December 3rd, 2010 by Bryan Vartabedian, M.D. in Better Health Network, Opinion, True Stories
No Comments »

I just can’t imagine life today as a medical student. Every medical publication in the palm of your hand. The capacity to create an audience and publish at your own will. Real-time dialog between students, faculty, anyone. Global reach from your phone. It’s mind-boggling really.
This is in stark contrast to my experience. My world was centered on index cards, textbooks and pens with different colors. We communicated via Post-it notes on the door of the student lounge. There were no apps and our only game was foozball. As a first year I scheduled time to compose H&Ps on the library’s only Macintosh II computer. This was plugged into the new Apple LaserWriter with WYSIWYG. Hi tech we were. We thought.
Being distractible and restless, I’m going to guess that if I had access to the communication platforms and tools available to today’s students, I might not have made it through. The inputs must be staggering and I imagine that discipline with personal bandwidth has become a critical key to survival. Read more »
*This blog post was originally published at 33 Charts*
December 2nd, 2010 by KevinMD in Better Health Network, News, Opinion
No Comments »

Medical students today consider lifestyle an essential criteria when choosing a specialty. It’s become a cliche that most are looking towards the ROAD (radiology, ophthalmology, anesthesiology and dermatology) to happiness.
There’s been some recent media attention at how women are lured to specialties that offer a greater balance between their family lifestyle and professional demands. Claudia Golden, a Harvard economics professor, recently noted that,
high-paying careers that offer more help in balancing work and family are the ones that end up luring the largest numbers of women. Surprisingly, colon and rectal surgery is one of these, because of rapid growth in routine colonoscopies that can be scheduled in advance, giving doctors control over their time. Goldin says 31% of colon and rectal surgeons under 35 years of age were female in 2007, compared with only 3% of those ages 55 to 64, and 12% of those ages 45 to 54, reflecting the fact that younger women are flocking to the field.
Of course, what’s not said is the grueling training that it takes to become a colorectal surgeon — but the numbers cited above do not lie. The new generation of doctors — both men and women — want greater control of their time. That means more shift-work and a predictable call schedule. Read more »
*This blog post was originally published at KevinMD.com*
August 16th, 2010 by BobDoherty in Better Health Network, Health Policy, News, Research
1 Comment »

Yes, according to a study in today’s Health Affairs. (The full text of the study is available only to subscribers, but Kaiser Health News Daily has a good summary of its findings and links to other news reports.)
The study compares inpatient death rates and lengths of stay for patients with congestive heart failure or acute myocardial infarction when provided by U.S. citizens trained abroad, citizens trained in the United States, and non-citizens trained abroad. Treatment was provided by internists, family physicians, or cardiologists. The differences were striking, according to the authors:
“Our analysis of 244,153 hospitalizations in Pennsylvania found that patients of doctors who graduated from international medical schools and were not U.S. citizens at the time they entered medical school had significantly lower mortality rates than patients cared for by doctors who graduated from U.S. medical schools or who were U.S. citizens and received their degrees abroad.”
Read more »
*This blog post was originally published at The ACP Advocate Blog by Bob Doherty*
August 15th, 2010 by GruntDoc in Better Health Network, Humor, Opinion, True Stories
No Comments »

 I’ve internalized all the dogma of medicine, for good and bad.
I’ve internalized all the dogma of medicine, for good and bad.
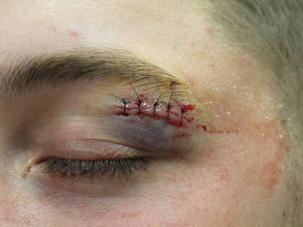
When I was an EMT, green as a twig in an ER, I learned the basics: For any wound with hair employ the razor, and get the hair away from the laceration so the doc could do a good closure.
So, employment week #3: Eyebrow laceration? Shaved that sucker clean off. ER doc freaked out, and I learned some medical dogma: Don’t shave eyebrows, they don’t grow back. Heard it later, too — all the way through training, in fact. Read more »
*This blog post was originally published at GruntDoc*
August 11th, 2010 by Lucy Hornstein, M.D. in Better Health Network, Health Policy, Health Tips, Opinion
No Comments »

 I like Dr. Rob, the one with the “distractible mind.” And although I thoroughly agree with the stance he takes in his recent post against cholesterol screening in kids, I must take issue with his opening statement:
I like Dr. Rob, the one with the “distractible mind.” And although I thoroughly agree with the stance he takes in his recent post against cholesterol screening in kids, I must take issue with his opening statement:
I have a unique vantage point when it comes to the issue universal cholesterol screening in children, when compared to most pediatricians. My unique view stems from the fact that I am also an internist who deals with those children after they grow up on KFC Double Downs.
From Dictionary.com:
“Unique: existing as the only one or as the sole example; single; solitary in type or characteristics.”
Your med-peds training allows you to follow patients from birth to death (but no obstetrics or gynecology). You can care for all organ systems and all stages of disease (but without as much training in psychiatry). Congratulations! You’ve just (re)invented family practice (except for the above shortcomings). Oh, wait — that’s already a recognized specialty with its own residency programs, boards and everything like that, forty years now.
This misuse of the word “unique” is one of my pet peeves. “Unique?” I don’t think that word means what you think it means. After twenty years in practice, I agree that there probably isn’t much difference between what Dr. Rob does and what I do. After twenty years, I’m not even sure how much relevance remains from our “training.” Still, there remains a great deal of confusion about the very real differences between family practice and med-peds residencies. Read more »
*This blog post was originally published at Musings of a Dinosaur*






 I’ve internalized all the dogma of medicine, for good and bad.
I’ve internalized all the dogma of medicine, for good and bad.
 I like Dr. Rob, the one with the “distractible mind.” And although I thoroughly agree with the stance he takes in his
I like Dr. Rob, the one with the “distractible mind.” And although I thoroughly agree with the stance he takes in his 









