January 19th, 2011 by BobDoherty in Better Health Network, Health Policy
1 Comment »

Federal law generally prohibits physicians from referring their own patients to a diagnostic facility in which they have an ownership issue — a practice called “self-referral” — unless the facility is located in their own practice. This exemption exists to allow patients with access to a laboratory test, X-ray, or other imaging test at the same time and place as when patients are seeing their physician for an office visit. Less inconvenience and speeder diagnosis and treatment — what could be wrong with that?
Much, say the critics, if it leads to overutilization and higher costs and doesn’t really represent a convenience to patients. This is the gist of two studies by staff employed by the American College of Radiology, published in the December issue of Health Affairs.
One study analyzes Medicare claims data and concludes that patients aren’t really getting “one-stop-shopping” convenience when their physician refers them to an imaging facility that qualifies for the “in-office” exemption.
“Specifically, same-day imaging was the exception, other than for the most straightforward types of X-rays. Overall, less than one-fourth of imaging other than these types of X-rays was accompanied by a same-day office visit. The fraction for high-tech imaging was even lower — approximately 15 percent.” Read more »
*This blog post was originally published at The ACP Advocate Blog by Bob Doherty*
July 27th, 2010 by GarySchwitzer in Better Health Network, Health Policy, News, Opinion, Quackery Exposed, Research
No Comments »

Kudos to Christopher Snowbeck and the St. Paul Pioneer Press for digging into new Medicare data to report that the state the newspaper serves is out of whack with the rest of the country in how many expensive MRI scans are done on Minnesotans’ bad backs.
Snowbeck artfully captures the predictable rationalization and defensive responses coming from locals who don’t like what the data suggest. Because what they suggest is overuse leading to overtreatment. So here’s one attempt a provider makes to deflect the data:
“The Medicare billing/claims data, which this report is generated from, would not capture conversations between a patient and provider that may have addressed alternative therapies for lower back pain,” said Robert Prevost, a spokesman for North Memorial Health Care. “It’s important to recognize the limitations of this data.”
No, data don’t capture conversations. But wouldn’t it be fascinating to be a fly on the wall during those many patient-physician encounters that led to an MRI to see what level of truly informed shared decision-making (if any) took place? Read more »
*This blog post was originally published at Gary Schwitzer's HealthNewsReview Blog*
June 22nd, 2010 by Davis Liu, M.D. in Better Health Network, Health Policy, News, Opinion
1 Comment »

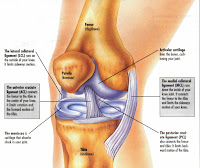 Boston Celtics basketball player Kendrick Perkins injured his knee during the NBA Finals against the Lakers when he landed awkwardly. Unable to weightbear, he left Game 6 not to return for the following pivotal Game 7.
Boston Celtics basketball player Kendrick Perkins injured his knee during the NBA Finals against the Lakers when he landed awkwardly. Unable to weightbear, he left Game 6 not to return for the following pivotal Game 7.
Based on his mechanism of injury and his physical examination, his trainer reported that he tore his medial collateral ligament (MCL) as well as the posterior cruciate ligament (PCL). More amazingly, this was done without the help of a MRI. Since Perkins was unable to play the final game, there was no urgent medical need to expedite the test, as regardless of the result his season was already done.
How do doctors know what’s wrong without X-ray vision or an imaging test? (Note that Perkins did get a X-ray, but X-rays generally don’t show ligament injuries.) Is it guessing? Read more »
*This blog post was originally published at Saving Money and Surviving the Healthcare Crisis*
March 25th, 2010 by KevinMD in Better Health Network, News, Opinion
No Comments »

It’s well known that the use of imaging scans, like CTs, MRIs and PET scans, have been growing at an alarming rate. But a recent study provides some stark numbers. According to a recent CDC report, “MRI, CT or PET scans were done or ordered in 14 percent of ER visits in 2007.” That’s four times as often as in 1996. Although a physician called that growth “astounding,” it’s really no surprise.
Emergency departments are becoming more crowded, and with patient satisfaction scores becoming more influential in financial incentives for physicians, sometimes just ordering a test is the path of least resistance. Factor in the spector of defensive medicine which, according to a survey from the Massachusetts Medical Society, accounts for up to 28 percent of tests ordered, it’s a wonder that more scans weren’t ordered.
Imaging scans are a clear cost driver in healthcare, contributing $12 billion to Medicare’s bill. But costs won’t resonate with patients requesting the tests or the doctors ordering them. One encouraging sign is the recent trend of publicizing the harms of scans, like radiation from CTs. I’m finding that patients are becoming increasingly aware of the risk, and making a more informed decision after I explain it to them. It’s a small step forward.
*This blog post was originally published at KevinMD.com*

















