January 22nd, 2011 by GarySchwitzer in Health Policy, Opinion
No Comments »

In a recent issue of the British Medical Journal (BMJ), journalist Ray Moynihan wrote: “Beware the fortune tellers peddling genetic tests.” (Subscription required for full access.) Excerpts:
“For anyone concerned about the creeping medicalisation of life, the marketplace for genetic testing is surely one of the latest frontiers, where apparently harmless technology can help mutate healthy people into fearful patients, their personhood redefined by multiple genetic predispositions for disease and early death.
…
Again a tool that’s proved useful in the laboratory has escaped like a virus into the marketplace, incubated by entrepreneurs, lazy reporters, and the power of our collective dreams of technological salvation, this time in the form of personalised medicine to treat us according to our individual genetic profiles.
…
Evaluating genetic tests is a complex business, requiring assessment of how well the test measures what it claims to measure, how well the genetic variation predicts actual disease, how useful the results are in terms of treatment, and what the social and ethical issues might be. Clearly there’s potential for exaggerating the value of a genetic test, which is one reason Germany has imposed severe restrictions on direct-to-consumer testing. In the United States they’re talking of a new test registry on a government website, raising immediate concerns that it could lend legitimacy to unproved and potentially harmful products. Read more »
*This blog post was originally published at Gary Schwitzer's HealthNewsReview Blog*
January 22nd, 2011 by Bryan Vartabedian, M.D. in Health Policy, True Stories
1 Comment »

So I’m in the exam room recently with a new patient. After some initial dialog with the child and family, I launched into the business of problem solving. Ten minutes into my history the mother politely asks: “I’m sorry, and you are?…”
I hadn’t introduced myself. I had left my ID badge at my workstation, and by order of some innocent distraction with the child or family, I hadn’t identified myself immediately on entering the room. This is rare.
Sometimes I assume people will know who I am. But I don’t wear a white coat and my stethoscope is concealed. I wear clothes only good enough to sustain the barrage of regurgitation, urine, full-frontal coughs, and sloppy hugs that mark a successful clinic day. A colleague once told me I dress like an algebra teacher. I haven’t quite processed that one, but suffice it to say it’s easy to fall into a mistaken identity.
So I apologized and made a proper introduction. What’s remarkable is how far I went without the mother having any idea about my identity. I can imagine that it took a certain amount of wherewithal to interrupt the person she suspected was the doctor to ask such a basic question. Read more »
*This blog post was originally published at 33 Charts*
January 22nd, 2011 by Toni Brayer, M.D. in Health Tips, Research
2 Comments »

 Haven’t we all learned that breakfast should be our biggest meal? “Start the day with ‘fuel’ and you can burn it off as the day goes on.” “Eat a big breakfast and you’ll eat fewer calories all day long.”
Haven’t we all learned that breakfast should be our biggest meal? “Start the day with ‘fuel’ and you can burn it off as the day goes on.” “Eat a big breakfast and you’ll eat fewer calories all day long.”
This advice is probably not true, and in fact a new study published in the January 17th issue Nutrition Journal shows that people ate the same at lunch and dinner regardless of what they had at breakfast. If a person ate 1,000 calories at breakfast (which is easy to do with bacon, eggs, toast, hashbrowns, and juice), he or she had a total increase in calories eaten throughout the day by 1,000 calories.
This doesn’t mean we should be skipping breakfast. The problem may be what we historically think of as an “American” breakfast. It might have worked for the farmer in the past or the laborer hauling lumber, but it’s just too many calories for our current level of activity. Read more »
*This blog post was originally published at EverythingHealth*
January 22nd, 2011 by admin in Opinion, True Stories
1 Comment »
 This is a guest post from Dr. Steven Reznick.
This is a guest post from Dr. Steven Reznick.
**********
Patient Advocacy: It’s Worth The Effort
I have a 61-year-old patient who has been seen in my practice for over thirty years. When she first started developing strange aches and pains as well as abdominal symptoms, her evaluation turned up nothing. At that point she was very active: Playing ball with her two growing sons and dancing the nights away wearing out dance partner after dance partner at community social functions.
When I could not determine the cause of her ills, I asked for help at reputable places including the University of Miami rheumatology division and gastroenterology division. Like so many illnesses, the disease remained a mystery until it was ready to show itself and until technology and progress developed diagnostic tools to allow us to see what is actually there. With the help of a brilliant local gastroenterologist and rheumatologist, and after trips to Johns Hopkins Medical Center and the Mayo Clinic, collagenous colitis and sarcoidosis were documented. In the interim, local medical doctors and her friends branded this poor woman as “another neurotic spouse of a doctor who liked narcotics.”
She developed a peripheral neuropathy, which meant her feet and legs hurt all the time with burning/shooting discomfort exacerbated by walking. She went from dancing the Lindy to hobbling with the assistance of her husband, and a cane from the bedroom to her kitchen. She would then have to sit down, massage her legs, and put on thick-cushioned sweat socks to tolerate the foot and leg discomfort. Read more »
January 21st, 2011 by DavedeBronkart in Health Tips, Opinion
No Comments »

There are several stages in becoming an empowered, engaged, activated patient — a capable, responsible partner in getting good care for yourself, your family, whoever you’re caring for. One ingredient is to know what to expect, so you can tell when things seem right and when they don’t.
Researching a project today, I came across an article* published in 2006: “Key Learning from the Dana-Farber Cancer Institute’s 10-Year Patient Safety Journey.” This table shows the attitude you’ll find in an organization that has realized the challenges of medicine and is dealing with them realistically:
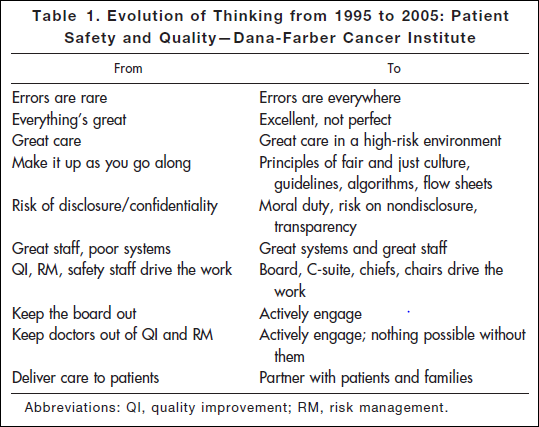
“Errors are everywhere.” “Great care in a high-risk environment.” What kind of attitude is that? It’s accurate.
This work began after the death of Boston Globe health columnist Betsy Lehman. Long-time Bostonians will recall that she was killed in 1994 by an accidental overdose of chemo at Dana-Farber. It shocked us to realize that a savvy patient like her, in one of the best places in the world, could be killed by such an accident. But she was.
Five years later the Institute of Medicine’s report “To Err is Human” documented that such errors are in fact common — 44,000 to 98,000 a year. It hasn’t gotten better: Last November the U.S. Inspector General released new findings that 15,000 Medicare patients are killed in U.S. hospitals every month. That’s one every three minutes. Read more »
*This blog post was originally published at e-Patients.net*





 This is a guest post from Dr. Steven Reznick.
This is a guest post from Dr. Steven Reznick.









