December 19th, 2010 by StevenWilkinsMPH in Better Health Network, Health Tips, Opinion, Research, True Stories
No Comments »

It seem like everyone these days is focused on changing some aspect of patient health behavior. You know — getting patients to get a mammogram or PSA test, exercise more, take medications as prescribed, or simply becoming more engaged in their healthcare. If only we could change unhealthy patient health behaviors, the world would be a better place.
I agree with the sentiment, but I think that patients and their health behavior often get a “bad rap” from healthcare professionals. I would even go so far as to say that much (not all) of what we attribute to poor patient behavior is more correctly attributable to ineffective doctor communications with patients.
In my last post I talked about the link between strong physician advocacy, e.g., I recommend, and desirable health outcomes, i.e., patients getting more preventive screening.
Here’s what I mean. Mammography studies have consistently shown that screening mammograms rates would be much high if more physicians “strongly recommended” that women get screened, e.g., “I recommend” you get a mammogram. In studies where physicians advocated for screening, mammography screening rates were always higher compared to physicians that did not advocate for them. The same phenomenon can be found in studies dealing with exercise, weight loss, colorectal cancer screening, HVP immunization, and patient participation in clinical trials. Read more »
*This blog post was originally published at Mind The Gap*
December 18th, 2010 by KerriSparling in Better Health Network
1 Comment »

 I loved diabetes camp. Actually, that should be in present tense because I continue to love diabetes camp, even though I’m not a camper anymore. Attending Clara Barton Camp for those five summers changed the way I looked at life with diabetes, and my health has always been better for it.
I loved diabetes camp. Actually, that should be in present tense because I continue to love diabetes camp, even though I’m not a camper anymore. Attending Clara Barton Camp for those five summers changed the way I looked at life with diabetes, and my health has always been better for it.
But I’ve talked about camp before. I’d love to play a role in sending other kids to diabetes camp. And thankfully, we as a community now have that chance.
The Diabetes Education and Camping Association (DECA) is in the running to win one of the Pepsi Refresh Project grants. If they earn one, they’ll use their winnings to send kids to diabetes camps and will also arm them with digital filmmaking skills so that the campers can chronicle their experiences with type 1 diabetes. As a diabetes camp alum, a patient advocate, and the wife of a filmmaker, I think this is a fantastic idea. Read more »
*This blog post was originally published at Six Until Me.*
December 18th, 2010 by EvanFalchukJD in Better Health Network, Health Policy, Opinion
No Comments »

Here are 11 things that are absolutely going to happen* in 2011 (they’re in no particular order….or are they?):
1. There will be no big compromise between President Obama and the Republicans on healthcare reform. Why? Because the law is such a massive collection of, well, stuff, that it is pretty much impossible to find pieces of it that you could cut a deal on, even if you wanted to. And no, the federal district court decision on the individual mandate doesn’t change my mind…and in fact may breathe new life into other parts of the law). State governments, insurance companies, and private businesses have made all kinds of important and hard to reverse choices based on the law as is. There’s not much of an appetite outside of people trying to score political points for making big changes.
2. No major employer will drop their health benefits. No major employer is going to outsource their healthcare benefits to the government any time soon. Employers — particularly the big self-insured employers that pay for healthcare costs as a bottom-line expense — see their benefits as an integral part of their business and competitive strategies. As Congress looks at this issue more closely, they will learn this.
3. Time that doctors spend with patients will be less in 2011 than earlier years. It’s a long-term trend, and the factors that create this problem aren’t getting better. The latest government data show that the average doctor visit features face to face time with the patient of 15 minutes or less. With an aging population, increasing numbers of people getting health insurance, and no influx of new doctors, this problem will keep getting worse. Read more »
*This blog post was originally published at See First Blog*
December 18th, 2010 by John Di Saia, M.D. in News
3 Comments »
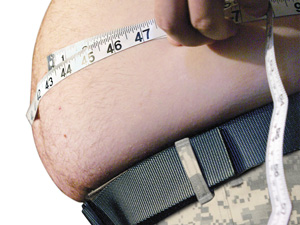 The Orange County Register blog posted on military plastic surgery and mentioned liposuction:
The Orange County Register blog posted on military plastic surgery and mentioned liposuction:
Army Times reports that soldiers are turning to liposuction to remove fat if extreme dieting, laxatives and other methods fail to get them under the Army’s weight limit for their height, age and gender.
“Liposuction saved my career. Laxatives and starvation before an [Army Physical Fitness Test] sustains my career,” a soldier told the periodical. “Soldiers are using liposuction, laxatives and starvation to meet height and weight standards. I did, do and still do.”
I am well aware of the military patient looking to stay within military parameters to stay in the service as my San Clemente office is quite close to Camp Pendleton, and I give military discounts. I have seen several of these patients in my decade in San Clemente. Surgery for wives still outnumbers surgery for soldiers, though.
As some of these clients have explained, the Marine administration requires active duty soldiers to have certain measurements at a certain weight. Those who do not fall within these expected norms are first warned and then penalized. Liposuction has worked at times to keep some of these soldiers in the service.
– John Di Saia, M.D.
*This blog post was originally published at Truth in Cosmetic Surgery*
December 18th, 2010 by Elaine Schattner, M.D. in Better Health Network, Opinion
No Comments »

A perspective in [a recent] NEJM considers the Emerging Importance of Patient Amenities in Patient Care. The trend is that more hospitals lure patients with hotel-like amenities: Room service, magnificent views, massage therapy, family rooms and more. These services sound great, and by some measures can serve an institution’s bottom line more effectively than spending funds on top-notch specialists or state-of-the-art equipment.
Thinking back on the last time I visited someone at Sloan Kettering’s inpatient unit, and I meandered into the bright lounge on the 15th floor, stocked with books, games, videos and other signs of life, I thought how good it is for patients and their families to have a non-clinical area like this. The “extra” facility is privately-funded, although it does take up a relatively small bit of valuable New York City hospital space (what might otherwise be a research lab or a group of nice offices for physicians or, dare I say, social workers) seems wonderful.
If real healthcare isn’t an even-sum expense problem, I see no issue with this kind of hospital accoutrement. As for room service and ordering oatmeal for breakfast instead of institutional pancakes with a side of thawing orange “juice,” chicken salad sandwiches, fresh salads or broiled salmon instead of receiving glop on a tray, that’s potentially less wasteful and, depending on what you choose, healthier. As for yoga and meditation sessions, there’s rarely harm and, maybe occasionally, good (i.e. value).
But what if those resources draw funds away from necessary medicines, better software for safer CT scans and pharmacies, and hiring more doctors, nurses or aides? (I’ve never been in a hospital where the nurses weren’t short-staffed.) Read more »
*This blog post was originally published at Medical Lessons*




 I loved diabetes camp. Actually, that should be in present tense because I continue to love diabetes camp, even though I’m not a camper anymore. Attending
I loved diabetes camp. Actually, that should be in present tense because I continue to love diabetes camp, even though I’m not a camper anymore. Attending