March 7th, 2011 by Elaine Schattner, M.D. in Health Policy, Opinion
No Comments »

[Recently] a short article in the New York Times, New Kidney Transplant Policy Would Favor Younger Patients, [drew] my attention to a very basic problem in medical ethics: Rationing.
According to the Washington Post coverage, the proposal comes from the United Network for Organ Sharing, a Richmond-based private non-profit group the federal government contracts for allocation of donated organs. From the Times piece:
Under the proposal, patients and kidneys would each be graded, and the healthiest and youngest 20 percent of patients and kidneys would be segregated into a separate pool so that the best kidneys would be given to patients with the longest life expectancies.
This all follows [the recent] front-page business story on the monetary value of life.
I have to admit, I’m glad to see these stories in the media. Any reasoned discussion of policy and reform requires frank talk on healthcare resources which, even in the best of economic times, are limited.
*This blog post was originally published at Medical Lessons*
March 7th, 2011 by RyanDuBosar in Health Policy, News
No Comments »

A federal judge who’d ruled healthcare reform was unconstitutional and that his decision as a federal judge was the equivalent of an injunction has relented. Healthcare reform can continue in the states, pending appellate and Supreme Court review.
“The sooner this issue is finally decided by the Supreme Court, the better off the entire nation will be,” wrote federal judge Roger E. Vinson, who’d decided that the healthcare reform act’s mandate that people buy insurance or face penalties overextended Congress’ powers under the commerce clause of the constitution.
One reason for granting a stay, despite his previous clear intent that healthcare reform cease, includes his statement (on page 18) that:
“Can (or should) I enjoin and halt implementation of the Act in a state where one of its federal courts has held it to be Constitutional? In addition, many of the plaintiff states have publicly represented that they will immediately halt implementation of the Act in light of my declaratory judgment, while at least eight plaintiff states (as identified by the defendants in their motion and reply) have suggested that, in an abundance of caution, they will not stop implementing the Act pending appeal. In addition to these apparent disagreements among the plaintiff states, there is even disagreement within the plaintiff states as to whether the implementation should continue pending appeal. For example, while the plaintiffs (a group that includes the Attorney General of Washington) have requested that I enjoin the defendants from implementing the Act, the Governor of Washington has just filed an amicus brief specifically opposing that request.”
The decision gives the Obama administration seven days to file an appeal against his decision, which a U.S. Department of Justice spokesperson said the administration intends to do. Read more »
*This blog post was originally published at ACP Internist*
March 7th, 2011 by Dr. Val Jones in Health Policy, True Stories
8 Comments »
I first applied for a license to practice medicine in the state of California on July 9, 2008. I was licensed on March 3, 2011 — a whopping 967 days after they first received my application. I haven’t had a problem getting a license in any other state, and I am licensed in six of them. Just to give you a sense of how long it usually takes to process the paperwork for a medical license, Maryland completed mine in under three weeks. So what’s going on in California?
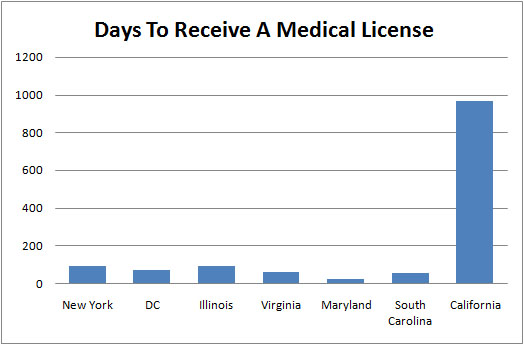
Dr. Val’s Experience
I think the best way to tell this story is with a timeline, and let the facts speak for themselves. I know this represents just one physician’s experience (namely mine), so results may vary:
July 9, 2008 – The Medical Board of California (MBC) received my licensure application and my checks for $493 (for fingerprint and processing fee) and $805 (initial licensing fee), which were cashed soon thereafter.
Sept 29, 2008 – I received a letter in the mail stating that there were four items missing from my application. Two of these four items were already included in the Federation Credentials Verification Service (FCVS) packet they had received from me. The other two items were requests for residency program directors to write letters to support the forms that they had already filled out on my behalf. I immediately requested these letters, and even though I should not have needed to send additional copies of items from the FCVS packet, I did so as well.
December 3, 2008 – I received a letter in the mail from the MBC, stating that there was an additional fee of $25 now required for physicians whose licensure applications were postmarked after December 31, 2008. This obviously didn’t relate to me, but the letter reminded me to follow up with the board to make sure that they had received the four items from the Sept 29th letter. I sent the licensing program administrator an email and left a voice message for follow-up purposes. He gave no response. Read more »
March 6th, 2011 by Edwin Leap, M.D. in Opinion, True Stories
1 Comment »

 Here’s my column in the March issue of Emergency Medicine News.
Here’s my column in the March issue of Emergency Medicine News.
Second Opinion: Be Smarter Than Your Brain
“Everyone is a drug seeker. Why does everyone want to be on disability? I’m so tired of lies. Great, another lousy shift. I wonder who will die tonight? I’m so sick of suffering. I’m so weary of misery and loss. I hope this never happens to my family. I’ll probably get sued. Being sued nearly drove me crazy. This job never gets easier, only harder. I have to find something else to do; I can’t go on this way. I think I’m going crazy. I don’t have any more compassion. People hate me now.”
These are only a few of the wonderful thoughts that float through the minds of emergency physicians these days. Sure, not every physician has them. But I know our specialty, I know our colleagues, I hear from doctors around the country and I see that fear, frustration and anxiety are common themes.
Older physicians fantasize about career changes, and younger ones are often blind-sided by the hard realities of practice outside of their training programs (where their work-hours and staffing do not necessarily reflect the world beyond).
We are crushed by regulations and overwhelmed by holding patients, often put in situations where we are set squarely between the devil and the deep blue sea. “Spend more time with your patients; see them faster. Don’t let the ‘psychiatric hold’ patient escape; why are you using so much staff on psychiatric patients? See chest pain immediately; why didn’t you see the board member’s ankle injury as fast as the chest pain?”
In all of this mess of emergency medicine, we often find ourselves frustrated and bitter. But is it only because of our situations? They are admittedly daunting. But is our unhappiness merely the result of the things imposed on us? Or could it be more complex than that? Lately, I have come to wonder if our thoughts are perhaps worse enemies than even lawsuits, regulations, or satisfaction scores. Read more »
*This blog post was originally published at edwinleap.com*
March 6th, 2011 by Glenn Laffel, M.D., Ph.D. in Opinion, Research
No Comments »

 Among fans who attend live sporting events, drinking alcohol is nearly as commonplace as root-root-rooting for the home team. And while virtually no one has a problem with a fan who pushes back a beer or two during the game, flat-out drunk fans can ruin the experience for those sitting nearby. Worse yet, these people frequently get behind the wheel of a car after the game is over.
Among fans who attend live sporting events, drinking alcohol is nearly as commonplace as root-root-rooting for the home team. And while virtually no one has a problem with a fan who pushes back a beer or two during the game, flat-out drunk fans can ruin the experience for those sitting nearby. Worse yet, these people frequently get behind the wheel of a car after the game is over.
Recently, Darin Erickson and colleagues at the University of Minnesota decided to find out just how many fans go overboard at games, and their findings are worrisome, indeed. Using standard blood alcohol testing on 362 adult volunteers who were leaving 13 professional baseball and three professional football games, the scientists found that 40 percent had measurable levels of alcohol in their blood and a stunning eight percent were legally drunk (as defined by a blood alcohol level of .08 or greater). The highest alcohol level recorded by the scientists was .22.
Erickson’s group also observed that Monday Night Football attendees were more likely than other fans to have been drinking. In addition, fans who were 35 years old or younger were eight times more likely to leave the game drunk, and those who attended tailgating parties before the game were 14 times more likely to leave the game drunk.
The latter finding is consistent with a study from the University of Toledo, in which scientists gave breathalyzer tests to tailgaters at a college football game. The scientists found that an astounding 90 percent of the participants consumed alcohol during tailgate festivities, and among them, the average blood alcohol concentration was 0.06, well on the way to being legally drunk.
Maybe these people should save the money they spent on tickets and go to a bar. Erickson’s study was published in Alcoholism: Clinical & Experimental Research.
*This blog post was originally published at Pizaazz*
















