October 21st, 2013 by Dr. Val Jones in Opinion
9 Comments »
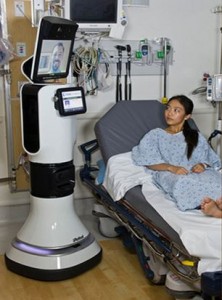
A "Medical Service Provider"
As I sat in my orthopedist’s exam room, the discussion quickly turned from my chief complaint to his: “I don’t know why I’m doing this anymore,” he said. “Medicine is just not what it used to be, and I don’t enjoy my work anymore. The bureaucracy and regulations are bad enough, but what really gets me is the hostility. My patients are chronically angry and mean. The only comfort I get is from talking to other doctors. Because they all feel the same way.”
Perhaps this sentiment strikes you as the spoiled musings of a physician who is lamenting his demotion from “god” to “man” – reflecting the fundamental change in the public perception of doctors that has occurred over the past ~50 years. Or maybe you wonder if this surgeon’s patients are mean because he is a bad doctor, or isn’t respectful of their time? Maybe he deserves the hostility?
I’ve found this particular surgeon to be humble, thoughtful, and thorough. He is genuinely caring and a proponent of conservative measures, truly eager to avoid surgical procedures when possible. He is exactly what one would hope for in a physician, and yet he is utterly demoralized. Not because of the hours of daily documentation drudgery required by health insurance and government regulators, but because the very souls he has been fighting to serve have now turned on him. Their attitudes are captured in social media feeds on every major health outlet:
Doctors? I no longer afford that kind of respect: I call them “medical services providers.” They and their families and the medical cabal created this mess when they got control of med schools so that the wealth of a nation would remain in the hands of a few medical elites and their families. The very notion that doctors are smarter, more productive, more anything than others is ludicrous. They are among the worst sluff-offs of our society, yet the richest at the same time. It is an unreal world they have created themselves and they are now watching the natural outcome of such a false system.
The very best physicians have always been motivated primarily by the satisfaction of making a difference in their patients’ lives. That drive to “help others” is what makes us believe that all the sacrifices are worth it – the years of training, the educational debt, the lack of sleep, the separation from family, the delay (and sometimes denial) of becoming a parent, the daily grind of administrative burden, the unspeakable emotional toll that death and disease take on your heart… All of that is offset by the joy of changing and saving lives. But when that joy is taken from you, what remains is despondency and burn out.
What patients need to realize is that they have been (and still are) the primary motivator of physician job satisfaction. Patients have the power to demoralize us like no one else – and they need to take that power very seriously. Because if negative attitudes prevail, and hostility spreads like a cancer in our broken system, the most caring among us will be the first to withdraw.
And in the end all that will be left is “medical service providers.”
November 21st, 2012 by Dr. Val Jones in Health Policy, Opinion
No Comments »
 In a recent post entitled, “The Joys Of Health Insurance Bureaucracy” I described how it took me (a physician) over three months to get one common prescription filled through my new health insurance plan. Of note, I have still been unable to enroll in the prescription refill mail order service that saves my insurer money and (ostensibly) enhances my convenience. The prescription benefits manager (PBM) has lost three of my physician’s prescriptions sent to them by fax, and as a next step have emailed me instructions to complete an online form so that they have permission to contact my physician directly (to confirm the year’s refills). Unfortunately, page one of the form requires you to fill in your drug name and match it to their database’s list before you can continue to page two. For reasons I can’t understand, my common drug is not in their database. Therefore, I am unable to comply with my insurer’s wish that I enroll in mail order prescription refills. This will further delay receipt of my medication – and probably increase my cost as I will be penalized for not opting into the “preferred” mail order refill process.
In a recent post entitled, “The Joys Of Health Insurance Bureaucracy” I described how it took me (a physician) over three months to get one common prescription filled through my new health insurance plan. Of note, I have still been unable to enroll in the prescription refill mail order service that saves my insurer money and (ostensibly) enhances my convenience. The prescription benefits manager (PBM) has lost three of my physician’s prescriptions sent to them by fax, and as a next step have emailed me instructions to complete an online form so that they have permission to contact my physician directly (to confirm the year’s refills). Unfortunately, page one of the form requires you to fill in your drug name and match it to their database’s list before you can continue to page two. For reasons I can’t understand, my common drug is not in their database. Therefore, I am unable to comply with my insurer’s wish that I enroll in mail order prescription refills. This will further delay receipt of my medication – and probably increase my cost as I will be penalized for not opting into the “preferred” mail order refill process.
Now, all of this is infuriating enough on its own, but the larger concern that I have is this: How many patients are not “compliant” with their medication regimen because of problems/delays with their health insurer or PBM? Physicians are being held accountable for their patients’ medication compliance rates, even receiving lower compensation for patients who don’t reach certain goals. This is called “pay-for-performance” and it’s meant to incentivize physicians to be more aggressive with patient follow up so that people stay healthier. But all the follow up in the world isn’t going to get patient X to take their medicine each day if their health insurer or PBM makes it impossible for them to get it in the first place. And shouldn’t there be consequences for such excessive red tape? Who is holding the insurers and PBMs accountable for their inefficiencies that prevent patients from getting their medicines in a timely manner?
Pay-for-performance assumes that physicians are the only healthcare influencers in the patient compliance cycle. I’ve learned that we only play a part in helping people stay on the best path for their health. Other key players can derail our best intentions, and it’s high time that we look at the poor performance of health insurers and PBMs as they often block (with intentional bureaucracy) our patients from getting the medicine they need. While insurers save money by having patients struggle to get their prescriptions filled, doctors are payed less when patients don’t take their medicines.
Not a great time to be a doctor or a patient… or both.
September 23rd, 2012 by Dr. Val Jones in Health Policy, Opinion
2 Comments »
 In another example of government over-reach, the NYT describes how the Obama administration is enlisting the help of patients to report physicians (whom they believe may have made a medical error), directly to the federal government. While there are systems already in place for such reports at the local hospital level, apparently the “under reporting of medical errors” has triggered AHRQ to pilot a program in which questionnaires are sent to patients to ferret out potential examples of errors caused by the following:
In another example of government over-reach, the NYT describes how the Obama administration is enlisting the help of patients to report physicians (whom they believe may have made a medical error), directly to the federal government. While there are systems already in place for such reports at the local hospital level, apparently the “under reporting of medical errors” has triggered AHRQ to pilot a program in which questionnaires are sent to patients to ferret out potential examples of errors caused by the following:
* “A doctor, nurse or other health care provider did not communicate well with the patient or the patient’s family.”
* “A health care provider didn’t respect the patient’s race, language or culture.”
* “A health care provider didn’t seem to care about the patient.”
* “A health care provider was too busy.”
* “A health care provider didn’t spend enough time with the patient.”
* “Health care providers failed to work together.”
* “Health care providers were not aware of care received someplace else.”
So if a patient determines, for example, that a physician did not spend enough time with them, and they believe that resulted in a medical error (whatever that might be), they can/should report the physician to the federal government. Wow. One physician explains the potential hazards of such a process:
Dr. Kevin J. Bozic, the chairman of the Council on Research and Quality at the American Academy of Orthopaedic Surgeons, said it was important to match the patients’ reports with information in medical records.
“Patients’ perceptions and experience of care are very important in assessing the overall success of medical treatments,” Dr. Bozic said. “However, patients may mischaracterize an outcome as an adverse event or complication because they lack specific medical knowledge.
“For instance, a patient may say, ‘I had an infection after surgery’ because the wound was red. But most red wounds are not infected. Or a patient says, ‘My hip dislocated’ because it made a popping sound. But that’s a normal sensation after hip replacement surgery.”
I believe that reporting medical errors is critical in the process of quality improvement, but that is most efficiently handled at the hospital level. There is no need to involve the federal government at the earliest stages of investigation, and the amount of bureaucracy required to support such an effort boggles the mind.
In the past when I encountered medical errors in the hospital setting, I found successful ways to report the incidents to the local administration. The result was a rapid correction of the problems and new processes put in place to ensure that it didn’t happen again. This is how medical errors should be reported and resolved. Soliciting patients for accounts of subtle lapses in social graces by their healthcare providers, and then reporting them to the government for it, is nothing short of Big-Brother creepy.
December 31st, 2011 by DrWes in Health Policy, Opinion
1 Comment »

It is tough playing man-to-man when coaches on the sideline keep insisting your team plays zone.
Such is it with health care.
For doctors, the man-to-man defense never ends. Stay with them. Glue to them. Move with them. Run with them. Defend against the bounce pass, or the dribble to avoid the admission. Hands up! Watch their waist, ignore the head fake. You shift your coverage to accommodate their needs. One on one, mana-a-mano.
But for the business of medicine, it’s all about the zone. Defend the admission basket against as many people as possible with the least number of defenders. Stay in your position. Work it 2-1-2, 2-3, or if you’re really adventurous: 1-2-2. Stick to Read more »
*This blog post was originally published at Dr. Wes*
December 26th, 2011 by Debra Gordon in Opinion
No Comments »

One of the hot phrases in health care these days is “patient-centered,” as in “patient-centered hospitals,” “patient-centered practices,” and “patient-centered medicine.” For all of you out there working on creating such “patient-centered” systems, let me provide a bit of advice based on a recent experience my family and I had with Delta Airlines. For if you substitute the word “customer” for “patient,” you get what every business, whether in health care or not, should be focused on — the person receiving, nay, purchasing, their services. The ones you hope will return, again and again.
I’m actually writing this as I sit in the lobby of a hotel in Park City, Utah. It is a gorgeous day outside, crisp and cold, just perfect for the skiing my family had in mind when we booked this trip; it’s a short trip– just 3 days on the slopes before we head home — so every minute counts. Unfortunately, despite plenty of time sitting in airports yesterday (i.e., no tight connection), only 2 out of our 6 pieces of luggage made it here. Fortunately, one of those was the suitcase filled with skiing togs. Unfortunately, one of the missing pieces was my son’s new snowboard, also filled with all of his ski togs. So while my boys are out on the slopes (the snowboard kid wearing my ski clothes), I’m sitting in the lodge awaiting our luggage. It is nearly noon — half of the day gone, one-sixth, possibly one-third, of our vacation gone–and I have not yet set foot on the slopes. Sure, I could head over and buy all-new ski stuff. . . . but that isn’t the point.
The point is how this was handled. Read more »
*This blog post was originally published at A Medical Writer's Musings on Medicine, Health Care, and the Writing Life*



 In a recent post entitled, “
In a recent post entitled, “ In another example of government over-reach, the
In another example of government over-reach, the 









