March 3rd, 2011 by Dinah Miller, M.D. in Opinion, Research
1 Comment »




[Recently] in The New York Times, David Tuller [wrote] about a study published in The Lancet that shows that psychotherapy is an effective treatment for chronic fatigue syndrome. In his article “Psychotherapy Eases Chronic Fatigue, Study Shows,” Tuller writes:
The new study, conducted at clinics in Britain and financed by that country’s government, is expected to lend ammunition to those who think the disease is primarily psychological or related to stress.
The authors note that the goal of cognitive behavioral therapy, the type of psychotherapy tested in the study, is to change the psychological factors “assumed to be responsible for perpetuation of the participant’s symptoms and disability.”
In the long-awaited study, patients who were randomly assigned to receive cognitive behavioral therapy or exercise therapy, in combination with specialized medical care, reported reduced fatigue levels and greater improvement in physical functioning than those receiving the medical care alone — or getting the medical care along with training in how to recognize the onset of fatigue and to adjust their activities accordingly.
Interesting. Generally I like to stay away from the “it’s all in your head” debates. I’ll let the commenters do the talking here.
*This blog post was originally published at Shrink Rap*
March 3rd, 2011 by Linda Burke-Galloway, M.D. in Better Health Network, Health Tips
No Comments »

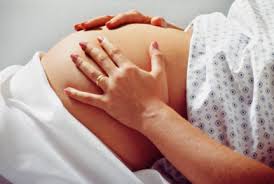 Having a baby can be a beautiful thing until something goes wrong. The tragedy is that many high-risk conditions can be managed appropriately if the patient is cooperative and the healthcare provider is competent and well trained. Unfortunately, almost 600 pregnant women die in the U.S. each year from complications and the most common complication is significant blood loss after birth or postpartum hemorrhage (PPH).
Having a baby can be a beautiful thing until something goes wrong. The tragedy is that many high-risk conditions can be managed appropriately if the patient is cooperative and the healthcare provider is competent and well trained. Unfortunately, almost 600 pregnant women die in the U.S. each year from complications and the most common complication is significant blood loss after birth or postpartum hemorrhage (PPH).
PPH occurs when there is a blood loss of 500 cc or greater for a vaginal delivery and 1,000 cc after a cesarean section (C-section). Or, if you were admitted with a hemoglobin of 12 and it drops by ten points to 11, there should be a high index of suspicion for PPH as well. Therefore, if you feel lightheaded or dizzy, have palpitations or an increased heart rate after delivering a baby, inform the hospital staff immediately.
The most common cause of PPH is uterine atony or lack of contractions after the baby is delivered. Any pregnant condition that stretches the uterus significantly — such as having twins or a higher gestation, excess amniotic fluid (aka polyhydramnios), a prolonged induction of labor (greater than 24 hours) — increases the risk of PPH. Retained products of conception, such as the placenta, also places the patient at risk for developing PPH.
Other risk factors for PPH include:
- Women with a known placenta previa
- African-American women
- Hypertension or preeclampsia
- Mothers with infants weighing greater than 8.8 pounds (or 4,000 grams)
- Mothers with greater than seven children
- Women with a history of hemophilia
If you have any of the risk factors listed above, please be proactive and discuss the possibility of a PPH with your healthcare provider. Read more »
*This blog post was originally published at Dr. Linda Burke-Galloway*
March 3rd, 2011 by RyanDuBosar in Health Policy, Research
No Comments »

 High rates of inappropriate antibiotic use continued despite a 15-year campaign by the Centers for Disease Control and Prevention (CDC) aimed at Michigan physicians and consumers on the dangers of antibiotic overuse.
High rates of inappropriate antibiotic use continued despite a 15-year campaign by the Centers for Disease Control and Prevention (CDC) aimed at Michigan physicians and consumers on the dangers of antibiotic overuse.
The Center for Healthcare Research & Transformation (CHRT) released an issue brief detailing overall antibiotic prescribing for adult Blue Cross Blue Shield of Michigan (BCBSM) members. (The project is a non-profit partnership between the University of Michigan and BCBSM.)
While antibiotic prescribing in adults decreased 9.3 percent from 2007 to 2009, it increased 4.5 percent for children during the same time period. The studies found significant differences in prescribing patterns between rural southeast Michigan and the rest of the state, particularly for children. Children in rural southeastern Michigan were prescribed an average of .93 antibiotics per year, while elsewhere children were prescribed an average of 1.0 per year.
“The continuing high rate of antibiotic use for viral infections in children and adults — particularly outside of southeast Michigan — is of great concern, as is the increase in the use of broad spectrum antibiotics in children,” said Marianne Udow-Phillips, CHRT’s director. “Using antibiotics when they are unnecessary — or treating simple infections with drugs that should be reserved for the most serious infections — are practices that contribute to antibiotic resistance, making future infections harder to treat.”
Nearly half (49.1 percent) of antibiotic prescriptions in the study population were for broad spectrum antibiotics in 2009, compared to the national rate of 47 percent. Between 2007 and 2009, prescriptions for what the National Committee for Quality Assurance calls “antibiotics of concern” declined slightly in adults, decreasing 0.4 percent during that time period. In the same time period, antibiotics of concern prescribed to children increased 3.4 percent, from 44.9 percent to 46.4 percent.
One possible explanation for the rising rate in children is a rise in resistant pathogens in ear infections, according to the study brief. Other possible reasons are that kids get different infections than adults, and that some drugs that are used in adults are not used for pediatric patients. Read more »
*This blog post was originally published at ACP Internist*
March 3rd, 2011 by David H. Gorski, M.D., Ph.D. in Opinion, Quackery Exposed, Research
No Comments »

Last Friday, Mark Crislip posted an excellent deconstruction of a very disappointing article that appeared in the most recent issue of Skeptical Inquirer (SI), the flagship publication of the Committee for Skeptical Inquiry (CSI). I say “disappointing,” because I was disappointed to see SI publish such a biased, poorly thought out article, apparently for the sake of controversy. I’m a subscriber myself, and in general enjoy reading the magazine, although of late I must admit that I don’t always read each issue cover to cover the way I used to do. Between work, grant writing, blogging, and other activities, my outside reading, even of publications I like, has declined. Perhaps SI will soon find itself off my reading list.
Be that as it may, I couldn’t miss the article that so irritated Mark, because it irritated me as well. There it was, emblazoned prominently on the cover of the March/April 2011 issue: “Seven Deadly Medical Hypotheses.” I flipped through the issue to the article to find out that this little gem was written by someone named Michael Spector, M.D. A tinge of familiarity going through my brain, I tried to think where I had heard that name before.
And then I remembered.
Dr. Spector, it turns out, first got on my nerves about a year ago, when he wrote an article for the January/February 2010 issue of SI entitled “The War on Cancer: A Progress Report for Skeptics.” I remember at that time being irritated by the article and wanting to pen a discussion of the points in that article but don’t recall why I never did. It was probably a combination of the fact that SI doesn’t publish its articles online until some months have passed and perhaps my laziness about having to manually transcribe with my own little typing fingers any passages of text that I wanted to cite. By the time the article was available online, I forgot about it and never came back to it — until now. I should therefore, right here, right now, publicly thank Mark (and, of course, Dr. Spector) for providing me the opportunity to revisit that article in the context of piling on, so to speak, Dr. Spector’s most recent article. After all, Deadly Hypothesis Seven (as Dr. Spector so cheesily put it) is:
From a cancer patient population and public health perspective, cancer chemotherapy (chemo) has been a major medical advance.
Dr. Spector then takes this opportunity to cite copiously from his 2010 article, sprinkling “(Spector, 2010)” throughout the text like powdered sugar on a cupcake. There’s the opening I needed to justify revisiting an article that’s more than a year old! And what fantastic timing, too, hot on the heals of my post from a couple of weeks ago entitled “Why Haven’t We Cured Cancer Yet?” Read more »
*This blog post was originally published at Science-Based Medicine*
March 2nd, 2011 by Jessie Gruman, Ph.D. in Better Health Network, Opinion
1 Comment »

 The other day I came across this photo of a couple clasping each other in a dramatic tango on the cover of an old medical journal — a special issue from 1999 that was focused entirely on doctor-patient partnership. The tone and subjects of the articles, letters and editorials were identical to those written today on the topic: “It’s time for the paternalism of the relationship between doctors and patients to be transformed into a partnership;” “There are benefits to this change and dangers to maintaining the status quo;” “Some doctors and patients resist the change and some embrace it: Why?”
The other day I came across this photo of a couple clasping each other in a dramatic tango on the cover of an old medical journal — a special issue from 1999 that was focused entirely on doctor-patient partnership. The tone and subjects of the articles, letters and editorials were identical to those written today on the topic: “It’s time for the paternalism of the relationship between doctors and patients to be transformed into a partnership;” “There are benefits to this change and dangers to maintaining the status quo;” “Some doctors and patients resist the change and some embrace it: Why?”
Two questions struck me as I impatiently scanned the articles from 12 years ago: First, why are these articles about doctor-patient partnership still so relevant? And second, why did the editor choose this cover image?
I’ve been mulling over these questions for a couple days, and I think an answer to the second question sheds light on the first. Here are some thoughts about the relationship between patients and doctors (and nurse practitioners and other clinicians) evoked by that image of the two elegant people dancing together:
It takes two to tango. Ever seen one guy doing the tango? Nope. Whatever he’s doing out there on the dance floor, that’s not tango. Without both dancers, there is no tango. The reason my doctor and I come together is our shared purpose of curing my illness or easing my pain. We bring different skills, perspectives and needs to this interaction. When in a partnership, I describe my symptoms and recount my history. I talk about my values and priorities. I say what I am able and willing to do for myself and what I am not. My doctor has knowledge about my disease and experience treating it in people like me; she explains risks and tradeoffs of different approaches and tailors her use of drugs, devices, and procedures to meet my needs and my preferences. Both of us recognize that without the active commitment of the other we can’t reach our shared goal: To help me live as well as I can for as long as I can.
Each dancer adjusts to his or her partner. In tango, each partner has different moves; the lead shifts subtly and constantly between them throughout the dance. In a partnership, when I am really ill, I delegate more decisions to my physicians; when I am well we freely go back and forth, discussing treatment options and making plans. Read more »
*This blog post was originally published at CFAH PPF Blog*


















