June 2nd, 2011 by Toni Brayer, M.D. in Health Policy, Opinion
No Comments »

 It is my job at EverythingHealth to steer the reader to great information. For this reason I am providing you with a Link to The New England Journal of Medicine article titled “The $650 Billion Dollar question – why does cost effective care diffuse so slowly?” I have retitled it “Why Health Care Costs So Much”.
It is my job at EverythingHealth to steer the reader to great information. For this reason I am providing you with a Link to The New England Journal of Medicine article titled “The $650 Billion Dollar question – why does cost effective care diffuse so slowly?” I have retitled it “Why Health Care Costs So Much”.
The United States spends much more on health care than other industrialized nations with no improvement in outcomes or health status of it’s citizens. If we enacted some of the policies that other nations use, we would have $650 Billion to spend on education, infrastructure, social security and other societal needs. Why can’t we get there?
Read here to understand the barriers. It isn’t simple. Resistance to change and instituting cost effective care has many stakeholders including legislators, doctors, hospitals, drug and equipment manufacturers, academic training centers, insurance companies and even the media. We, the public, are also to blame for not understanding that reform which lowers costs would benefit all of us. There is no free lunch. When the cost of care goes up for employers, that keeps our wages stagnant. When millions are uninsured, the cost of their care is born by everyone and it is inefficient care.
The article authors tell us: Read more »
*This blog post was originally published at EverythingHealth*
June 1st, 2011 by RamonaBatesMD in Research
No Comments »

Have you ever lost your sense of smell or taste? Recall how it feels when your face/mouth don’t work properly until the nerve blocks wear off after a dental procedure.
Those are all things (and more) a facial transplant patient has to deal with. The article discussing recovery of sensation after facial transplantation in the May issue of Plastic and Reconstructive Surgery discusses this topic (first reference below).
In addition to reviewing their own face transplant patients (n=4), Dr. Maria Siemionow and colleagues did a literature review (English literature for peer-reviewed articles published between 1940 and 2010) of sensory recovery after various standard nerve repair techniques.
These other nerve repair techniques included repair of the peripheral branches of the trigeminal nerve; sensory return after free tissue transfer (ie noninnervated flaps, including radial forearm, lateral thigh, anterolateral thigh, latissimus dorsi, trapezius, et al and innervated free flaps, including radial forearm, anterolateral thigh, and rectus abdominis musculocutaneous flaps); and sensory recovery following replantation of scalp and forehead. Read more »
*This blog post was originally published at Suture for a Living*
June 1st, 2011 by Happy Hospitalist in Humor
1 Comment »

I’ve discovered the perfect tool to improve doctor-nurse communication skills. Let’s see. Hundreds of nurses. Dozens of floors. Day shifts. Night shifts. This pin pretty much sums it up. Any questions?

*This blog post was originally published at The Happy Hospitalist*
June 1st, 2011 by GarySchwitzer in Announcements, Medblogger Shout Outs
1 Comment »

Even if you’re not into blog rankings, Wikio.com’s ranked list includes links to many solid sites. This blog rose a bit in the rankings in the past month. We’re pleased to be included in a list of so many quality blogs.
Ranking made by Wikio
Wikio’s fine print on how ratings are compiled: Read more »
*This blog post was originally published at Gary Schwitzer's HealthNewsReview Blog*
June 1st, 2011 by Paul Auerbach, M.D. in Health Tips, Research
No Comments »

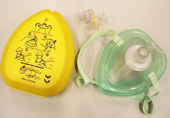 When a person performs cardiopulmonary (heart and lung) resuscitation (CPR), it is sometimes recommended to provide rescue breathing. This is certainly the case when the primary cause of the victim’s difficulty relates to failure to breathe adequately, such as with a drowning episode. When CPR first arrived on the landscape, laypersons were trained to perform mouth-to-mouth breathing (for adults) or mouth-to-mouth and nose breathing (for infants and small children).
When a person performs cardiopulmonary (heart and lung) resuscitation (CPR), it is sometimes recommended to provide rescue breathing. This is certainly the case when the primary cause of the victim’s difficulty relates to failure to breathe adequately, such as with a drowning episode. When CPR first arrived on the landscape, laypersons were trained to perform mouth-to-mouth breathing (for adults) or mouth-to-mouth and nose breathing (for infants and small children).
Following growing concern about transmission of diseases from blood and body fluids, laypersons were introduced to using masks or something similar to allow them to provide breathing assistance (“artificial respiration,” “artificial ventilation,” “rescue breathing,” etc.) to non-breathing persons. Masks have been used for decades by professional rescuers for ventilating patients, often in conjunction with the use of bags in a “bag-valve-mask” configuration. The valve between the mask and bag provides for one-way flow and prevents the backwash of vomitus, blood, liquid from the lungs, or other fluids that might diminish the effectiveness of the technique.
A number of excellent masks and face shields are available on the market for rescuers to be able to (relatively) safely blow air into a victim’s lungs. One example is Read more »
This post, CPR: Mouth-to-Mouth Breathing May Have Some Advantages Over Mask-Assisted Breathing, was originally published on
Healthine.com by Paul Auerbach, M.D..
 It is my job at EverythingHealth to steer the reader to great information. For this reason I am providing you with a Link to The New England Journal of Medicine article titled “The $650 Billion Dollar question – why does cost effective care diffuse so slowly?” I have retitled it “Why Health Care Costs So Much”.
It is my job at EverythingHealth to steer the reader to great information. For this reason I am providing you with a Link to The New England Journal of Medicine article titled “The $650 Billion Dollar question – why does cost effective care diffuse so slowly?” I have retitled it “Why Health Care Costs So Much”.






 When a person performs cardiopulmonary (heart and lung) resuscitation (CPR), it is sometimes recommended to provide rescue breathing. This is certainly the case when the primary cause of the victim’s difficulty relates to failure to breathe adequately, such as with a drowning episode. When CPR first arrived on the landscape, laypersons were trained to perform mouth-to-mouth breathing (for adults) or mouth-to-mouth and nose breathing (for infants and small children).
When a person performs cardiopulmonary (heart and lung) resuscitation (CPR), it is sometimes recommended to provide rescue breathing. This is certainly the case when the primary cause of the victim’s difficulty relates to failure to breathe adequately, such as with a drowning episode. When CPR first arrived on the landscape, laypersons were trained to perform mouth-to-mouth breathing (for adults) or mouth-to-mouth and nose breathing (for infants and small children).







