January 5th, 2015 by Dr. Val Jones in Health Tips, Research
No Comments »
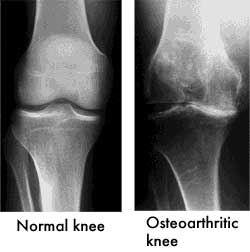 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
#1. Knee injection with gel (Rx hyaluronic acid)
#2. Knee injection with steroid (Rx corticosteroid)
#3. Diclofenac (Voltaren – Rx oral NSAID)
#4. Ibuprofen (Motrin – OTC oral NSAID)
#5. Naproxen (Alleve – OTC oral NSAID)
#6. Celecoxib (Celebrex – Rx NSAID)
#7. Knee injection with saline solution (placebo injection)
#8. Acetaminophen (Tylenol – OTC Synthetic nonopiate derivative of p-aminophenol)
#9. Oral placebo (Sugar Pill)
I found this rank order list interesting for a few reasons. First of all, acetaminophen and celecoxib appear to be less effective than I had believed. Second, placebos may be demonstrably more effective the more invasive they are (injecting saline into the knee works better than acetaminophen, and significantly better than sugar pills). Third, injection of a cushion gel fluid is surprisingly effective, especially since its mechanism of action has little to do with direct reduction of inflammation (the cornerstone of most arthritis therapies). Perhaps mechanical treatments for pain have been underutilized? And finally, first line therapy with acetaminophen is not clinically superior to placebo.
There are several caveats to this information, of course. First of all, arthritis pain treatments must be customized to the individual and their unique tolerances and risk profiles. Mild pain need not be treated with medicines that carry higher risks (such as joint infection or gastrointestinal bleeding), and advanced arthritis sufferers may benefit from “jumping the line” and starting with stronger medicines. The study is limited in that treatments were only compared over a 3 month trial period, and we cannot be certain that the patient populations were substantially similar as the comparative effectiveness was calculated.
That being said, this study will influence my practice. I will likely lean towards recommending more effective therapies with my future patients, including careful consideration of injections and diclofenac for moderate to severe OA, and ibuprofen/naproxen for mild to moderate OA, while shying away from celecoxib and acetaminophen altogether. And as we already know, glucosamine and chondroitin have been convincingly shown to be no better than placebo, so save your money on those pills. The racket is expected to blossom into a $20 billion dollar industry by 2020 if we don’t curb our appetite for expensive placebos.
In conclusion, the elephant in the room is that weight loss and exercise are still the very best treatments for knee osteoarthritis. Check out the American Academy of Orthopedic Surgery’s recent list of evidence-based recommendations for the treatment of knee arthritis for more information about the full spectrum of treatment options.
March 21st, 2011 by Michael Kirsch, M.D. in News, Opinion
No Comments »

 Recently, every newspaper in the country reported on a landmark development in breast cancer treatment. It is now clear that certain breast cancer women do not need to undergo removal of lymph nodes from the armpit as part of their treatment. This would spare them from the risk and discomfort of an unnecessary procedure. It is welcome news, particularly for those of us who argue that in medicine, less is more. This is an example of the benefit of comparative effectiveness research, a tool that can separate what patients truly need from what the medical profession believes they must have.
Recently, every newspaper in the country reported on a landmark development in breast cancer treatment. It is now clear that certain breast cancer women do not need to undergo removal of lymph nodes from the armpit as part of their treatment. This would spare them from the risk and discomfort of an unnecessary procedure. It is welcome news, particularly for those of us who argue that in medicine, less is more. This is an example of the benefit of comparative effectiveness research, a tool that can separate what patients truly need from what the medical profession believes they must have.
Let’s hope that breast cancer breakthrough metastasizes across the medical profession. Here’s what it accomplished.
- It spares women from unnecessary surgery.
- It saves money.
- It demonstrates that physicians and medical professionals can serve the public interest.
- It gives hope that all medical specialties will critically evaluate and justify the tests and treatments that we recommend to our patients.
Ironically, when the U.S Preventive Services Task Force (USPSTF) published their mammography guidelines last year, also arguing that less is more, they were assailed as medical traitors against women.
When it comes to breasts
There’s a tug of war
Some want less
And some want more.
Every practicing physician, medical educator and researcher should examine their own practices and medical advice. On what basis do we recommend our treatments? Do we do so because we were taught these practices in our training years ago? Is it from habit or adhering to the community standard? Is it because patients have such a high expectation of a medical intervention that we feel obligated to act?
Can anyone argue that patients are subjected to too much/many
- Chemotherapy
- Antibiotics
- Colonoscopies
- Cardiac stents
- CAT scans and their imaging cousins Read more »
*This blog post was originally published at MD Whistleblower*
March 12th, 2010 by StaceyButterfield in Better Health Network, News
No Comments »

As one would expect from such a diverse group, comparisons were a common topic at the co-located National Medical Home Summit, National Retail Clinic Summit, and Population Health and Disease Management Colloquium this week.
During an opening session, Carolyn Clancy, head of the AHRQ, updated us on some of the comparison work her agency has been doing. Last year’s stimulus bill dedicated a lot of funds ($300 mill directly, more through the Secretary of HHS) to the agency’s work on comparative effectiveness. Read more »
*This blog post was originally published at ACP Internist*
January 11th, 2010 by DrRich in Better Health Network, Health Policy, Opinion
No Comments »

As has been pointed out (pointedly) to DrRich, we do not have death panels in the United States. And indeed, considering that we’re not conducting military tribunals for Islamist terrorists who have tried (or succeeded in) killing and maiming as many of us as possible, it seems relatively unlikely that we’d assemble death panels (which sound even less due-process-friendly than military tribunals) for American patients.
What we will have, however, is a federally-mandated assembly, body, committee, commission, board, diet, parliament, or posse (but not a panel) of experts which will carefully evaluate all the objective clinical evidence regarding a particular medical treatment, and make “recommendations” to doctors about whether or when to use that treatment. The model which frequently has been offered up for our consideration, as we contemplate the workings of such a non-death-panel, is the British National Institute for Clinical Excellence, or NICE. Read more »
*This blog post was originally published at The Covert Rationing Blog*
October 6th, 2009 by DrWes in Better Health Network, Health Policy, News
No Comments »

I just finished our first day at the Principle Investigator Meeting for the launch of the Catheter Ablation Versus Anti-arrhythmic Drug Therapy for Atrial Fibrillation (CABANA) trial in Philadelphia today. The trial is a 3000-patient patient trial performed at 140 centers around the world and jointly sponsored by the National Heart, Lung, and Blood Institute (NHLBI), a component of the National Institutes of Health (NIH), and industry (St. Jude Medical and Biosense Webster).
The trial will randomize 3000 previously untreated or incompletely treated patients at high risk of cardiovascular complications in the trial to two arms: 1500 patients to catheter ablation as primary therapy of atrial fibrillation and the other 1500 patients to conventional medical therapy with rate control or rhythm control strategies to determine if catheter ablation is superior to medical therapy at reducing total mortality (the primary endpoint). Secondary endpoints of a composite endpoint of mortality, disabling stroke, serious bleeding, or cardiac arrest will also be studied.
If done properly, this study stands to be a landmark trial for the field of cardiac electrophysiology and has huge ramifications for the treatment of patients with atrial fibrillation. Also, it doesn’t take a lot of rocket science to know that the government will be looking closely at the results of this trial to determine which treatment strategy will receive government funding. Read more »
*This blog post was originally published at Dr. Wes*
 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
















