November 9th, 2010 by GarySchwitzer in Better Health Network, Health Policy, News, Opinion
No Comments »

Take medical uncertainty. Add financial incentive to treat. Voila! Increased utilization. Now take away financial incentive to treat. Guess what you get?
MedPageToday explains, in the case of hormone therapy for prostate cancer:
Medicare accomplished what clinical guidelines and evidence-based medicine couldn’t: it reduced unnecessary use of androgen deprivation therapy (ADT) in prostate cancer.
Inappropriate use decreased by almost 30% from 2003 to 2005, following enactment of the Medicare Modernization Act, which lowered physician reimbursement for ADT. Appropriate use of ADT did not change during the same time period, according to an article in the Nov. 4 issue of the New England Journal of Medicine.
“Our findings suggest that reductions in reimbursement may influence the delivery of care in a potentially beneficial way, with even the modest [reimbursement] changes in 2004 associated with a substantial decrease in the use of inappropriate therapy,” Vahakn B. Shahinian, MD, of the University of Michigan in Ann Arbor, and co-authors wrote in conclusion.
“The corollary is that reimbursement policies should be carefully considered to avoid providing incentives for care for which no clear benefit has been established. The extreme profitability of the use of gonadotropin-releasing hormone (GnRH) agonists during the 1990s probably contributed to the rapid growth in the use of ADT for indications that were not evidence-based.”
*This blog post was originally published at Gary Schwitzer's HealthNewsReview Blog*
November 9th, 2010 by Felasfa Wodajo, M.D. in Better Health Network, News, Research
No Comments »

 The explosion of smart phones, originally led by the iPhone 2007, has catalyzed the explosion of mobile medical apps which our readers are surely familiar with. But, along with the proliferation of medical reference apps and interfaces to electronic health records (EHRs), there is a much broader world of mobile medical devices and simpler phone interfaces collectively termed “mHealth,” which is an area of intense interest for governments, industry and care providers.
The explosion of smart phones, originally led by the iPhone 2007, has catalyzed the explosion of mobile medical apps which our readers are surely familiar with. But, along with the proliferation of medical reference apps and interfaces to electronic health records (EHRs), there is a much broader world of mobile medical devices and simpler phone interfaces collectively termed “mHealth,” which is an area of intense interest for governments, industry and care providers.
This year, this interest has been punctuated by nearly half a dozen different mobile health meetings — many that iMedicalApps has attended and participated in. Perhaps, the largest one of all — the mHealth Summit — is now in session in the Washington Convention Center, sponsored in part by the Foundation at National Institutes of Health (FNIH) — an event we are currently attending. This type of sponsorship is an indication of the importance mobile health (or “mHealth”) is now reaching. To further accentuate this, the keynote speaker to launch the event was Dr. Francis Collins, the director of the NIH himself. Read more »
*This blog post was originally published at iMedicalApps*
November 9th, 2010 by KevinMD in Better Health Network, News, Opinion
No Comments »

A social media manager is becoming an imperative position for hospitals.
Medical institutions are waking up to the fact that they need to engage their patients and physicians online. Nowhere is there more fertile growth than in the various social media platforms that are prevalent today — like Facebook, Twitter, and YouTube.
American Medical News recently profiled the phenomenon, highlighting the position of social media manager, which some institutions pay between $60,000 and $80,000 per year.
As it stands, many hospitals are tiptoeing into the world of social networks, guided by the able hands of select online mavens like Mayo Clinic’s Lee Aase and Swedish Medical Center’s Dana Lewis. However, convincing executives of the return on investment remains a challenge. Read more »
*This blog post was originally published at KevinMD.com*
November 9th, 2010 by Edwin Leap, M.D. in Better Health Network, Opinion, True Stories
1 Comment »

When we physicians don’t get our way, or don’t get the response we desire, we can be intimidating. I have seen this play out many different ways. I have been treated rudely by other physicians. I was once threatened by a very prominent one, who told me (in response to the fact that I dared question his tone): “Be careful son, you’re digging yourself a deep hole.” I don’t know what kind of hole, or where it would have taken me, but he was certain I was digging it. Oddly enough, I rather like digging holes. (Very zen.)
Physicians yell at one another, or curse. Physicians stomp around and slam down charts. I don’t like it at all. I think it suggests immaturity. I always tell students and residents that in the ER, especially, the physician is “Captain of the Ship,” and the Captain must never lose his or her cool.
But physicians, sadly, do the same to non-physicians. Nurses, in particular, earn their ire as they scream, curse, stomp and engage in all sorts of negative behaviors. It also happens to paramedics, unit secretaries, dietary workers, therapists, administrators and all manner of persons. Read more »
*This blog post was originally published at edwinleap.com*
November 8th, 2010 by Bryan Vartabedian, M.D. in Better Health Network, Health Policy, News, Opinion
2 Comments »

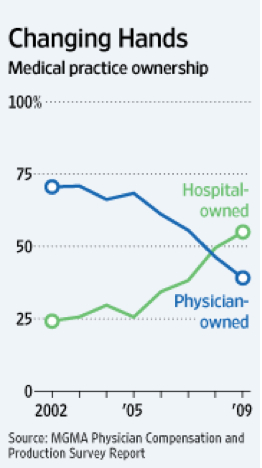 I didn’t need the Wall Street Journal to tell that the days of “private practice” are numbered. According to recent numbers, fewer and fewer medical practices are under the ownership of physicians. Even in my corner of the economically secure State of Texas, small practices are folding faster than beach chairs at high tide.
I didn’t need the Wall Street Journal to tell that the days of “private practice” are numbered. According to recent numbers, fewer and fewer medical practices are under the ownership of physicians. Even in my corner of the economically secure State of Texas, small practices are folding faster than beach chairs at high tide.
I was driven out of private practice in 2004 by rising malpractice premiums and plummeting reimbursement. In Texas at the time the trial attorneys ran the place and medmal insurance carriers simply couldn’t keep up with the greed.
Medical practices are just too expensive to run and the services that physicians provide are dangerously undervalued. You do the math. Sure it’s a complicated issue. But the end result is institutionally-employed doctors with institutional pay and the risk of institutional service. Read more »
*This blog post was originally published at 33 Charts*




 The explosion of smart phones, originally led by the iPhone 2007, has catalyzed the explosion of
The explosion of smart phones, originally led by the iPhone 2007, has catalyzed the explosion of 











