July 8th, 2009 by KerriSparling in Better Health Network, Patient Interviews, True Stories
No Comments »

After a hectic week with the conference in Philly and then Chris’s great news, I need to spend some time today catching up on everything. Thankfully, Jessica Phillips has offered to guest post today, writing about marking 500 days with type 1 diabetes. She’s come a long way, and I’m proud to host her words here on SUM.
Heeeeeeere’s Jessica!
* * *
As I was injecting myself with insulin on a lunch break at work, a co-worker walked by and exclaimed, “I could never do that! EW! I hate needles!” Less than two years ago I might have agreed. I never had a strong phobia of needles, but that is not to say that I particularly liked them either. I was known in my childhood to run out of doctor’s offices into the parking lot at the first mention of “shot”. Now when I hear such a strong and callous remark to my now normal routine of insulin injections, I struggle with trying not to angrily reply, “Well you would have to give yourself shots if you had to in order to live!” or, “How do you think I feel? You think I want to do this?” I’ve learned as of late to simply smile and say, “It’s not easy.”
never do that! EW! I hate needles!” Less than two years ago I might have agreed. I never had a strong phobia of needles, but that is not to say that I particularly liked them either. I was known in my childhood to run out of doctor’s offices into the parking lot at the first mention of “shot”. Now when I hear such a strong and callous remark to my now normal routine of insulin injections, I struggle with trying not to angrily reply, “Well you would have to give yourself shots if you had to in order to live!” or, “How do you think I feel? You think I want to do this?” I’ve learned as of late to simply smile and say, “It’s not easy.”
Reactions like this are commonplace for those of you who have experienced Type One Diabetes for many years, and even some for the majority of your life. For me, June 9th, 2009 marked my 500th day with type 1 diabetes. I was diagnosed in my hometown of San Diego, California on January 25th, 2008 at 26 years-old. For a couple months prior to diagnosis I had been experiencing the typical signs of hyperglycemia and a failing pancreas as I was constantly dehydrated, urinating, and tired. Being a college student and in a constant state of stress, I quickly attributed the majority of my symptoms, from dizziness to infections, to be solely related to my immune system’s battle with my constant stress. After many weeks of procrastinating, I finally urged my doctor to order a blood test. I went in to the lab on January 23rd and was called by my doctor 24 hours later while I was driving to school. The tone in her voice immediately caught my attention and set me in a state of alarm. She informed me that my blood sugar the day before was above 300 mg/dL and I was to avoid sugar and be referred to an endocrinologist immediately.
Luckily I was able to see an experienced endocrinologist the next day, and he diagnosed me with type 1 within minutes of being seated in the exam room. I was in complete shock, and felt confused, angry, and overwhelmingly sad all at the same time. I felt a struggle between trying to remain alert to the bombardment of information he was feeding me, and trying desperately not to cry. The doctor left the room to retrieve my new meter and insulin pens, and I lost it. Luckily I had some moral support with me, but I have never felt so alone and lost. I kept thinking, “how did this happen?” and, “what did I do wrong?” To have gone many years without having anything major occur medically, not even a broken bone, it was a major shock to hear I had something irreversibly wrong with me. I not only had something wrong, but I could not do anything to change it.
The next few days were extremely challenging to say the least. I was unable to give myself insulin and had to have someone else do it for me for the first couple days. I would sit and look at the needle and could not conceive of how this tiny piece of metal was going to go through my skin. I just kept thinking it was so wrong, and foreign. I also cried. A lot. And I researched online and in books so much that I felt as though I could speak at a lecture on the biology of diabetes. I found the knowledge empowering, and the more I grasped what my body was actually doing, and not doing, I became more confident in my ability to control my state.
Now, 500 days later, this diabetic routine is normal to me. I can hardly even remember a time when diabetes wasn’t on my mind. The memories have faded of when my blood sugar was not a concern, and when I was able to look at food as just food. The last year and a half has been a giant emotional roller coaster, full of ups and downs, but they have changed me. Sometimes I get the look of sympathy from others when I detail my hardships with this disease, anywhere from medical costs to just the simple annoyance of pricking myself all the time, and I have found myself realizing that although I would not choose to have this disease, I consider myself lucky. I am lucky of course to not have something worse, but having gone through this change has made me look at my life through a new and clearer lens. My bottom-line now is a cliché idea, but it is so true … life is short, and you only get one shot, so make it worth it, no matter what.
* * *
Thanks for sharing your story, Jessica. (And for the record, Jessica is the one with the fantastic hair on the right in that photo. Also for the record, I just realized that today is my 8,209th day with diabetes. Holy crap, my pancreas is lazy.)
*This blog post was originally published at Six Until Me.*
June 23rd, 2009 by KerriSparling in Better Health Network, True Stories
No Comments »

I saw my niece over the weekend. She just turned seven. She had a bit of a fever and wasn’t feeling very well, so when I saw her snuggled up on the couch under a blanket, she looked every bit the little kid she is. Poor little peanut, hiding out until she felt better.
I remembered that I was about her age when I was diagnosed.
I found an old school photo from second grade, with me sitting next to my friend Bobby (who I still talk to, which is a very surreal experience, hanging out with someone I’ve known longer than I’ve known insulin injections). I was diagnosed in September, right as second grade started.
I’m in the blue dress, second row from the bottom, third from the left.
Swinging my feet. Not much for sitting still, even in second grade.
Over the last few days, I’ve been reading some emails from the CWD parents as they gear up for the Friends for Life conference in Orlando in a few weeks. These emails are sent out to a whole mailing list of attendees, and somehow I ended up on the list with all the parents. (Or maybe the list just happens to be mostly parents and I just happen to be an adult “kid” with diabetes.) These parents are comparing notes and reaching out to one another, looking forward to other parents who understand what they’re going through every day as they care for their kid with diabetes.
And I wish that my mother had this kind of support when she was dealing with my diagnosis over twenty years ago. My mom had a lackluster team of doctors at the Rhode Island Hospital (where I went for a few months before going to Joslin) and Eleanor (the only other mother of a diabetic kid that we knew of in our town and the woman who just happens to be my local Dexcom rep), leaving her with little to manage the enormous learning curve.
This weekend, I went on a bike ride with my sister-in-law, my father-in-law, and my husband. I had to remember to test beforehand, bring my meter, stash some glucose sources on several people, and monitor as re rode. A lot of thought for maybe an hour long bike ride. And it made me wonder what kind of preparation and worry my mother went through when she sent me out to play for a whole Saturday afternoon. Lot of work on my mom’s part just to keep things normal.
I forget this sometimes, how many people are really involved in keeping me healthy.
I need to call my mom.
(Granted, my diabetes diagnosis hasn’t kept me from doing much at all. And it definitely didn’t keep me from being … um, a bit of a goofball.)
*This blog post was originally published at Six Until Me.*
January 3rd, 2009 by Dr. Val Jones in Patient Interviews
3 Comments »
Thanks to KevinMD for highlighting an interesting discussion about the ethics of disclosing another physician’s error. It reminded me of a case I witnessed many years ago.
A young man had been in a car accident and was transferred to the rehab unit after several orthopedic surgeries and a long inpatient stay. Prior to beginning physical therapy, he was sent for doppler ultrasounds of his deep leg veins to make sure that he didn’t have a thrombus (clot) that might break off and lodge in his lungs during exercise. The ultrasound was actually positive for a large DVT. Unfortunately, the radiology note listed all the large veins that were patent (had no clots) first, and then finished with a notation of (+) DVT in one of the veins. The patient was transferred back upstairs to the rehab unit, the physical therapist glanced at the radiology report (where the first several sentences indicated normal findings) and took the patient to group therapy.
The patient got up out of his wheelchair, stood for a few seconds, and immediately collapsed. His DVT broke off and traveled to his lungs, causing a massive occlusion of his vessels. The crash cart arrived as he coded, the vascular surgery team quickly took him to the OR to crack his chest and try to remove the clot, but he didn’t make it. It was shocking and terrible.
What happened afterwards was memorable. The rehabilitation medicine attending notified the family of the error, explained exactly what happened and apologized with tears. The hospital administration was notified, the physical therapist, radiologist, residents, and attending physicians got together for a meeting in which a new reporting protocol for positive doppler findings was created. To my knowledge, there has not been another case of pulmonary embolism on that rehab unit since.
The family members did not sue. They were deeply grieved, but grateful for the transparency. The dangers of DVTs were indellibly burned into the minds of all physicians and staff working in the rehabilitation unit – and I believe that our lifelong vigilance may save many other patients from a similar fate.
That’s what should be done when mistakes happen.
November 14th, 2008 by Dr. Val Jones in Patient Interviews
3 Comments »
 |
|
Kerri Morrone-Sparling
|
Kerri Morrone-Sparling is a whirlwind of energy. Not only is she the founder of one of the first diabetes blogs on the Internet: SixUntilMe, but she has devoted her career to helping others with diabetes. She works full time at dLife.com, a delightful and practical diabetes website and community. Kerri recently offered me some Halloween survival tips for people with diabetes, and today I had the chance to interview her about her life, her work, and the meaning of World Diabetes Day.
**Listen to the Podcast**
I’ve summarized some of our talking points below for those who don’t wish to listen to the dulcet tones of two very friendly ladies dishing about diabetes.
Dr. Val: Tell me a little bit about your blog.
Kerri: My blog is called SixUntilMe and I started it in May of 2005. I was looking for other people like me who were living with diabetes and since I couldn’t find a community like that I decided to start one myself. As it turns out I wasn’t the only one – there were 2 or 3 other diabetes bloggers out there at the time, and now there are more than 250 of us.
Dr. Val: What does “six until me” mean?
Kerri: My diabetes started when I was six years old – I had a viral illness on my birthday which probably triggered an autoimmune response, causing the disease. My blog is about my diabetes – which started when I was six and is ongoing until now. So I called it “sixuntilme.”
Dr. Val: How are you involved in diabetes advocacy?
Kerri: I work for a diabetes media company, (dLife in Westport, Connecticut) so my entire day is built around reaching out to people with diabetes, trying to make a difference in their life, and connecting them with up-to-date health information. Since I grew up without knowing any other kids who had diabetes, this job is like the holy land. I mean, this whole company was built to help people like me.
Dr. Val: What are some of the worst diabetes myths and what do you have to say about them?
Kerri: First of all, most people don’t know the difference between type 1 and type 2 diabetes, and to make matters worse, they believe that people “give themselves diabetes” by eating too much sugar. So they make it seem like it’s all our fault. Secondly, people often believe that insulin is the cure for diabetes. They don’t realize that a glucose meter, an insulin pump, or a continuous glucose monitor are just technology, not a cure. Sometimes people think there’s no need to donate to diabetes research anymore because these technologies are available. And finally, Halle Berry has promoted a myth that has done a lot of harm to the diabetes community. She claimed that she was able to wean herself off her insulin, and that other type 1 diabetics could do the same if they tried hard enough. Of course, that’s blatantly false.
Dr. Val: What’s your favorite new technology for diabetes management?
Kerri: My continuous glucose monitor (CGM). It doesn’t replace finger stick checks, but it helps you to see the trends in your blood sugar. For example, when you’re about to go to bed and you see that your glucose is 90, the CGM will give you some idea if that’s 90 on its way up, or 90 falling towards hypoglycemia, or 90 holding steady – you can go to bed and not worry about a thing. It’s like swinging on a trapeze only now I have a net.
Dr. Val: How does the machine work?
Kerri: It’s a small device that has a needle in it, and you stick it to a fleshier part of your body. There’s a small wire (introduced through the needle) that continuously samples the sugar level in your interstitial fluid. It’s easy to remove and should be rotated every 3-7 days.
Dr. Val: Is it painful?
Kerri: No, I don’t think so. I use the Dexcom Seven CGM. Occasionally I feel a little prick when I insert it but then I don’t even notice that I’m wearing it. Here’s a photo of me wearing it:
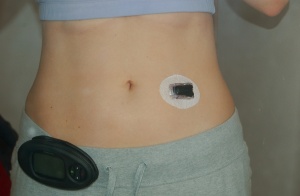

Dr. Val: Tell me about World Diabetes Day.
Kerri: It’s a global awareness campaign that was started in 1991 by the International Diabetes Federation. The United Nations recognized the event for the first time in 2007. It’s a day that directs the world’s attention to diabetes and the epidemic its become and the effort it takes to manage it. On World Diabetes Day bloggers want to spread the word that diabetes is not an invisible disease. It affects lives every day, and it deserves the world’s attention.
Dr. Val: What’s the most important thing for Americans to know about diabetes?
Kerri: They need to know that diabetes is not cured by insulin, and it’s not going away without their help. It’s a very difficult disease to manage. No matter how well you control your sugar levels, the effects of the disease take their toll eventually, and the effects can be devastating. We must not ease up on our research efforts, especially when the numbers of people living with diabetes are growing exponentially.
References
www.diabeticfeed.com
http://the-bad-blog.blogspot.com/
http://www.diabetesdaily.com/johnson/
Kerri writes a column at dLife called Generation D (www.dlife.com/generation_d) and maintains a pretty extensive Flickr account at http://www.flickr.com/photos/sixuntilme/. And lastly, if you’d like to follow Kerri on Twitter, you can find her at www.twitter.com/sixuntilme.
October 29th, 2008 by Dr. Val Jones in Health Tips, Medblogger Shout Outs
No Comments »
 My friend and fellow blogger Kerri Morrone Sparling (at the Six Until Me blog) was diagnosed with type 1 diabetes when she was in second grade. The diagnosis came a few short weeks before Halloween, and back then she didn’t realize the risks of sneaking candy bars behind her mom’s back.
My friend and fellow blogger Kerri Morrone Sparling (at the Six Until Me blog) was diagnosed with type 1 diabetes when she was in second grade. The diagnosis came a few short weeks before Halloween, and back then she didn’t realize the risks of sneaking candy bars behind her mom’s back.
Now that Kerri’s grown up, she has some excellent tips for parents of children with type 1 diabetes (or frankly, for anyone who wants to enjoy Halloween and manage their diabetes). You should check out her video blog on the subject here.
Some tips include:
1. Focus on the costume part of the holiday, not the candy part.
2. Make some “candy” corn with Splenda, Equal or a sugar substitute. Enjoy the salty-sweet treat instead of a Snicker’s bar (for example).
3. Work in a small amount of candy into your diet plan. Eat a half a candy bar during a period of high activity, for example, and the sugar spike will not be so bad.
Please check out Kerri’s post for more tips!
***
And for a good laugh about candy, check out The Onion’s headline here.
 never do that! EW! I hate needles!” Less than two years ago I might have agreed. I never had a strong phobia of needles, but that is not to say that I particularly liked them either. I was known in my childhood to run out of doctor’s offices into the parking lot at the first mention of “shot”. Now when I hear such a strong and callous remark to my now normal routine of insulin injections, I struggle with trying not to angrily reply, “Well you would have to give yourself shots if you had to in order to live!” or, “How do you think I feel? You think I want to do this?” I’ve learned as of late to simply smile and say, “It’s not easy.”
never do that! EW! I hate needles!” Less than two years ago I might have agreed. I never had a strong phobia of needles, but that is not to say that I particularly liked them either. I was known in my childhood to run out of doctor’s offices into the parking lot at the first mention of “shot”. Now when I hear such a strong and callous remark to my now normal routine of insulin injections, I struggle with trying not to angrily reply, “Well you would have to give yourself shots if you had to in order to live!” or, “How do you think I feel? You think I want to do this?” I’ve learned as of late to simply smile and say, “It’s not easy.”














