June 23rd, 2011 by BarbaraFicarraRN in Health Tips, Opinion
No Comments »

[image: iStockphoto]

Ladies imagine planning your daily events based around the timing of you menstrual cycle.
Some women suffering from uterine fibroids have a menstrual flow so heavy that it can impede their life.
“Everything must be planned around their menstrual, and it can be very draining physically (from the anemia of blood loss), as well as, mentally from the resulting stress this creates,” says Dr. John Lipman, Director of Interventional Radiology & Center For Image-Guided Medicine, Emory-Adventist Hospital, Atlanta, Georgia. “This can imprison women such that their entire life is tied to the menstrual cycle. They may not work or even be able to leave the house for several days each month. Even if they can work, the frequent interruptions throughout the day often makes this time very unproductive,” he adds.
“Uterine fibroids are the most common non-cancerous tumors in women of childbearing age. Fibroids are made of muscle cells and other tissues that grow in and around the wall of the uterus, or womb. The cause of fibroids is unknown. Risk factors include being African-American or being overweight.”
According to The National Women’s Health Information Center – U.S. Department of Health and Human Services Office on Women’s Health, about 20 percent to 80 percent of women develop fibroids by the time they reach age 50.
Dr. Lipman writes: Read more »
*This blog post was originally published at Health in 30*
May 22nd, 2010 by Toni Brayer, M.D. in Better Health Network, Health Tips
1 Comment »

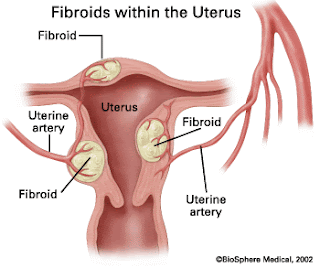 Uterine fibroids are benign growths on the muscular wall of the uterus. They can be tiny in size (like a marble) or grow huge and fill up the entire uterine cavity. Some fibroids are as large as a five-month pregnancy. There are certain facts that women should know about uterine fibroids. Read more »
Uterine fibroids are benign growths on the muscular wall of the uterus. They can be tiny in size (like a marble) or grow huge and fill up the entire uterine cavity. Some fibroids are as large as a five-month pregnancy. There are certain facts that women should know about uterine fibroids. Read more »
*This blog post was originally published at EverythingHealth*
April 25th, 2009 by eDocAmerica in Better Health Network
No Comments »
This article was co-authored by Elyse Chapman, who became an e-patient through the following process:
I recently became acquainted with a woman in Iowa, Elyse Chapman, who was concerned about her “fibroids”. I heard about her from a colleague whose online moniker is “e-Patient Dave”. Dave deBronkart used information from the internet to successfully steer the course of his own therapy for kidney cancer . Elyse is a friend of Dave’s who was scheduled for a hysterectomy because of a very large, mass, probably a uterine fibroid, a benign but often problematic tumor of the smooth muscle fibers of the uterus. She had problems with excessive painful cramping, bladder pressure and a sensation of swelling and bloating in her abdomen. A CT scan was ordered and showed a mass either on the ovary or uterus. The mass was so large that her doctors wanted to make sure that this was not a malignant tumor of the uterus or ovary. They had scheduled a total hysterectomy via exploratory laparotomy in 3 weeks and Dave was “consulting” with his online friends to see if anyone knew of a patient group with whom she could collaborate to see if there was an alternative to major surgery.
I volunteered to help. Shortly thereafter, I received an e-mail from Elyse and then gave her a call. I heard more details about her history, learned that she had lost her husband recently, and as a single parent, felt very shaky about the prospects of recovering from major surgery without help at home. She wondered why her doctors were so focused on performing a total hysterectomy and why she wouldn’t be a candidate for a laparoscopic approach. She also wondered if she really even needed to undergo surgery now, or could she safely wait and watch for a time.
Unable to determine for certain that an alternative approach was feasible in her case, I encouraged her, at the very least, to become more assertive about getting answers to her questions: If she wasn’t a candidate for laparoscopy, why not? I told her I’d do some further research about this and get back in touch with her. I looked this up on the internet and then sent her this e-mail:
I looked at some sites on laparoscopic hysterectomy. Here is one I thought was good:http://www.ohanlan.com/laparoscop.htmFrom what I can tell, it should be possible to remove even a large uterine mass via laparoscopy.Good luck getting an answer on this that makes sense to you. Let me know if I can help any further.
Elyse actually communicated directly with a nurse at the above site and it bolstered her belief that it may not be necessary to undergo a total abdominal hysterectomy. She communicated this to her doctors in Iowa who were still uncomfortable exploring alternative options. So, she sent me the following e-mail:
http://www.google.com/search?hl=en&q=fibroids+ultrasound&btnG=Google+Search&aq=0&oq=fibroids+ul
Charlie, have you heard of this — nuking the fibroid with ultrasound while using MRI to view and target the waves? Just learned of it today.Seems to me that U of I is wanting to just yank everything out even though there’s no proof that this growth is malignant. Sounds to my laywoman’s brain like at very worst there’s a 50-50 chance of malignancy, yet they do not want to do a biopsy for fear of rupturing something that might be ovarian and malignant, causing easy spread of malignant cells. What I don’t understand is how anyone can determine if its malignant without a biopsy, but obviously someone knows how to do that, because links in the above results say the ultrasound procedure works well for non malignant fibroids, which means that somehow there’s a way to determine malignancy or no without too much fuss.U of I insists that there is no better imaging method than the CT scan I had, but at least some of the above links state that MRI is better. Huh?? Who is right? Is this a case of “we only know how to use a hammer, so everything we see must be a nail” or maybe “we’re financially invested in [name your imaging method of choice], so we’re going to use and promote that”?Thoughts, please?
Elyse
Well, truthfully, I had not heard of this technique, so I did some additional research and found that the number of sites offering the procedure were limited, but sent these to her, with some additional links from the internet. In addition, this e-mail string reminded me that an increasing number of doctors and patients are opting for uterine artery embolization. I mentioned this, and she e-mailed me back that she was unable to find links for this procedure that I mentioned.
Here is my reply to her:
Elyse,
I should have used the “correct” term: uterine artery embolization.
Here: http://www.fibroidworld.com/UAE.htm
This is another very reasonable alternative for you to consider, maybe even more realistic than the ultrasound approach.
Charlie
After several more fax and phone exchanges between Elyse and the physician in California who published the web site noted above, and after phone exchanges with the physicians in Iowa, Elyse underwent an ultrasound examination that confirmed a large, single uterine fibroid about 6 or 7 cm in diameter. The Gynecologist/Oncologist in California felt that surgery was entirely optional at this point, noting that Elyse would likely experience shrinkage of the mass following menopause within a few years.
She is still in the process of finalizing her decision whether to proceed with a laparoscopic hysterectomy or take the “watch and wait” approach but is certain of one thing: she is NOT going to proceed with the scheduled total abdominal hysterectomy.
So, that is where we stand. But, what is the point? Well, the HUGE point is, Elyse is no longer content to blindly follow her doctor’s suggestions. Whereas they suggested she undergo a major surgical procedure, they didn’t even mention two significant new, less invasive procedures that might well be appropriate for her to consider, and did not give her clear information to consider the option of just watching and waiting.
The other point of the story is that a wealth of information is available on the web, but patients often need encouragement to seek it, and help interpreting it and applying it to their own situations. Peer support groups on line are one way to accomplish this and finding an interested, available physician to serve as an “e-patient advisor” is another way.
Either way, it is a good example of how patients are moving into the e-patient revolution and, through this process, the health care system is changing. In the meantime, join me in hoping Elyse soon finds the perfect solution for herself and has a great outcome.
*This blog post was written by Dr. Charlie Smith and originally published at the eDocAmerica blog.*





 Uterine fibroids are benign growths on the muscular wall of the uterus. They can be tiny in size (like a marble) or grow huge and fill up the entire uterine cavity. Some fibroids are as large as a five-month pregnancy. There are certain facts that women should know about uterine fibroids.
Uterine fibroids are benign growths on the muscular wall of the uterus. They can be tiny in size (like a marble) or grow huge and fill up the entire uterine cavity. Some fibroids are as large as a five-month pregnancy. There are certain facts that women should know about uterine fibroids. 









