November 2nd, 2010 by Jennifer Shine Dyer, M.D. in Better Health Network, Health Policy, Opinion, Quackery Exposed, Research
No Comments »
I recently read an article by Heather MacDonald entitled “Public Health Quackery” that has not left my thoughts since. The truth in regards to what determines health is being argued in the article.
At the heart of the article, MacDonald seeks to contrast the traditional science approach with the miasmatician approach to the fundamental question of the role of individual behaviors vs. socioeconomics on the determinants of health. MacDonald summarizes the miasmaticians’ beliefs of health determinants as being exclusively influenced by socioeconomics thereby dismissing any and all influences on health by individual behaviors.
Her primary argument in favor of the traditional science belief in individual behaviors as determinants of health is as follows: Traditional science bases assumptions of truth on data that is valid by scientific standards vs. miasmaticians’ assumptions of truth from biased, “flimsy” data. In other words, “quacky” ideas come from “quacky” data thus are not likely to be true. Read more »
November 1st, 2010 by Dr. Val Jones in Health Tips, News
No Comments »
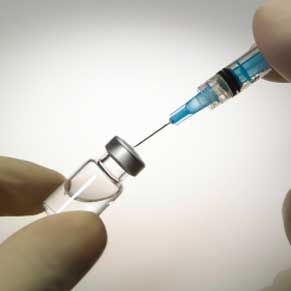 Vaccines have saved more lives than any other medical intervention in history. They are incredibly safe and effective and are well-tolerated by most people. In the US, the Centers For Disease Control and Prevention (CDC) carefully reviews all reports of adverse reactions that could be associated with vaccines. Over decades of review, they have found that the rate of potential severe reactions is so low that they cannot even calculate a risk.
Vaccines have saved more lives than any other medical intervention in history. They are incredibly safe and effective and are well-tolerated by most people. In the US, the Centers For Disease Control and Prevention (CDC) carefully reviews all reports of adverse reactions that could be associated with vaccines. Over decades of review, they have found that the rate of potential severe reactions is so low that they cannot even calculate a risk.
There are many vaccines available for babies, children, and adults. Please check these vaccine schedules to make sure that you and your family are fully protected from vaccine-preventable diseases. (Or you can ask your doctor/nurse to review your vaccine needs with you in person.)
Vaccines for ages 0-6 click here.
Vaccines for ages 7-18 click here.
Vaccines for adults click here.
In case you have any doubts about the value of protecting yourself from disease, here are my top 10 reasons to get vaccinated: Read more »
November 1st, 2010 by EvanFalchukJD in Better Health Network, Health Policy, News, Opinion
1 Comment »

You want to see a doctor? You’re going to have to wait. And I don’t mean like an hour in the office. I mean like 53 days.
It’s not some doomsday story from the future. It’s happening today here in Massachusetts. Massachusetts — the state whose 2006 law was the model for the federal healthcare reform law. Massachusetts — home to some of the world’s best medical centers and doctors. And, as the Boston Globe’s “White Coat Notes” blog reports, Massachusetts — home to doctor shortages and long waits to see a doctor:
When primary care patients do secure an appointment for a non-urgent matter, they have to wait to get in the door, the survey found. The average delay is 29 days to see a family medicine doctor, down from 44 days last year, and 53 days to see an internist, up from 44 days last year.
The report said shortages also exist in dermatology, emergency medicine, general surgery, neurology, orthopedics, psychiatry, urology, and vascular surgery.
But what about costs? If you make sure everyone’s covered, you’ve got the foundation for real cost control, right? Unfortunately, no. Healthcare costs have been booming in Massachusetts:
Costs are rising relentlessly for both families and for the state government. The median annual premium for family plans jumped 10% from 2007 to 2009 to $14,300 — again, that’s a substantial rise on top of an already enormous number. For small businesses, the increase was 12%. In 2006, the state spent around $1 billion on Medicaid, subsidies for medium-to-lower earners, and other health-care programs. Today, the figure is $1.75 billion. The federal government absorbed half of the increase.
So what are the lessons for the future of American healthcare? Read more »
*This blog post was originally published at See First Blog*
November 1st, 2010 by DrRich in Better Health Network, Health Policy, Opinion
No Comments »

In prior posts, DrRich introduced his readers to Ezekiel Emanuel, M.D., Ph.D., brother of Rahm, eminent medical ethicist, and one of the White House’s chief advisers on healthcare policy. Dr. Emanuel was one of the authors of that recent paper in the Annals of Internal Medicine which admonished American physicians that resistance is futile. He has also famously called upon American physicians to abandon the obsolete medical ethics expressed in the Hippocratic Oath.
The reason the ideas (and pronouncements) of Dr. Emanuel are important is that he presumably will be a major “decider” in determining who will serve on the GOD panels, and how those panels will operate to advance his (and Mr. Obama’s) program of healthcare reform.
So, before we leave Dr. Emanuel to his important duties, let us take one more pass at the views he has expressed, regarding the direction of American healthcare, which we can expect to see manifested in government guidelines and policies in the coming years. In particular, and especially relevant to the subject of this blog, let us view how Dr. Emanuel would direct the rationing of our healthcare. Read more »
*This blog post was originally published at The Covert Rationing Blog*
October 31st, 2010 by DavidHarlow in Better Health Network, Health Policy, News, Opinion
No Comments »

I [recently] attended the Connected Health Symposium in Boston. I enjoyed many of the sessions (sometimes wished I could have attended two simultaneously, though the livetweeting — #chs10 — helped on that front), and as usual enjoyed the hallway and exhibit floor conversations too. As is often the case at conferences these days, I had the opportunity to meet several online connections in real life for the first time.
(I will not attempt to give a comprehensive report of the symposium here. Please see the livetweeting archive and other reports to get a sense of the rest of the event.)
This year’s exhibit floor included a diverse mix of distance health tools. Most striking from my perspective was the fact that most of these tools do one of two things: Enable patient-clinician videoconferencing, or upload data from in-home monitoring devices. The best of the second category also trigger alerts resulting in emails or PHR/EHR alerts to clinicians if vital signs are out of whack, or phone calls to consumers or their caregivers if, for example, meds aren’t taken on time (one company had a pill bottle with a transmitter in the cap that signals when it’s opened; another had a Pyxis-like auto-dispenser, that looked like you’d need an engineer — or a teenager — to program it). One tool — Intel’s — seemed to combine most of these functions, and more, into one platform, but it’s barely in beta, with only about 1,000 units out in the real world.
The speakers this year seemed to return again and again to several major themes: (1) Is any particular connected health solution scalable? (2) Who will pay for connected health, or mobile health (mHealth)? and (3) Does it work? Read more »
*This blog post was originally published at HealthBlawg :: David Harlow's Health Care Law Blog*














