June 7th, 2010 by GarySchwitzer in Better Health Network, Health Policy, News, Opinion, Research
No Comments »

The worst-kept secret in journalism circles recently was that the New York Times was planning an article critical of the Dartmouth Atlas. Among the main points in the article:
• “The mistaken belief that the Dartmouth research proves that cheaper care is better care is widespread.”
• “The atlas’s hospital rankings do not take into account care that prolongs or improves lives.”
• “Even Dartmouth’s claims about which hospitals and regions are cheapest may be suspect.”
• “Failing to make basic data adjustments undermines the geographic variations the atlas purports to show.”
The Times has also published the correspondence it had with the Dartmouth team about methodology questions.
The Dartmouth team challenges each of these criticisms. The team says the Times made at least five factual errors and several misrepresentations. They write:
“What is truly unfortunate is that the Times missed an opportunity to help educate the American public about what our research actually shows — or about the breadth of agreement about what our findings mean for health care reform.” Read more »
*This blog post was originally published at Gary Schwitzer's HealthNewsReview Blog*
January 4th, 2010 by Toni Brayer, M.D. in Better Health Network, Health Policy, True Stories
1 Comment »

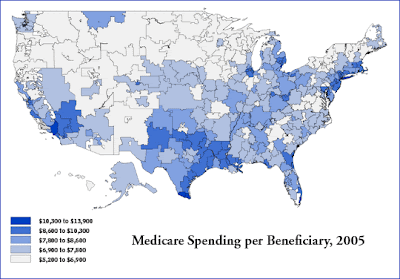 It has been proven than there is tremendous variation in the practice of medicine across the United States. The Dartmouth data (Wennberg et al) has documented the differences in how medical resources are used and how different physicians practice medicine, depending upon where they live. The Dartmouth studies are mainly focused on cost and outcomes and make the case that improved quality is often inversely related to the cost of care. More (expensive) care is not necessarily better care.
It has been proven than there is tremendous variation in the practice of medicine across the United States. The Dartmouth data (Wennberg et al) has documented the differences in how medical resources are used and how different physicians practice medicine, depending upon where they live. The Dartmouth studies are mainly focused on cost and outcomes and make the case that improved quality is often inversely related to the cost of care. More (expensive) care is not necessarily better care.
Now that I am recovering from a total joint replacement, I am amazed to see the differences in how physicians, doing the same surgery, treat the patient. Total knee replacement (TKA) is one of the most common orthopedic procedures done today. Despite this, the patient cannot expect the same post op care. Read more »
*This blog post was originally published at EverythingHealth*
November 8th, 2009 by Richard Cooper, M.D. in Better Health Network, Opinion
No Comments »

 Is poverty the major factor underlying geographic variation in health care? It assuredly is. There is abundant evidence that poverty is strongly associated with poor health status, greater per capita health care spending, more hospital readmissions and poorer outcomes. It is the single strongest factor in variation in health care and the single greatest contributor to “excess” health care spending. It should be the focus of health care reform but, sadly, many provisions in the current bills will worsen the problem.
Is poverty the major factor underlying geographic variation in health care? It assuredly is. There is abundant evidence that poverty is strongly associated with poor health status, greater per capita health care spending, more hospital readmissions and poorer outcomes. It is the single strongest factor in variation in health care and the single greatest contributor to “excess” health care spending. It should be the focus of health care reform but, sadly, many provisions in the current bills will worsen the problem.
Much of this is discussed elsewhere on this blog and in our recent “Report to The President and The Congress.” In this posting, I would simply like to tap into your common sense. We all know that poverty is geographic. There are wealthy neighborhoods and impoverished ones, rich states and poor ones, developed countries and developing ones. Sometimes poverty is regional, as in Mississippi, but sometimes it’s confined to “poverty ghettos,” as in the South Bronx. Read more »
*This blog post was originally published at PHYSICIANS and HEALTH CARE REFORM Commentaries and Controversies*






 Is poverty the major factor underlying geographic variation in health care? It assuredly is. There is abundant evidence that poverty is strongly associated with poor health status, greater per capita health care spending, more hospital readmissions and poorer outcomes. It is the single strongest factor in variation in health care and the single greatest contributor to “excess” health care spending. It should be the focus of health care reform but, sadly, many provisions in the current bills will worsen the problem.
Is poverty the major factor underlying geographic variation in health care? It assuredly is. There is abundant evidence that poverty is strongly associated with poor health status, greater per capita health care spending, more hospital readmissions and poorer outcomes. It is the single strongest factor in variation in health care and the single greatest contributor to “excess” health care spending. It should be the focus of health care reform but, sadly, many provisions in the current bills will worsen the problem.







