August 17th, 2015 by Dr. Val Jones in True Stories
26 Comments »
 If you have not read the latest essay and editorial about scandalous physician behavior published in the Annals of Internal Medicine (AIM), you must do so now. They describe horrific racist and sexist remarks made about patients by senior male physicians in front of their young peers. The physicians-in-training are scarred by the experience, partially because the behavior itself was so disgusting, but also because they felt powerless to stop it.
If you have not read the latest essay and editorial about scandalous physician behavior published in the Annals of Internal Medicine (AIM), you must do so now. They describe horrific racist and sexist remarks made about patients by senior male physicians in front of their young peers. The physicians-in-training are scarred by the experience, partially because the behavior itself was so disgusting, but also because they felt powerless to stop it.
It is important for the medical community to come together over the sad reality that there are still some physicians and surgeons out there who are wildly inappropriate in their patient care. In my lifetime I have seen a noticeable decrease in misogyny and behaviors of the sort described in the Annals essay. I have written about racism in the Ob/Gyn arena on my blog previously (note that the perpetrators of those scandalous acts were women – so both genders are guilty). But there is one story that I always believed was too vile to tell. Not on this blog, and probably not anywhere. I will speak out now because the editors at AIM have opened the conversation.
When I was a third-year medical student I was assigned to tag along with an ophthalmology resident serving his first year of residency as an intern in general surgery. We were to cover the ER consult service one night, and our first patient was a young Hispanic girl with abdominal pain. It was suspected that she may have had appendicitis. Part of the physical exam required that we rule out a gynecologic cause of the pain. And so a pelvic exam was planned for this young girl of about 12 or 13. She was frightened and clinging to her grandmother. She had never seen a gynecologist before and had explained through her grandmother that she was a virgin – making a gynecologic cause of her abdominal pain less likely. I offered her some reassurance with my broken Spanish and held her hand as we wheeled her on a stretcher to a private examining room. The resident whispered in my ear, “This is going to be fun.”
The resident was creepy at every stage of the exam. He was clearly relishing the process, slowly instructing the poor girl to position herself correctly on the table. He held her knees apart as she whimpered and cried. He pretended to have difficulty positioning the speculum, inserting and reinserting it an unconscionable number of times. All-in-all it probably took ten minutes for him to get a cervical sample (this usually takes under 60 seconds). He performed the bi-manual portion of the exam in a bizarre, sexualized manner. I was furious and nauseated.
The patient was finally returned to her grandmother and the resident took me aside to ask how I thought he did. The perverted expression on his face was not lost on me. I looked at him with daggers in my eyes, but I knew that if I confronted him head-on it could trigger an investigation and in the end I had no hard evidence to prove that he had done anything wrong. It would wind up being a “he said, she said” scenario. I mustered the courage to say, “I think you were slow.”
For a fleeting moment he was taken aback by my insubordinate criticism and then he said the sentence that still haunts me today, “Well it was her first time.”
Each time I think of this interaction I feel sick to my stomach. I wonder what more I could have done.* I wonder if he is still out there violating his patients, and if anyone has ever confronted him. My only consolation, I suppose, is that he did not go on to become an Ob/Gyn. As an ophthalmologist one would hope that he had fewer opportunities for sexual abuse of patients.
I guess you could say that in my medical training, I witnessed a child rape. I don’t think it gets much worse than that… and I don’t know what to do with this horrific memory. I am forever changed.
It is my hope that these sorts of situations become true “never events” and that we create a protective environment where there are no career consequences for medical students thrust into the unfortunate position of whistle blower. Maybe the courageous AIM editorial is the first step towards redemption and healing.
*Note that I never saw this resident again. Our paths did not cross after the incident, and it was only at the end of the exam that I fully recognized the evil of his intent.
January 5th, 2015 by Dr. Val Jones in Health Tips, Research
No Comments »
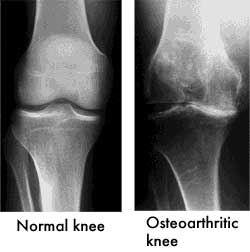 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A new meta-analysis published by the Annals of Internal Medicine may shed some light on this important question. After 3 months of the following treatments, here is how they compared to one another in terms of power to reduce pain, starting with strongest first:
#1. Knee injection with gel (Rx hyaluronic acid)
#2. Knee injection with steroid (Rx corticosteroid)
#3. Diclofenac (Voltaren – Rx oral NSAID)
#4. Ibuprofen (Motrin – OTC oral NSAID)
#5. Naproxen (Alleve – OTC oral NSAID)
#6. Celecoxib (Celebrex – Rx NSAID)
#7. Knee injection with saline solution (placebo injection)
#8. Acetaminophen (Tylenol – OTC Synthetic nonopiate derivative of p-aminophenol)
#9. Oral placebo (Sugar Pill)
I found this rank order list interesting for a few reasons. First of all, acetaminophen and celecoxib appear to be less effective than I had believed. Second, placebos may be demonstrably more effective the more invasive they are (injecting saline into the knee works better than acetaminophen, and significantly better than sugar pills). Third, injection of a cushion gel fluid is surprisingly effective, especially since its mechanism of action has little to do with direct reduction of inflammation (the cornerstone of most arthritis therapies). Perhaps mechanical treatments for pain have been underutilized? And finally, first line therapy with acetaminophen is not clinically superior to placebo.
There are several caveats to this information, of course. First of all, arthritis pain treatments must be customized to the individual and their unique tolerances and risk profiles. Mild pain need not be treated with medicines that carry higher risks (such as joint infection or gastrointestinal bleeding), and advanced arthritis sufferers may benefit from “jumping the line” and starting with stronger medicines. The study is limited in that treatments were only compared over a 3 month trial period, and we cannot be certain that the patient populations were substantially similar as the comparative effectiveness was calculated.
That being said, this study will influence my practice. I will likely lean towards recommending more effective therapies with my future patients, including careful consideration of injections and diclofenac for moderate to severe OA, and ibuprofen/naproxen for mild to moderate OA, while shying away from celecoxib and acetaminophen altogether. And as we already know, glucosamine and chondroitin have been convincingly shown to be no better than placebo, so save your money on those pills. The racket is expected to blossom into a $20 billion dollar industry by 2020 if we don’t curb our appetite for expensive placebos.
In conclusion, the elephant in the room is that weight loss and exercise are still the very best treatments for knee osteoarthritis. Check out the American Academy of Orthopedic Surgery’s recent list of evidence-based recommendations for the treatment of knee arthritis for more information about the full spectrum of treatment options.
November 17th, 2014 by Dr. Val Jones in News, Research
4 Comments »

A Cost Effective Fitness Band
In a new study published in the Annals of Internal Medicine, researchers found that overweight and obese patients who used a popular smart phone app (MyFitnessPal) did not lose significant weight after a 6 month trial period. The randomized controlled trial is the first of its kind to demonstrate that well-liked mobile apps may be ineffective for most users.
Two hundred and twelve racially diverse (73% female) patients treated at two UCLA primary care clinics were enrolled in the study. All indicated that they were interested in losing weight and 79% who completed the study indicated that they were “somewhat” or “completely” satisfied with the app, while 92% reported that they’d recommend it to a friend.
Unfortunately, as pleased as the subjects were with the app, there was no statistically significant difference in weight loss between the intervention and control groups. On average, the MyFitnessPal users lost 0.66 lbs in 6 months.
The authors note:
“Most participants rarely used the app after the first month of the study… Given these results it may not be worth a clinician’s time to prescribe MyFitnessPal to every overweight patient with a smart phone… Our analysis did not show any demographic covariates to be important predictors of app use.”
This study serves as a reminder that “popular” and “effective” do not always go hand-in-hand when it comes to weight loss interventions. While mHealth apps are expected to earn $26 billion by 2017, one is left to wonder if this money will be well spent or if we’ll all be “somewhat to completely satisfied” with the apps without anything medically significant to show for it?
March 31st, 2014 by Dr. Val Jones in Health Policy, Health Tips, Opinion, Research
2 Comments »
 A Canadian study published today in the Annals of Internal Medicine suggests that about one third of new prescriptions (written by primary care physicians) are never filled. Over 15,000 patients were followed from 2006 to 2009. Prescription and patient characteristics were analyzed, though patients were not directly interviewed about their rationale for not filling their prescriptions.
A Canadian study published today in the Annals of Internal Medicine suggests that about one third of new prescriptions (written by primary care physicians) are never filled. Over 15,000 patients were followed from 2006 to 2009. Prescription and patient characteristics were analyzed, though patients were not directly interviewed about their rationale for not filling their prescriptions.
In short, patients were less likely to fill a prescription if the treatment was expensive, but certain types of drug indications had consistently higher non-fill rates:
- Headache (51% not filled)
- Ischemic heart disease (51.3% not filled)
- Thyroid agents (49.4% not filled)
- Depression (36.8% not filled)
Overall, hormonal (especially Synthroid), ENT (especially Flonase), skin, and cardiovascular drugs (especially statins) had the highest non-fill rates.
As far as those prescriptions more likely to be filled, antibiotics (especially for urinary tract infections) ranked number one.
Trends towards prescription compliance were seen among older, healthier patients, and those who were switching medications within a class rather than starting an entirely new drug. Patients who received prescriptions from a doctor that they visited regularly (rather than a new provider) were also more likely to fill their prescriptions.
This study was not designed to elucidate the exact rationale behind prescription non-adherence, but I am willing to speculate about it. In my experience, patients are less likely to fill a prescription if a reasonable over-the-counter alternative is available (think headache or allergy relief). I also suspect that they are less likely to fill a prescription if they believe it won’t help them (skin cream) or isn’t treating a palpable symptom (statin therapy for dyslipidemia). Finally, patients are probably nervous about starting a medicine that could effect their metabolism or cognition (thyroid medication or anti-depressant) without a full explanation of the possible benefits and side effects.
I was surprised to see how compliant patients seem to be with antibiotic agents (at least, filling the initial prescriptions). Given the increasing rates of antibiotic resistance, this reinforces the need to limit prescriptions to those agents truly indicated, and to analyze bacterial sensitivities during the treatment process to optimize medical management.
My take home message from this study is that providers need to do a better job of explaining the reasoning behind new prescriptions (their necessity, consequences of non-compliance, and risk/benefit profiles) and reviewing the overall cost to the patient. If a cheaper, effective alternative is available (whether OTC or generic), we should consider prescribing it. Providers can likely improve medication compliance rates with a little patient education and price consciousness. Extra time should be spent with patients at higher risk for non-compliance due to their personal situation (age, degree of illness, income level) or if a specific drug with lower compliance rates is being introduced (Synthroid, statins, etc.) Regular follow up (especially with the same prescriber) to ensure that prescriptions are filled and taken as directed is also important.
January 6th, 2014 by Dr. Val Jones in Health Tips, Opinion, Research
No Comments »
 We’ve known for quite some time that weight loss can reduce the risk of developing insulin resistance and type 2 diabetes. However, a healthy diet alone (without weight loss) may also help to reduce risk. In a recent Spanish study (published in the Annals of Internal Medicine), 3,541 men and women ages 55-80 at risk for diabetes were followed for an average of 4.1 years. Those who ate a diet rich in fish, whole grains, fruits, vegetables, and olive oil were less likely to develop diabetes than those following other diets of similar caloric value.
We’ve known for quite some time that weight loss can reduce the risk of developing insulin resistance and type 2 diabetes. However, a healthy diet alone (without weight loss) may also help to reduce risk. In a recent Spanish study (published in the Annals of Internal Medicine), 3,541 men and women ages 55-80 at risk for diabetes were followed for an average of 4.1 years. Those who ate a diet rich in fish, whole grains, fruits, vegetables, and olive oil were less likely to develop diabetes than those following other diets of similar caloric value.
This is interesting for a few reasons. First of all, it provides us with insight into the importance of what we eat (and not just how much we eat) for optimum health. When considering how to follow a Mediterranean diet, I think it might be easiest to focus on what is NOT on the menu, rather than what we need to add to our diet. Notice that the Mediterranean diet has very low sugar, refined carbohydrates, processed foods and animal fat (with the exception of fish oil). This is not a low carb or low fat diet. It is a low glycemic-index and unprocessed food diet.
Secondly, calorie-restriction alone may not be the optimal way to reduce the risk of developing type 2 diabetes. In the past we have focused primarily on fat loss for diabetes prevention – through calorie restriction and exercise. We’ve often heard that “a calorie is a calorie” and that folks can lose weight effectively on a low-carb, low-fat, or high protein diet. While it’s true that studies have been equivocal regarding the most effective type of diet for weight loss, and people have been able to lose weight on everything from a bacon and grapefruit to a cookie diet, a deeper look suggests that certain diets really are healthier for us in the long run.
Thirdly, what we eat can have a profound effect on our health, and food is an easily modifiable risk factor for illness. Unlike many diseases and conditions (such as type 1 diabetes and other autoimmune disorders) where we have little to no control over whether or not we contract them, it is exciting to know that a healthy diet is a powerful weapon against disease that does not rely on pharmaceutical products or medical interventions.
And finally, I found this study interesting because it confirms what I have noticed in my own life recently – that cutting out refined carbohydrates and sugars can have a very positive effect on body composition and overall health. I have always had a very difficult time with hunger during calorie restriction, and I finally realized that it had to do with being sensitive to blood sugar spikes and drops from too many refined carbs. Once I cut out all added sugars and white flours from my diet (replacing them with lean protein and whole grains) my chronic hunger resolved and I could settle in to a comfortable relationship with food without constantly battling the scale.
If you haven’t tried the Mediterranean diet, there’s no time like the present. While evidence suggests you’ll be healthier for it, my experience tells me you’ll feel a whole lot better too. Say goodbye to the food craving and hunger cycle, and hello to a new way of healthy eating that can be comfortably maintained for a lifetime.
 If you have not read the latest essay and editorial about scandalous physician behavior published in the Annals of Internal Medicine (AIM), you must do so now. They describe horrific racist and sexist remarks made about patients by senior male physicians in front of their young peers. The physicians-in-training are scarred by the experience, partially because the behavior itself was so disgusting, but also because they felt powerless to stop it.
If you have not read the latest essay and editorial about scandalous physician behavior published in the Annals of Internal Medicine (AIM), you must do so now. They describe horrific racist and sexist remarks made about patients by senior male physicians in front of their young peers. The physicians-in-training are scarred by the experience, partially because the behavior itself was so disgusting, but also because they felt powerless to stop it.

 Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A
Wear and tear on the knee joints creates pain for up to 40% of Americans over age 45. There are plenty of over-the-counter (OTC) and prescription (Rx) osteoarthritis treatments available, but how effective are they relative to one another? A 

 We’ve known for quite some time that weight loss can reduce the risk of developing insulin resistance and type 2 diabetes. However, a healthy diet alone (without weight loss) may also help to reduce risk.
We’ve known for quite some time that weight loss can reduce the risk of developing insulin resistance and type 2 diabetes. However, a healthy diet alone (without weight loss) may also help to reduce risk. 









