patient-centered paternalism: people mean well, but patients sense that the thinking didn’t happen while standing in patients’ shoes, because the advice, policies, and publications just don’t hit home. It’s like somebody guessed what you want, instead of knowing (because they’re like you).
We hear a lot about “patient-centered”: patient-centered care, patient-centered thinking, everything. Frankly, a lot of it strikes me as patient-centered paternalism: people mean well, but patients sense that the thinking didn’t happen while standing in patients’ shoes, because the advice, policies, and publications just don’t hit home. It’s like somebody guessed what you want, instead of knowing (because they’re like you).
A couple of years ago I learned about Planetree, a terrific, small organization in Connecticut that’s been thinking from the patient’s point of view for thirty three years. (Yes, since 1978. Why are they not better known??)
This week I attended a live webcast at a “Planetree designated” hospital, Griffin Hospital, in Derby CT, produced by HealthLeaders Media. When somebody’s truly patient centered, you rarely hear a puzzled “Do people really need that?” or “Isn’t this good enough?”, because they start with what patients want. (See founders’ story at bottom.)
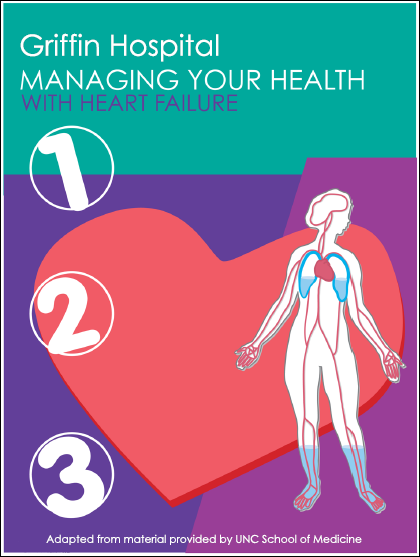
A great example is this booklet about CHF (congestive heart failure), which Griffin Hospital was kind enough to share. (Click the image to download the entire PDF, (1.7MB).) In my day job I did a bit of instructional development, so I can appreciate how well this was done: the “to-do” items are clearly presented, with NO extraneous explanation, and top-class use of icons and images. It’s all essential information, clearly presented, and nothing else. It’s what you need to do to succeed as a patient. Read more »
*This blog post was originally published at e-Patients.net*
April 14th, 2011 by Happy Hospitalist in Health Policy, Humor, True Stories
No Comments »

This was a classic moment of comical clarity that only comes along once a week. As you may or may not know, starting in 2013, The Medicare National Bank has promised to take back 1% of all of a hospital’s total Medicare revenue (to increase in future years) if the hospital has a higher 30 day readmission rate for congestive heart failure, acute myocardial infarction or pneumonia than an as yet undefined acceptable 30 day rate of readmission.
What does this mean? It means if the government decides that 20% is an acceptable rate for congestive heart failure 30 day readmission, and the hospital has a readmission rate of 25%, the hospital will be told to return 1% of all Medicare revenue for the year, not just their heart failure revenue.
Let’s use some hypothetical numbers, shall we? If a hospital generates $250 million dollars in a year on 25,000 Medicare discharge diagnosis related groups (DRGs) but only 100 of those discharge DRGs (or $1,000,000) were heart failure in 2013, what would happen if 21 CHF patients returned for readmission (a 21% thirty day readmission rate) within 30 days for heart failure instead of allowable 20%? The hospital would have to return 2.5 million dollars (1% of their total revenue on all Medicare admissions).
That one patient that took them from 20% to 21% will cost them 2.5 million dollars. The hospital would generate one million dollars in CHF revenue for the year and pay back 2.5 million dollars in penalty. That’s a pretty hefty price to pay considering that hospital profit margins from Medicare have been negative, on average, for most of the last decade. Read more »
*This blog post was originally published at The Happy Hospitalist*
March 28th, 2011 by PJSkerrett in Health Tips, News
No Comments »


The condition that took Elizabeth Taylor’s life affects millions of Americans.
Reports of Elizabeth Taylor’s death focused, as they should, on her life, not on her death from heart failure. But given how common this condition is—the American Heart Association says nearly 6 million Americans are living with heart failure and it kills about 300,000 each year—a little attention to it might be a good idea.
What is heart failure?
The term “heart failure” is a scary one, conjuring up images of a heart that is suddenly unable to work. In truth, it represents a gradual decline in the heart’s ability to pump enough blood to meet the body’s needs. As the heart weakens, all parts of the body suffer the consequences. Read more »
*This blog post was originally published at Harvard Health Blog*
December 2nd, 2010 by John Mandrola, M.D. in Better Health Network, News, Opinion, Research
No Comments »

In treating atrial fibrillation (AF), this year has witnessed some real excitement. And not all the good news has to do with new pills. Recently, there has been a flurry of encouraging and objective news on ablating AF. Here are some comments on three notable studies that address three important questions:
1. What are the “long-term” success rates of AF ablation?
On this important question comes an American Heart Association (AHA) abstract from the highly-regarded lab of Dr. Karl-Heinz Kuck in Hamburg. They report on a relatively young cohort of 161 patients who underwent AF ablation (using standard pulmonary vein isolation techniques) in 2003-2004. At an average of five years of follow up, more than 80 percent were either AF-free or “clinically improved.”
Real-world impression: Although late recurrences of AF years after successful ablation have been reported, my impression (having started with AF ablation in 2004) is that most who are AF-free off drugs after one year have remained AF-free thus far. Read more »
*This blog post was originally published at Dr John M*
 Most physicians will be thrust into the role of patient or caregiver at some point during their careers. Unfortunately, it’s not until this occurs that many become fully aware of the finer points of excellent care and communication. Take for example, the simple act of reporting test results to a patient. We do this every day, but may not realize that how we frame the information is as important as the data themselves.
Most physicians will be thrust into the role of patient or caregiver at some point during their careers. Unfortunately, it’s not until this occurs that many become fully aware of the finer points of excellent care and communication. Take for example, the simple act of reporting test results to a patient. We do this every day, but may not realize that how we frame the information is as important as the data themselves.

















