October 20th, 2015 by Dr. Val Jones in Health Tips, Opinion
1 Comment »
 Most of my patients think about pain medicines in terms of the symptoms they treat. “This is my headache medicine, and this is my arthritis medicine,” they often say. Healthcare providers are more likely to categorize pain medicines by the way they work: some are anti-inflammatory, some affect nerve endings, and others influence how the brain perceives pain. But the truth is that no matter how you classify pain medicines, there is no way to know if they’ll help until you try them for yourself.
Most of my patients think about pain medicines in terms of the symptoms they treat. “This is my headache medicine, and this is my arthritis medicine,” they often say. Healthcare providers are more likely to categorize pain medicines by the way they work: some are anti-inflammatory, some affect nerve endings, and others influence how the brain perceives pain. But the truth is that no matter how you classify pain medicines, there is no way to know if they’ll help until you try them for yourself.
Most people don’t realize that pain management is personal. Research is beginning to help us understand why people respond to medicines so differently, and one day we will probably be able to personalize treatment plans more successfully. For now, there are several known genetic reasons why pain medicines are more or less effective for one individual over another. Genes affect:
-
The number of enzymes that break down medicines and remove them from the body. Some people have larger numbers of these enzymes and therefore require more drug to feel its pain-relieving effects. Others may be strongly affected by even small doses of drug.
-
Pain medicine receptor variations can make one medicine effective and another (nearly identical medicine) ineffective in relieving pain.
-
Differences in carrier molecules that transport pain medicine across the blood stream and into the cells that are triggering pain sensations. Some people have fewer carrier molecules to bring the medicine to the site of pain.
-
The number of “middle man” neurotransmitter molecules that pass along the pain response. Too many of these molecules can reduce drug binding and mute the pain relief effects of some drugs.
When pain is severe, prescription medications may be necessary. However, mild to moderate pain may be effectively managed with over-the-counter (OTC) medicines. I believe in the start low, go slow approach to finding the smallest effective dose of pain medicines. I always recommend that my patients read and follow all the instructions on the Drug Facts labels to make sure that they don’t accidentally overdose on active ingredients.
When I choose a pain reliever with my patients, the first thing I think about is potential side effects. Some medicines (such as non-steroidal anti-inflammatory drugs like ibuprofen and naproxen sodium) can be hard on the stomach lining, or cause bleeding in people who are at risk for it. Other medicines (such as acetaminophen) can harm the liver if used in excess, while prescription pain medicines can cause constipation and drowsiness. The best pain medicine to start with is one that is least likely to cause harm to the specific person.
The next thing I ask is whether or not the medicine has worked for the patient in the past. Previous experience is one of the best indicators of future success. Since I know that my patient has a unique, genetically determined number of enzymes, transporters, and receptors, previous experience with pain medicines will give me a good idea of how well they will tolerate it again, and if it will be effective.
Finally, I consider the type of pain that they are experiencing. If the pain is caused by inflammation (from an injury, surgery, or arthritis) I’ll consider a medicine with primarily anti-inflammatory properties. If the pain is caused by tension (such has headache) or complicated by fever, I may consider acetaminophen first. If the pain is coming from a nerve (such as sciatica or neuropathy) then I’ll use pain medicines that work for nerve pain specifically. If the pain is complicated by depression, I may discuss additional medicines and approaches.
Sometimes, combinations of medicines are significantly more effective than one medicine alone at treating pain (this is why some prescription pain relievers are combinations of an opioid and acetaminophen). When using more than one pain relief medicine, it is important to compare active ingredients in both prescription medications and OTC products to make sure that accidental overdoses do not occur. I also recommend consulting with a healthcare professional if there are concerns about drug interactions or if the patient is already on a significant number of prescription medications that could interact with his or her OTC pain medicine choices.
The bottom line is that science is still catching up to pain management. Perhaps one day a simple blood test will help us to determine the very best pain medicine regimen for a specific patient at a given time. But until then, adopting a strategy of careful trial and error (avoiding unwanted side effects, using the lowest effective doses, and consulting a physician when pain is severe) is the only option. Don’t worry too much about whether a specific medicine is “best” for your pain. Pain management is very personal, so you will need to discover your own best solution.
***
Disclosure: Dr. Val Jones is a paid consultant for McNeil Consumer Healthcare Division.
January 5th, 2015 by Dr. Val Jones in Health Tips, Research
No Comments »
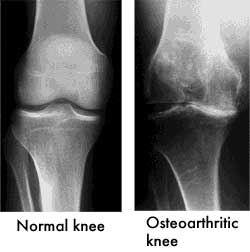 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
#1. Knee injection with gel (Rx hyaluronic acid)
#2. Knee injection with steroid (Rx corticosteroid)
#3. Diclofenac (Voltaren – Rx oral NSAID)
#4. Ibuprofen (Motrin – OTC oral NSAID)
#5. Naproxen (Alleve – OTC oral NSAID)
#6. Celecoxib (Celebrex – Rx NSAID)
#7. Knee injection with saline solution (placebo injection)
#8. Acetaminophen (Tylenol – OTC Synthetic nonopiate derivative of p-aminophenol)
#9. Oral placebo (Sugar Pill)
I found this rank order list interesting for a few reasons. First of all, acetaminophen and celecoxib appear to be less effective than I had believed. Second, placebos may be demonstrably more effective the more invasive they are (injecting saline into the knee works better than acetaminophen, and significantly better than sugar pills). Third, injection of a cushion gel fluid is surprisingly effective, especially since its mechanism of action has little to do with direct reduction of inflammation (the cornerstone of most arthritis therapies). Perhaps mechanical treatments for pain have been underutilized? And finally, first line therapy with acetaminophen is not clinically superior to placebo.
There are several caveats to this information, of course. First of all, arthritis pain treatments must be customized to the individual and their unique tolerances and risk profiles. Mild pain need not be treated with medicines that carry higher risks (such as joint infection or gastrointestinal bleeding), and advanced arthritis sufferers may benefit from “jumping the line” and starting with stronger medicines. The study is limited in that treatments were only compared over a 3 month trial period, and we cannot be certain that the patient populations were substantially similar as the comparative effectiveness was calculated.
That being said, this study will influence my practice. I will likely lean towards recommending more effective therapies with my future patients, including careful consideration of injections and diclofenac for moderate to severe OA, and ibuprofen/naproxen for mild to moderate OA, while shying away from celecoxib and acetaminophen altogether. And as we already know, glucosamine and chondroitin have been convincingly shown to be no better than placebo, so save your money on those pills. The racket is expected to blossom into a $20 billion dollar industry by 2020 if we don’t curb our appetite for expensive placebos.
In conclusion, the elephant in the room is that weight loss and exercise are still the very best treatments for knee osteoarthritis. Check out the American Academy of Orthopedic Surgery’s recent list of evidence-based recommendations for the treatment of knee arthritis for more information about the full spectrum of treatment options.
November 7th, 2011 by Mary Lynn McPherson, Pharm.D. in Opinion, Research
1 Comment »
The overdose death rate from prescription opioids, referred to as “narcotics”, has reached “epidemic levels” in the US according to a report just released by the Centers for Disease Control and Prevention (CDC). The report further states that the intentional misuse and abuse of popular opioids such as OxyContin, Vicodin, methadone and others now cause more deaths than those caused by heroin and cocaine combined.
Dr. Thomas Frieden, CDC Director told reporters that “Narcotics prescribed by physicians kill 40 people a day.” He continued by stating “Prescription painkillers are meant to help people who have severe pain. They are, however, highly addictive.”
The report states that increased prescribing of pain medications by doctors is a significant cause of this growing number of deaths. However, the situation is far more complicated than this report presents. Poor pain management and prescription drug abuse has become Read more »
September 29th, 2011 by PreparedPatient in Health Tips, True Stories
No Comments »

Whether caused by injury, surgery or a toothache so bad it slams you awake in the middle of the night, acute pain is difficult. Receiving prompt and helpful treatment can make all the difference in the world. But lack of care or inadequate care means that the acute pain may develop into chronic agony.
Fortunately, acute pain is not always long lasting or overwhelming, such as when you have a short severe cramp or multiple bee stings that can be handled with time, over-the-counter medication and other home remedies [See: Pain Treatment Options].
Since individuals’ tolerance for pain varies widely, the question of when pain itself requires urgent medical attention is difficult to answer. Chest pain should prompt a visit to the emergency room, of course—but other types of pain are trickier to call. Read more »
*This blog post was originally published at Prepared Patient Forum: What It Takes Blog*
September 13th, 2011 by Toni Brayer, M.D. in Research
No Comments »

 A new study of more than 52,000 pregnant women in Canada shows that miscarriage rates were more than twice as high for women who took a nonsteroidal anti-inflammatory drug (NSAID) compared to women who did not. The study, published in the Canadian Medical Association Journal reported that women who used prescription NSAIDS for just 4 days during early pregnancy had an increased risk for miscarriage.
A new study of more than 52,000 pregnant women in Canada shows that miscarriage rates were more than twice as high for women who took a nonsteroidal anti-inflammatory drug (NSAID) compared to women who did not. The study, published in the Canadian Medical Association Journal reported that women who used prescription NSAIDS for just 4 days during early pregnancy had an increased risk for miscarriage.
These medications are commonly prescribed for pain, cramps, headaches and fever and can be bought over the counter as Advil, Aleeve or Ibuprofen. We have thought they were safe in early pregnancy but this study shows that may not be the case. Read more »
*This blog post was originally published at EverythingHealth*
 Most of my patients think about pain medicines in terms of the symptoms they treat. “This is my headache medicine, and this is my arthritis medicine,” they often say. Healthcare providers are more likely to categorize pain medicines by the way they work: some are anti-inflammatory, some affect nerve endings, and others influence how the brain perceives pain. But the truth is that no matter how you classify pain medicines, there is no way to know if they’ll help until you try them for yourself.
Most of my patients think about pain medicines in terms of the symptoms they treat. “This is my headache medicine, and this is my arthritis medicine,” they often say. Healthcare providers are more likely to categorize pain medicines by the way they work: some are anti-inflammatory, some affect nerve endings, and others influence how the brain perceives pain. But the truth is that no matter how you classify pain medicines, there is no way to know if they’ll help until you try them for yourself.

 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A 












