August 13th, 2009 by admin in Better Health Network, Quackery Exposed
No Comments »

Astrology with Needles
by Ben Kavoussi, MS, MSOM, LAc
The following is an excerpt of an upcoming article called “The Untold Story of Acupuncture.” It is scheduled to be published in December 2009 in Focus in Alternative and Complementary Therapies (FACT), a review journal that presents the evidence on alternative medicine in an analytical and impartial manner. It argues that if the effects of “real” and “sham” acupuncture do not significantly differ in well-conducted trials, it is because traditional theories for selecting points and means of stimulation are not based on an empirical rationale, but on ancient cosmology, astrology and mythology. These theories significantly resemble those that underlined European and Islamic astrological medicine and bloodletting in the Middle-Ages. In addition, the alleged predominance of acupuncture amongst the scholarly medical traditions of China is not supported by evidence, given that for most of China’s long medical history, needling, bloodletting and cautery were largely practiced by itinerant and illiterate folk-healers, and frowned upon by the learned physicians who favored the use of pharmacopoeia.
Heaven is covered with constellations, Earth with waterways, and man with channels.
Yellow Emperor’s Canon of Medicine (黄帝内经, huang di nei jing)1
Acupuncture is presumed to have its origins in blood ritual, magic tattooing and body piercing associated with Neolithic healing practices.2,3 The Neolithic origin hypothesis is supported by the presence of nonfigurative tattoos on the Tyrolean Ice Man–an inhabitant of the Oetztal Alps in Europe–whose naturally preserved 5,200-year-old body displays a set of small cross-shaped tattoos that are located significantly proximal to classical acupuncture points. Medical imaging shows that the middle-aged man suffered from lumbar arthrosis and the cross-shaped tattoos are located at points traditionally indicated for this condition.4,5 Similar nonfigurative tattoos and evidence of therapeutic tattooing, lancing and blood ritual have been found throughout the Ancient world, including the Americas.6,7,8 Health-related tattoos are still prevalent in Tibet, where specific points on the body are needled with a blend of medicinal herbs in the dyes. These practices appear to be largely intended to maintain balance with the natural and spiritual worlds, and also to protect against demonic infestation and malevolence. Seemingly, this Neolithic and Bronze Age lancing heritage, which was intertwined with magic and animism has evolved in various cultures into codified systems of lancing and venesection for assuring good health and longevity. In addition to treating the impurity or superabundance of blood, in various cultures lancing was also believed to affect the flow of a numinous life-force that is, for instance, called qi (or chi, 氣, pronounced “chee”) in Chinese, prāna (प्राण) in Sanskrit, pneuma (πνεύμα) in Greek, etc.9 In many instances, elements of metaphysics, mythology, mysticism, magic, shamanism, exorcism, astrology and empirical medicine intimately intertwined, making it difficult for modern scholars to interpret them as mutually exclusive categories.
In China, for instance, the numinous force was believed to mirror the Sun’s annual journey through the Ecliptic-meaning its apparent path on the celestial sphere–and to circulate in a network of 12 primary jing luo (經络) known in English as the chinglo channels or simply channels or meridians (a term coined in 1939 by George Soulié de Morant, a French diplomat). These imaginary pathways run from head to toes and interconnect around 360 primary points on the skin.10 There is a strong possibility that the web of these channels was a rudimentary model of the vascular system that was conceptualized according to an episteme-meaning a set of fundamental beliefs-that was based on astrological principles and solar mythology. This episteme also indicated that a person’s health and destiny are determined by the position of the Sun, the Moon, the 5 Planets and the apparition of comets, along with the person’s time of birth.11 In this worldview, each body segment corresponds to one of the 12 Houses of the Chinese zodiac system di zhi (地支) known in English as the Earthly Branches, and which consists of 12 two-hour (30°) divisions of the Ecliptic. The channels are therefore named according to their degree of yin (阴) and yang (阳), from tai yang (太阳) to jue yin (厥阴), which are terms that describe the phases and the positions of the Sun and the Moon.12 Each has five special points designated by the characters 水 (Water), 木 (Wood), 火 (Fire), 土 (Earth) and 金 (Metal) which are also the Chinese terms for Mercury, Jupiter, Mars, Saturn and Venus13, and seem to correspond to the transit positions of these Planets in the matching House. Each point is also associated with a color, which comes from the visual appearance of the matching Planet in the night sky. Venus is white, Jupiter blue-green, Saturn golden-yellow, Mars red, and Mercury “black,” for it appears to be the dimmest of the five. Each of these points has also an occult connection with a direction, a segment of time, a season, a number set, a taste, a musical note, an internal organ, a body region, etc, in an ancient Chinese metaphysical cosmology often referred to as “correlative cosmology”14 and reminiscent of the esoteric and mystical beliefs held by Pythagoras of Samos (c. 580-c. 490 BC) and his followers, the Pythagoreans.15 In his occult and magico-mystical worldview, the nature of the life-force qi is often described in such terms16:
The major premise of Chinese medical theory is that all the forms of life in the universe are animated by an essential life-force or vital energy called qi. Qi also means “breath” and air and is similar to the Hindu concept of prāna. Invisible, tasteless, odorless, and formless, qi nevertheless permeates the entire cosmos. Qi is transferable and transmutable; digestion extracts qi from food and drink and transfers it to the body, breathing extracts qi from air and transfers it to the lungs. When these two forms of qi meet in the blood-stream, they transmute to form human-qi, which then circulates throughout the body as vital energy. It is the quality and balance of your qi that determines your state of health and span of life.
Other texts refer to qi as a “cosmic spirit that pervades and enlivens all things”17 and “from which the world was created.”18 For instance, the alchemist Ko Hung (葛洪, 2nd – 3rd Century AD) writes that “Man is in qi and qi is in each human being. Heaven and Earth and the ten thousand things all require qi to stay alive. A person that knows how to allow qi to circulate will preserve himself and banish illness that might cause him harm.”19, 20 The belief in a “cosmological correlation” between its pathways in the body and the Houses of the Chinese zodiac seems to be based on health and safety beliefs in geocentric cosmology and the related doctrine of “as above, so below” which stipulated that everything in the Heavens has its counterpart on Earth and also in man.
The episteme of “as above, so below” and correlative cosmology were prevalent throughout the ancient world, from the Eastern Mediterranean cultures to Northern Europe. It is notably found in the relics of a collection of occult writings called the Corpus Hermetica which are believed to be compiled in Hellenistic Egypt during the 1st or 3rd century AD and are attributed to Hermes Trismegistus (”Thrice-great Hermes”), the Greek equivalent of the Egyptian god of wisdom, Thoth. The original text was presumably lost or destroyed during the systematic annihilation of non-Christian literature between the 4th and 6th centuries AD. Nonetheless, a section of it known as the Emerald Tablet survived and was translated into Arabic by the Muslim conquerors and later into Latin by John of Seville c. 1140 AD and by Philip of Tripoli c. 1243 AD. An Arabic version of the Tablet by the Muslim polymath and alchemist Abu Musa Jābir ibn Hayyān (أبو موسى جابر بن حيان , c. 721-c. 815 AD) states “That which is above is from that which is below, and that which is below is from that which is above, working the miracles of One.”21 Given the prevalence of this set of fundamental beliefs throughout the ancient world, it seems that the natural philosophy that has given rise to the underlying theories of acupuncture in China stems from the same set of beliefs in that were also prevalent along the Silk Road in Persia, Mesopotamia, Egypt and in Greece and that have influenced the health and safety beliefs of pre-Christian Europe, such as the Eastern Mediterranean mystery cults22, or the early Gnostic Christianity.23 This hypothesis is supported by a statement by Gregor (Gregorius) Reisch (c. 1467-1525) in Margarita Philosophica (Pearl of Wisdom), first published in 150324:
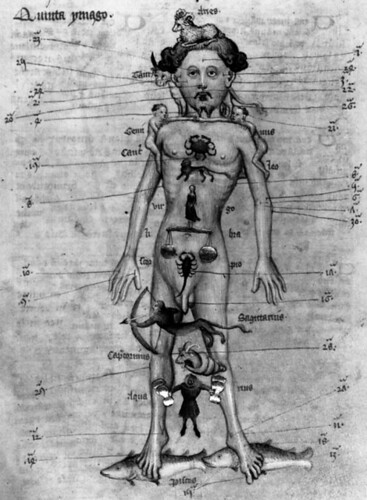
The pagans believed that the zodiac formed the body of the Grand Man of the Universe. This body, which they called the Macrocosm (the Great World), was divided into twelve major parts, one of which was under the control of the celestial powers reposing in each of the zodiacal constellations. Believing that the entire universal system was epitomized in man’s body, which they called the Microcosm (the Little World), they evolved that now familiar figure of “the cut-up man in the almanac” by allotting a sign of the zodiac to each of twelve major parts of the human body.
Figure 1: European medieval Zodiac Man form John de Foxton’s Liber Cosmographiae, published in 1408. It indicated the repartition of astrological influences on the body which physicians used to determine the auspicious time to let blood. Images courtesy of The Master and Fellows of Trinity College, Cambridge, UK.
Given this fundamental belief, European physicians Read more »
*This blog post was originally published at Science-Based Medicine*
August 11th, 2009 by Paul Auerbach, M.D. in Better Health Network, Health Tips
No Comments »

 One of the most dangerous times for a patient is during the transition, or “handoff,” between providers. This is due to a number of reasons. First, the original provider(s) may not relay all the information he or she knows about the patient to the next provider(s). Second, the accepting team may take it for granted that everything is known about the patient, and therefore not take a complete history or perform an adequate physical examination. Third, if the patient initially looks good, the accepting providers may be lulled into a false sense of security, and not anticipate a deterioration in the patient’s condition.
One of the most dangerous times for a patient is during the transition, or “handoff,” between providers. This is due to a number of reasons. First, the original provider(s) may not relay all the information he or she knows about the patient to the next provider(s). Second, the accepting team may take it for granted that everything is known about the patient, and therefore not take a complete history or perform an adequate physical examination. Third, if the patient initially looks good, the accepting providers may be lulled into a false sense of security, and not anticipate a deterioration in the patient’s condition.
We know this problem to exist in the hospital setting. Survey of doctors-in-training suggests that handoffs may commonly lead to patient harm. Last year (2008) in September, there was a blog written by Elizabeth Cooney in the Boston Globe that stated, “a 2006 survey of resident physicians at Massachusetts General Hospital found that handoffs commonly lead to patient harm, according to an article in The Joint Commission Journal on Quality and Patient Safety.” More than 50 percent “of the 161 medical or surgical residents who responded to the anonymous survey said they recalled at least one occasion in their last month-long rotation when a patient suffered from flawed handoffs.” Approximately “one in nine said the harm that resulted was significant.” The respondents said that “if the patient was coming from the emergency department or from another hospital, problematic handoffs were more likely.”
This holds true in the field. Unless the new treatment team makes the assumption that they need to begin their assessment of the patient’s condition from scratch, they are more likely to make a mistake. Obviously, such caution depends on the possible severity of the patient’s condition and the rescue/environmental situation. If I can get a decent handle on a patient’s condition, and there is little or no risk of me missing something, I will tailor my questioning and examination to suit the circumstances. However, I always start from the position that something has been hidden from me, of course not intentionally, and that the patient’s initial assessment has underestimated the problem(s).
I cannot begin to tell you how many times I have found something that was missed, or have accepted the care of a patient just as he or she began to “crash.” This is in no way a criticism of others, just a common fact of medical care. Previous rescuers may have been tired, the conditions may not have been conducive to a full examination, the patient may have been withholding information, or the situation may have just taken its natural course and worsened. Regardless, it’s my responsibility to learn what I can as quickly as I can about my patient, so that nothing slips through the cracks.
Here are some simple rules to follow:
1. If the situation permits, ask your new patient to repeat his or her history. If they are reticent to engage in a long conversation, at least try to get them to relate current relevant events.
2. Repeat as much of the physical examination as you can. Explain to the patient that you have assumed their care, and that in order to do the best that you can on their behalf, it’s important for you to understand their issues and to be able to monitor their progress based up the exam.
3. Assume that until you have talked to the patient or otherwise obtained a comprehensive history, and performed a physical examination with your own hands, eyes, and ears, that you do not know as much about your patient as you could.
4. If a patient is under your care for a prolonged time, or if you are managing a situation prone to rapid or undetected deterioration, interview and examine your patient as often as is necessary and practical. If you must be absent from a patient for a longer period than is prudent between examinations, delegate the responsibility to someone else.
image of leg splinting courtesy of www.princeton.edu
This post, Dropping The Ball In Patient Care: Provider Handoffs, was originally published on
Healthine.com by Paul Auerbach, M.D..
July 2nd, 2009 by Steve Novella, M.D. in Better Health Network, Quackery Exposed
No Comments »

When patients ask me if a chiropractor can help them with their problem, I often think to myself, “OK, do I give them the short answer or the long answer?” The difficulty is often in the fact that chiropractic is a diverse profession and it is difficult to even characterize what a “typical” chiropractor is likely to do. As a chiropractor once admitted to me – there are a great many things that happen under the umbrella of “chiropractic.”
In this article I will summarize some of the history and practice of chiropractic, highlighting what I consider to be many of the enduring problems with this profession.
History
Chiropractic was founded in 1895 by Daniel David Palmer, a grocer with an intense interest in metaphysics. Prior to his “discovery” of chiropractic, D.D. Palmer was a magnetic healer. He also had interests in phrenology (diagnosing disease based on the bumps of the skull) and spiritualism. Palmer reported to have discovered the principle of chiropractic when he allegedly cured a janitor of his deafness by manipulating his neck. The fact that the nerve which conveys sound information from the ears to the brain does not pass through the neck did not seem to bother Palmer, if he was even aware of this fact.
Palmer created the term “chiropractic,” which literally means “done by hand,” to refer to his new therapy. He argued that all disease is caused by subluxated bones, which 95% of the time are spinal bones, and which disrupt the flow of innate intelligence. He did not subject his ideas to any form of research, but rather went directly to treating patients and to teaching his principles to the first generation of chiropractors.
Subluxation Theory
Palmer believed in the pre-scientific vitalistic notion that health stems from the flow of a spiritual life force. Although vitalism was rapidly declining within scientific thought by the end of the 19th century, it was the centerpiece of early philosophies of health in most cultures. Palmer borrowed this ancient belief and renamed it “innate intelligence” which he claimed flowed from the brain to the rest of the body through the spinal cord and peripheral nerves. All disease, he argued, results from disruption in the flow of innate intelligence. Disruption in flow is caused by spinal subluxations, which are small misalignments in the spine that compress the spinal nerves.
Therefore, liver disease is caused by a subluxation which compresses the spinal nerve which supplies the liver with life force, depriving it of its vital innate intelligence. Palmer therefore believed he could cure by fixing these misalignments with manipulation.
This idea has remained the cornerstone of chiropractic despite advances in neurobiology and anatomy which have failed to show any evidence for innate intelligence or chiropractic subluxations. Many continue to ascribe all disease to the blockage of innate intelligence despite scientific advances in medicine which have discovered infectious, genetic, autoimmune, degenerative, nutritional, and other causes for many of the diseases which plague mankind.
Chiropractic was also not the only tradition based upon manipulating the bones. Of note, osteopathic doctors also developed an art of bone manipulation in order to heal, but they believed they were unblocking blood flow through arteries. Osteopathy and chiropractic had similar roots, but took very different paths, as we will see.
D.D. Palmer’s son, B.J. Palmer, became involved in the chiropractic movement early on, during the formative years. B.J shared his father’s metaphysical bent (prior to chiropractic, he worked with a mesmerist and worked in the circus), his tendency to make sweeping statements about health without justification, and his ignorance of contemporary scientific knowledge. He was reported to state, for example, “When I saw there was no use for a sympathetic nervous system, I threw it out, and then just had to put something better in its place, so I discovered Direct Mental Impulse.” B.J. also “discovered” a non-existent “Duct of Palmer” connecting the spleen to the stomach. In 1907 B.J. engineered a hostile take over of his father’s school of chiropractic.
B.J. Palmer set the tone that would later dominate the field of chiropractic. He emphasized salesmanship, advertising, and practice building. He was highly critical of medicine, stating that M.D. stands for “more death.” He continuously sought new methods for increasing revenues, such as his neurocalometer, which would pinpoint subluxations by measuring skin temperature and he decreed must be rented from him by other practitioners at exorbitant fees.
From the beginning chiropractors were also politically aggressive. They sought licensure as a protection from the growing scientific medicine with which they were completely at odds. Many legislators were reluctant to license chiropractors for this reason, but as more and more states voted in licensure, it became increasingly difficult to fight. Additionally, many legislators looked upon licensure as way of controlling the scope of chiropractic. By 1925, 32 states had instituted licenses for chiropractors. The struggle ended in 1974 when Louisiana instituted licensing.
Many states then began to pass basic science board requirements for licensure, making chiropractors pass the same tests of basic science knowledge as medical and osteopathic students. This was justified by the fact that chiropractors were presenting themselves as primary practitioners. However, where roughly 86 percent of medical students passed their basic science boards between 1927 and 1953, only 23 percent of chiropractors did. Chiropractors who could not pass the boards either moved to another state without the requirement, or practiced without a license. Between 1967 and 1979 all of the basic science laws for chiropractors were repealed.
Over the years chiropractic has never ceased its tireless struggle for growth and acceptance. Despite the fact that scientific medicine has continued to progress and chiropractic has never shed its pseudoscientific origins, they have been quite successful. After licensure, they gained coverage under Medicare. They have also successfully sued the AMA to stop their antichiropractic campaign. Today they continue to lobby hard for increased coverage and access under health insurance and HMO policies.
Straights, Mixers, and Reformers
Almost since the beginning, chiropractic has been fraught with many internal schisms. Today there is a wide range of differences between individual chiropractors, but most can be placed within one of three basic types.
Straight chiropractors consider themselves the only true or pure chiropractors because they limit their practice to the identification and treatment of spinal subluxations. They adhere strictly to Palmer’s concept of disease and believe that all ailments can be treated through manipulation to restore the flow of innate intelligence. Once freely flowing, they believe innate intelligence has unlimited power to naturally heal the body.
Straight chiropractors are the most extreme in their anti-scientific views. They openly advocate a philosophical rather than a scientific basis for health care, calling mainstream medicine “mechanistic” and “allopathic.” They call physicians “drug pushers” and disparage the use of surgery. They are careful not to give diseases names, but none-the-less they claim to cure disease with their adjustments. They oppose vaccinations. They also openly advocate the replacement of scientific medicine with chiropractic as primary health care. The statements of Dr. Wilson A. Morgan (who just passed away earlier this month), previous Executive Officer of Life College School of Chiropractic, are typical:
“Chiropractic: The health care system whose time as the official guardian of the public’s health is fast approaching!”
“On the other hand, it is equally appropriate for chiropractors to be viewed as generalists in that the far-reaching effects of their highly specific spinal adjustments usually are followed by the decrease and often disappearance of a very broad array of symptoms, disabilities and pathological conditions.”
“Unlike the medical profession, chiropractic has a very strong philosophical basis, which no doubt has contributed to its having been labeled ‘unscientific’ by the more mechanistically-oriented scientific community.”
“It appears that education will prove to be the best strategy in the ‘war on drugs,’ including education about the dangers of drugs available on the street and also those available from the physician as prescriptions.”
Mixers, comprising the largest segment of chiropractors, may at first seem more rational. They accept that some disease is caused by infection or other causes and they do not limit their practice to fixing subluxations. Most chiropractors in this group, however, do not supplement subluxation theory with scientific medicine, but rather with an eclectic array of pseudoscientific alternative practices. Mixers commonly prescribe homeopathic and herbal remedies, practice acupuncture and therapeutic touch, diagnose with iridology, contour analysis, and applied kinesiology, and adhere to the philosophy of naturopathy. This broad use of unproven, unscientific, and fanciful so-called “alternative” practices clearly indicates an antiscience attitude, as well as a lack of scientific knowledge, on the part of those chiropractors who employ them.
The rhetoric of Mixers indicates that they are attempting to become accepted into the scientific mainstream, rather than replace scientifically based medicine with a philosophy based approach. They no longer openly oppose immunization, like straights do, but they do advocate the freedom to choose whether or not to be immunized. Their appeal to freedom is emotionally effective, especially in the United States, but it fails to recognize that immunization is far less effective in eliminating or containing infectious diseases when it is not given to everyone. They also advocate a role for chiropractors as a primary care portal of entry system within HealthCare, despite the fact that they lack adequate training as generalists skilled in medical diagnosis.
A small minority of chiropractors, numbering only about 1,000, or 2% of all chiropractors (these are rough estimates because accurate figures are lacking), have been openly critical of their own field. They have called for absolute rejection of the subluxation theory of illness, disposing of pseudoscientific and unethical practices by chiropractors, and the restriction of chiropractic to treating acute musculoskeletal symptoms. They are attempting to bring their field into the scientific mainstream.
Occasionally chiropractic reformers have attempted to forge a new profession, entirely shedding the pseudoscience attached to the chiropractic brand. About ten years ago one group in Canada renamed themselves “Orthopractors,” and considered the new discipline of orthopractic as distinct from chiropractic. Orthopractic is the use of manipulation to provide symptomatic relief from uncomplicated acute back strain. They do not believe in maintenance therapy, treating medical ailments, or the use of pseudoscientific alternative practices.
Unfortunately, this reform effort died because “orthopractic” did not exist as a legal entity. This also partly explains why the “chiropractic” label persists and covers such a wide range of philosophy and practice – because it exists as a recognized licensed profession. It has a regulatory inertia that is hard to combat.
To further complicate things, spinal manipulation exists outside of the chiropractic profession, and not all manipulation is chiropractic manipulation. Some physiatrists, sports medicine doctors, and osteopaths legitimately employ manipulative therapy to relieve muscle strain, mobilize joints, and improve function. Chiropractors do this as well. But some chiropractors also do chiropractic manipulation designed to realign the spine and reduce imaginary chiropractic subluxations.
The Evidence – Subluxations
In the past 100 years, there has been very little research conducted into the basic principles of straight chiropractic. There is no research that indicates the existence of innate intelligence or that such a force plays any role in health and disease. Further, the evidence strongly suggests that chiropractic subluxations are a figment of the chiropractic imagination. And it also seems that spinal manipulation is not capable of realigning the vertebra of the spine.
A study carried out by Edmund Crelin, Ph.D. investigated the amount of force necessary to displace vertebral bones of the spine in order to cause impingement of a spinal nerve. The study was carried out on six corpses within 8 hours after death. His conclusion was that the amount of force necessary to actually displace the vertebra was great enough to break the spine, arguing strongly that chiropractic manipulation cannot significantly affect spinal alignment, and that misaligned spines do not caused pinched nerves (Crelin, 1973).
Pinched or impinged spinal nerves do occur, but they are caused by herniated discs, fractures, tumors, or overgrowth of the vertebral bones. When spinal nerves are impinged they cause pain, numbness, and tingling and may cause a decrease or loss of deep tendon reflexes and weakness of the muscles supplied by the affected nerve. Impinged nerves are not caused by subluxations nor do they result in diseases of the organs. Believers in subluxation theory must claim, implausibly, that nerve impingement causes only a blockage of innate intelligence without causing any of the known signs and symptoms of such impingement.
Ironically, spinal manipulation is contraindicated in cases of actual nerve impingement and should not be performed. In medical studies of manipulation, such as the RAND study, often cited by chiropractors as evidence for manipulation, spinal nerve impingement was considered a reason not to have manipulation and therefore was a criteria for exclusion from the study.
Another source of evidence that the chiropractic theory of subluxations and innate intelligence is completely false comes from the unfortunate victims of spinal trauma. There are many victims of complete transection, or disruption, of the cervical spinal cord in the neck. Such a complete injury leaves its victim quadraplegic, unable to move the arms or legs. If the injury is high enough in the spinal cord the victim may not even be able to breath on their own. In such victims no impulses from the brain are able to travel below the spinal cord in the neck, and therefore most of the communication between the brain and the body is interrupted. Certainly, this is a much more dramatic and complete interference of nerve flow than that of an impinged spinal nerve.
Yet, in these patients, the organs continue to work without difficulty and diseases do not develop at any higher rate than those without such an injury. Of course, there are some effects from the disruption of the autonomic nervous system, that part of the nervous system which regulates the bladder, the degree of bowel motility, and other functions. But all effects of spinal cord damage are caused by known neurological injury. If subluxation theory were correct, then patients with high spinal cord injuries would be ravaged by every conceivable disease.
So chiropractors cannot realign the spine to fix imaginary subluxations and restore the flow of nonexistent innate intelligence. Subluxation theory is pure pseudoscience, like homeopathy or therapeutic touch, and has no place in a 21st century scientific health care system.
Despite the extreme scientific implausibility of subluxation theory, specific applications have been tested with clinical research – with predictable results. For example, many chiropractors will use manipulation to treat asthma is children. The results of this research are soundly negative – chiropractic does not work on asthma.
Despite this many chiropractors persist in treating asthma. This led Simon Singh to write in the Guardian in 2008 that the British Chiropractic Association, which does advocate chiropractic for childhood asthma, “promotes bogus therapies.” In response to this statement the BCA notably did not provide the evidence that Singh claimed was missing. Rather, they sued him for libel (the case is ongoing).
Next week I will cover the evidence for musculoskeletal uses of chiropractic.
*This blog post was originally published at Science-Based Medicine*
May 26th, 2009 by Medgadget in Better Health Network
2 Comments »


“.. imagine it is the tool with which you are about to remove a man’s limb. This is a dark, sombre instrument, with serious purpose.”
We don’t often unbox things here at Medgadget. For whatever reason, Phillips and GE keep forgetting to mail us their latest CT scanners for review. And Intuitive Surgical, where’s our da Vinci? We need something to make our morning lattes. That being said, recently we got our hands on a wonderfully preserved, rare 1800s surgical kit, made by the famous pre-civil war surgical equipment manufacturer Henry Schively out of Philadelphia, PA. We thought we’d use this opportunity to reminisce on surgery of the past, you know, before ether was given a try, and when surgeons could operate in formal attire. To help us on our voyage through the kit, Medgadget has enlisted our friend Dr. Laurie Slater, whose website Phisick showcases a formidable collection of medical and surgical antiques. Being more knowledgeable on such matters than us, he has kindly offered to act as our guide. From the confines of this post / interview, we’ll explore the surgical kit, touch on surgery in the 1800s, and get you thinking about the days when you’d probably dress like these gentlemen.
So let’s get started. Hinge opening… Now.

Dr. Slater, thank you for kindly serving as our guide through this kit.
You are very welcome. I’m delighted to be able to get a first hand look at this lovely surgical set, so thanks for asking me.
Before we dig into our kit, tell us a bit about why you started collecting medical antiques? What prompted you to start Phisick and where did the word ‘Phisick’ come from?
What I first thought would be a passing interest was not. I come from an era of medicine where much of the equipment tends to be plastic and throw-away. The first time I set eyes on some of the older surgical instruments, I was bowled over by the incredible workmanship and the painstaking effort which someone had lavished on them. I remember thinking that whoever had constructed them a) knew what they were doing and b) was in no hurry. They were of the highest quality, made from the finest materials, with a mastery of design and engineering which, I fancied, would have challenged the legendary skill of the elfin silversmiths of Lothlorien. They had function, obviously, but also form.
Take for example the capital saw (the large one) in your set. The handle is made from dark black smooth ebony which is a durable hardwood, polished and oiled over many hours to a smooth waterproof finish. The curve of the handle is simple, but with a design reminiscent of something from the animal kingdom. Well weighted in the hand; the inner curve fitting the surgeons grip and the upper ‘fin’ and lower ‘fish tail’ anchoring the palm to the handle. This, along with the crosshatching will prevent any slippage when the teeth of the the cold polished steel meet with bone.
Stop for a moment and have another look, but this time imagine that this instrument is about to saw through your own leg without anaesthetic. Or look at it from the surgeon’s point of view and imagine it is the tool with which you are about to remove a man’s limb. This is a dark, sombre instrument, with serious purpose.
An appreciation of these instruments and the men who designed and constructed them has helped me see medicine and history in a different light, and an altogether more vibrant context.
About “Phisick”… The word was commonplace in the 1500s and synonymous with our current day “medicine.” Spelling back then was fairly relaxed and no-one much worried about interchanging a “y” for an “i”. You could ‘take phisick’ by swallowing a pill, or doctors could ‘practise phisick’ by trying to cure their patients. So this was the name I chose for a website which celebrates the beautiful, breathtaking, sometimes life-giving tools invented by the pioneers of medicine and surgery.
 We’re fortunate to know a bit of history behind this set. It belonged to a Dr. Geo L. Shearer (an ancient relative of one of your editors), who practiced medicine in Dillsburg, Pennsylvania from 1825 to 1878. Were such personal surgical kits normal possession of doctors in that era?
We’re fortunate to know a bit of history behind this set. It belonged to a Dr. Geo L. Shearer (an ancient relative of one of your editors), who practiced medicine in Dillsburg, Pennsylvania from 1825 to 1878. Were such personal surgical kits normal possession of doctors in that era?
Knowing who the owner really brings this piece to life. I found a great account of Dr. George L Shearer and which included his role in the history of Dillsburg. The census in 2000 listed the population of Dillsburg at 2063, but when he first started there this figure was closer to 600. He was clearly a pillar of his local society – Chief Burgess of the borough, School Director, member of the Town Council and active in securing the Borough Charter, the State Road from Dillsburg to York, and the railroad. But for the people living there he would have been first and foremost their doctor. The author of this account of Dillsburg describes his “passing from time into eternity” in 1878 and he is also mentioned in his son’s obituary as “The beloved physician” so he was clearly held in both warm and high esteem.
The surgical set you have here in style and configuration is no later than 1840 and predates the civil war by over 20 years which raises the possibility that as the owner, he might have had some prior surgical training. However, the amount of use it would have had at the hands of a local doctor in a small town would have been pretty limited and it seems more likely that if this set had seen much use that it would have done so during the years of the Civil War. During the Gettysburg Campaign, Dillsburg was twice invaded by Confederate cavalry at which time Dr Shearer would have been 61. If he had performed surgery at this time he would have done so in one of two roles, either as a militia surgeon, or a contracted private surgeon. At the start of the war the army forces on either side had their own army surgeons, those of the Union forces numbered 113, of which 24 joined the Confederates. Such were the terrible casualties in an engagement managed by pre-war strategies designed to suit professional soldiers, but acted out by massive numbers of poorly trained civilian recruits, that by the end of the war over 15,000 surgeons had been required to serve in the army forces of either side. Bollet, a civil war historian writes about this:
“During the first year of the war, and especially during the Peninsula Campaign in 1862, army surgeons performed all operations. Soon the overwhelming numbers of battle wounded forced the army to contract civilian surgeons to perform operations in the field alongside their army counterparts. Their ability ranged from poor to excellent.”
In fact, because of controversy over the staggering number of casualties, strict rules were put in place to ensure that only experienced surgeons could operate and one figure suggests that only one in fifteen doctors performed amputation surgery. If Dr Shearer had had such a role he might have used this set to treat both wounded local conscripts from his home town (the number varied in the account I have read but was circa 30 of which 8 died) or soldiers with war wounds (who would have numbered considerably more). In fact, neither George L. Shearer nor his son, James M. Shearer are listed in the A.M.A. Deceased Physicians database. This in itself is not uncommon. Nor is he listed as a surgeon or asst. surgeon in the Roster of Regimental Surgeons for the Union Army, (but he would not have been of course unless he had actively joined the Union Army). Interestingly his son James M. Shearer is listed in the Roster as an assistant surgeon from Dillsburgh, Pa., who served until Aug. 1863. with the Pennsylvania 12th Reserves Infantry, (41st. Volunteers.) Nor is George L mentioned in the Medical and Surgical History of the War of Rebellion. So without any corroborative evidence that he was a surgeon in the Civil war it is not possible to say that this is a civil war surgical set, but the story as it has unfolded so far raises some fascinating possibilities.
In general, how would surgery be done in the 1800s? Would doctors ever operate on house calls? Any sort of anesthetics?
Dr Shearer practiced medicine in Dillsburg and to the six hundred residents of this backwater town in Pennsylvania he would also have been their physician, surgeon, gynaecologist, obstetrician and paediatrician. This heavy set contains instruments used for major surgery such as amputation or craniotomy. In practice, in a town of Dillsburg’s size, outside of war, either of these operations would have been very rare and I doubt it would have seen a great deal of use in this context. It certainly would not have been carried with him on any regular basis. Most likely he would have had another medical bag or physicians leather pocket case in which the more common instruments in daily use were contained and which he would have taken on his house calls. The sort of surgery he might have undertaken would have been suturing of wounds, the drainage of an abscess or possibly the treatment of a superficial flesh would from a bullet (likewise not a common injury in peacetime). He might have used the smaller knives, forceps and needles in the set for this. Local anaesthetic was not invented until the 1880s and none of these procedures wound would have merited ether or chloroform and so would have been done without anaesthetic.
With regards to surgery, the turning point in the 1800s was circa 1846, with the introduction of anaesthesia. Prior to this time the use of an orderly to hold the patient down and alcohol or opium was a poor substitute, and meant that only absolutely major surgery could be undertaken. By far the most common operation was amputation, but also craniotomy (drilling holes in heads – which I will talk about later) and also the removal of bladder stones. The imperative in any case where the patient was conscious would have been to perform surgery as quickly as possible and the earlier surgeons prided themselves in the speed at which they could operate, some claiming to be able to remove a leg in under one minute!
After the introduction of anaesthesia there was a rising tide of surgical procedures. Most of them however would have been done in the civilian hospitals. In Massachusetts Hospital there were a mere 39 operations carried out in the 10 years prior to 1846 and 189 operations (60% of them were amputations) in the 10 years post. It was not until the turn of the century however with the introduction of antisepsis and asepsis that the volume increased significantly by which time in Massachusetts they were averaging 2,427 operations each year.
During the civil war it was estimated that as many as 60,000 amputations were performed on both sides. Because of horrific casualties of war and their appalling prognosis, the surgeons of the time were given pretty bad press and held in poor esteem by the public. Rumours abounded that amputations were performed needlessly, even though this was almost certainly not the case. Surgeons were also accused of performing amputation without anaesthetic. With the notable exception in 1862 of 254 casualties at the battle of Luka, this was not true either, but the reason such accusations exist have explanation. Most of the amputations were performed outside because sunlight afforded by far the best illumination and so many procedures were done in public view of “passers by.” The anaesthetic would be applied by placing a cloth over the nose and face which had been soaked in either ether, or chloroform or a mixture of the two. As soon as the patient passed out the cloth was removed and this would have afforded only a relatively light anaesthetic. (And probably just as well because had it been held in place longer, fewer patients may have woken up). However, the light anaesthetic meant that the patients would tend to thrash around during the procedure even whilst unconscious. It seems likely that the observation of such movements in a public forum would lead to the assumption of an untrained eye, that the patient was still awake.
Given that these kits were used many, many times, how common were infections as a result of surgical procedures in the 1800s?
Many of the surgical procedures done in the civil war were complicated by infection as they were done without the knowledge of the role that bacteria played or the benefits of antisepsis and asepsis. Hospitals of the time were characterised by the stench of the ubiquitous pus and infection. The overcrowded and unhygienic conditions made the situation worse. Thick creamy pus from staphylococcal infection was referred to as “laudable pus” because it tended to be local in nature. The more serious infection from streptococcal infection produced a clear watery or bloodstained discharge and was called malignant because it caused septicaemia and death, hospital gangrene and osteomyelitis. The latter was a chronic infection in bone which was a complication of the almost inevitable infections which followed broken bones exposed to the air. The presence of osteomyelitis was a common indication for amputation.

This particular kit was made by Henry Schively. Since we’re a medical technology blog, would you mind briefly telling us about the medical instruments manufactured in that era?
In the late 18th century most American surgeons were buying their instruments abroad, or from agents who had imported them from England. Henry Schively (1761 – 1811) is described in Edmonson’s book on American surgical instruments as ‘the Premier Philadelphia surgical instrument maker of the era of heroic surgery’ which was the period from 1774 to 1840. He along with a number of other local artisans (there were 50 master smiths registered in the thriving city of Philadelphia, 10 of whom were listed as “instrument makers”) contributed to Philadelphia becoming the centre of the American instrument trade. Supporting this development was the fact that Philadelphia and the surrounding regions had also become the leading American medical centre of the time, boasting the very first public anatomy lectures and dissections, as well as the first medical school, the university of Pennsylvania. The first surgical chair of this medical school was held by Philip Physick, the “father” of American surgery. Relatively few of these early master craftsmen managed to sustain successful businesses but Henry Schively and John Rohr were among the better known. Schively was famous for inventing the Bowie knife, although it was his focus on making surgical instruments which marked him out and he was approached by many surgeons, Physick amongst them to construct and refine instruments which they had invented. Schively and the family business later carried on by his son beyond 1850 was acknowledged in its time as one of the finest surgical instrument makers in America.

Here’s an overview of the kit showing all of the tools inside. Do you think this was a common, general surgical kit, or do you think it might have been for more specialized procedures?
The set contains the basic surgical tools which would have been needed to perform emergency surgery by way of amputation and this is not an uncommon configuration. The essential tools for this would usually comprise of a Liston knife or knives which had long straight razor sharp blades polished steel blades for cutting through the muscle. A capital saw (the large one) was for sawing through weight bearing bones. The forceps and smaller knives would have been used for trimming the muscle and skin in such a way as to produce flap. The needles were used to sew the flap of skin and muscle in place over the bone stump. There would also have been a tourniquet for applying pressure around the limb to temporarily cutt off the blood supply.
In addition to these surgical tools the set also contains two hand trephines and other instruments used for trepanation. These would often come separately in their own case and so this set represents a “compendium” if you like. Other examples of sets which combined instruments for different purposes were carried on board ships. These were grand compendia with comprehensive collections of tools to manage all eventualities, including general surgical, orthopaedic, urological, ophthalmological and dental instruments.

This is the trepanning set within the kit. Would you mind briefly describing why a doctor would perform trepanning and how he would do the procedure?
Trepanation is the procedure of drilling a hole in the skull. The two main reasons for doing this would be to drain a collection of blood which had accumulated between the skull and the surface of the brain, or to elevate a depressed bone fracture. The former, often referred to as a subdural haematoma would raise the pressure within the skull and cause brain damage, and in a depressed fracture it was the bone of the skull pushing on the brain (like a collapsed ping-pong ball) which would damage the brain or causes it to swell. When done correctly for the right indications trepanation is a relatively simple procedure which is life saving. This set contains two drills with different sized crowns (“drill bits”), either of which can be attached with a screw to the horizontal crosshatched ebony handle. This forms a drill which is used in a similar way to a cork screw. A flap of scalp would first have been raised to clear the area of the skull to be tapped. In order to anchor the circular drill and prevent slippage a central spike is moved forward and fixed in place to start the drilling (see here). The drill is turned through the cranium until a disk of bone can be removed. This may have been pried out with a lever like ‘elevator’ and the edges of bone trimmed with a sharp knife or ‘lenticular’ and filed down with a ‘raspatory’. The instrument on the top right hand side of the case would probably have been used as a combination of an elevator and raspatory. Sometimes one hole would be enough to drain a collection of blood. Other times a larger plate of skull would need to be removed and this was done by drilling three or more holes and passing a small abrasive wire (a Gigli saw) between two holes at a time to saw through the intersection.
 Tell us, if you could, about the the lancet and what they’d be used for? Why was a scalpel or normal knife not sufficient to let blood?
Tell us, if you could, about the the lancet and what they’d be used for? Why was a scalpel or normal knife not sufficient to let blood?
Patients were frequently bled by their physicians in the 19th century and this was considered a panacea for numerous complaints ranging from headaches to gout. It was almost certainly ineffective in 99.9% of them. One such phlebotomy instrument used was the “spring lancet”. The name is largely self explanatory. The device is primed by pulling the black lever which also moves the blade upwards and holds it in position under tension. The lower edge of the instrument is held over the area to be bled and it is fired by pressing the arm on the side which released the blade at speed into the flesh. The ensuing blood was usually collected in cups applied to the skin (see here). I doubt that this spring lancet came with the set originally but would have been a later addition. It is the sort of instrument Dr Shearer might well have carried on his person or in his medical bag. Physicians also used small knives and thumb lancets to do the bleeding but because the spring lancet was able to pass the blade through the skin more quickly, they were less painful. Later automatic devices called scarificators worked on similar principles but primed multiple blades at a time (see here).

The above vertebrae was found in the kit. Any idea why a surgeon might keep that around!?
This is a human cervical vertebra (from the neck). The central body has been drilled and so it almost certainly once belonged to an anatomical model skeleton. The reason it has found its way into this set is not obvious. The container in which it sits, along with the spring lancet is where the tourniquet for this set would have gone.

What do you think this little brush might have been used for?
This is a brush which would have been used to brush away the small pieces of skull bone which accumulated around the drill bit during trepanation. It is probably made from bone although it could be ivory. Although most of the pieces in the set are made from ebony it is possible that this was original as a number of items in the set do combine the two.

What about these saws? How do you think they might have been used? Amputations?
The top saw is called a Hey saw after William Hey an English surgeon (1736-1819). It is used to perform craniotomies, but instead of using a trepan, Hey removed a plate of bone by sawing linear intersecting lines through the skull. The middle saw we have talked about is called a capital saw and this is the large saw which would have been used in leg amputations to saw through the femur or tibia. The bottom one is called a metacarpal saw and would have been used to cut smaller bones in the forearm or hand or finger bones.
Anything else in the kit or about the kit that you’d like to comment on?
Just to reiterate that this is a superb very early surgical set made by one of the most famous American instrument makers and I am delighted to have had the opportunity to look at it and explore the history with you. American and civil war surgical instruments are not my specific area of expertise and so this exercise has been very educational and enjoyable one for me.
Thank you so much for helping us out! If our readers what to learn more about medical antiques, do you have any recommendations for books, or other resources (besides Phisick of course) that they might want to check out?
There are a number of good books on antique medical and surgical instruments which include:
Antique Medical Instruments by Elisabeth Bennion
American Surgical Instruments by James Edmonson
Medicine: Perspectives in History and Art by Robert Greenspan
For those with a more specific interest in Civil War surgical instruments I would recommend a trip to Michael Echols’ web site which reflects his wealth of knowledge on this subject. I particularly want to thank Michael for the help he graciously offered in researching this set.
I would also recommend reading Bollet’s illuminating article “The truth about Civil War surgery“.
Lastly your readers may be interested in browsing the links page at Phisick.com where they can find a number of sites related to medical antiques and the history of medicine.
*This blog post was originally published at Medgadget*
July 28th, 2008 by Dr. Val Jones in Expert Interviews
1 Comment »
At the recommendation of my dear friend and fellow blogger, Dr. Ramona Bates, I attended a lecture entitled, “Limb Labs: Getting Amputee Soldiers Back to Work After World War I.” The lecture was held at the National Museum of Health and Medicine on the Walter Reed campus in Washington, DC. Both lecturers (Beth Linker and Jeffrey Reznick) did a wonderful job of transporting the audience back in time, outlining the cultural beliefs and historical context of the day. This is what I gleaned from their commentary:
Roughly 100,000 men became amputees as a result of injuries from the American Civil War (1861-1865). At the time there was no government-sponsored program to fit amputees with prosthetic limbs, so veterans were on their own. Prosthetists catered to the middle and upper classes who paid cash for their custom prostheses. Veterans of lesser means could only afford a peg leg, and some would sell photos of their stumps (like baseball cards) to support themselves. Many veterans were not effectively reintegrated into the work force after their injuries, and were considered “charity cases” by the American public.
By the time World War I began, there was significant social stigma associated with amputation. Peg legs and hook arms were synonymous with “blood thirsty villains” like Captain Ahab from Moby Dick, and Captain Hook from Peter and Wendy. As America braced for a fresh round of young amputees, the government prepared occupational rehabilitation programs in an attempt to reduce deliquency among injured veterans. An entire PR engine was developed to set expectations that veterans would become “active workers, not charity cases.” And authors like John Galsworthy, began describing the vocational reintegration of war heroes as “sacred work.”
Around the turn of the 20th century, technology had advanced to allow mass production of various goods. Factories were created to produce large quantities of standardized items like clothing, and the corresponding reduction in cost revolutionized the standard of living for many poor and middle income Americans. Not surprisingly, enterprising individuals looked for ways to mass produce costly, custom products – and be the first to market with a new, affordable option.
Seizing on the opportunity that World War I created (i.e. a new market for prosthetic limbs), a couple of orthopedic surgeons recognized an opportunity to take over the prosthetic limb market by creating a “one size fits all” solution that they could sell to the government. The government was eager to avoid the costly mistakes of the Civil War (i.e. not having a plan for reintegrating young men into the work force), but couldn’t afford the prosthetist’s fee of $200 per custom prosthetic limb. The “E-Z leg” was born, and at a cost of only $20 per prosthesis, it seemed like a steal.
The E-Z leg solved a few problems for the government – 1) it allowed injured veterans to walk off the ships (instead of being carried on stretchers) that brought them home from Europe, thus minimizing the public appearance of the toll of war 2) it allowed them to offer cosmetically appealing prostheses, rather than peg legs, to amputees 3) it increased the vocational rehabilitation potential of veterans.
Of course, the “E-Z leg” didn’t have the best marketing ring to it, so it was rebranded the “liberty leg” and hailed as a triumph of modern technology. In reality, though, it wasn’t much of a functional improvement over a peg leg. In prosthetic design, a “one size fits all” approach ensures that no one gets a truly good custom fit. But psychologically, the veterans were pleased to have a cosmetically appealing limb, and most had no idea how much better a custom limb could be. The public was satisfied by the government’s generosity, not realizing that the government had actually budgeted $75/amputee at the beginning of the war. What happened to the $55 savings? We’ll never know.
One thing’s for sure, the orthopedist owners of E-Z leg made out like bandits. John Galsworthy became so disillusioned with his push for “sacred work” that he wrote, “Empty promises and rhetoric of heroism… The war killed the self-importance, faith and idealism in me.” He never spoke of vocational rehabilitation for war veterans again.
***
As I watched the NBC nightly news yesterday, I noted an interview with a young Marine recovering from bilateral leg amputations (caused by an IED explosion in Iraq) at Walter Reed. When asked if he was worried about walking again he simply replied, “I don’t worry about that. With the artificial legs they have these days, I’ll probably be better than ever.”
And I thought to myself, “the more things change, the more they stay the same.”This post originally appeared on Dr. Val’s blog at RevolutionHealth.com.








 We’re fortunate to know a bit of history behind this set. It belonged to a Dr. Geo L. Shearer (an ancient relative of one of your editors), who practiced medicine in Dillsburg, Pennsylvania from 1825 to 1878. Were such personal surgical kits normal possession of doctors in that era?
We’re fortunate to know a bit of history behind this set. It belonged to a Dr. Geo L. Shearer (an ancient relative of one of your editors), who practiced medicine in Dillsburg, Pennsylvania from 1825 to 1878. Were such personal surgical kits normal possession of doctors in that era?


 Tell us, if you could, about the the lancet and what they’d be used for? Why was a scalpel or normal knife not sufficient to let blood?
Tell us, if you could, about the the lancet and what they’d be used for? Why was a scalpel or normal knife not sufficient to let blood?










